Advanced Therapies for Wound Management: The Role of Collagen
February 27, 2020
Wound chronicity is an ongoing challenge for patients and health care professionals around the globe. An astonishing 4.5 million people in the United States experience lower extremity wound chronicity, while an estimated 1% are affected in the Western population with all types of chronic wounds.1 The cascade of wound healing does not always follow suit in an orderly fashion of hemostasis, inflammation, proliferation, and remodeling. Chronic wounds become "stalled" in the inflammatory phase developing an increase of proteolytic enzymes with degradation of the extracellular matrix (ECM). This wound environment transforms into a hyperinflammatory and proteolytic state that prevents the wound from progressing further into the wound healing continuum.1
Biofilm is one of the main factors in delayed wound healing, with 60% of chronic wounds containing biofilm. Biofilm management has been proven to support wound healing in challenging wound chronicity of various etiologies.1 Biofilm management is a proactive approach that includes two important key elements: sharp and/or surgical debridement, and utilizing a broad-spectrum, noncytotoxic, antimicrobial product.2 Recent case studies have validated utilization of a purified collagen matrix (PCMP) coated with polyhexamethylene biguanide (PHMB) to various wound etiologies, nonhealing, and recalcitrant type wounds. This technology enables resistance of proteolytic degradation, while providing a sustained antimicrobial effect.1
Collagens in Wound Care Products
The most abundant protein in the body is collagen. The role of collagen in wound healing is to attract fibroblasts and encourage deposition of new collagen to the wound bed. Collagen dressing technology helps stimulates new tissue growth, while encouraging autolytic debridement, angiogenesis, and reepithelialization. Chronic wounds develop excessive matrix metalloproteinases (MMPs) that interfere with the normal wound healing process. Collagen dressings bind and inactivate excessive MMPs found within the extracellular matrix (ECM). Some collagen technologies have been paired with additional ingredients such as alginate, hydrogel, silver, polyhexamethylene biguanide (PHMB), carboxymethyl cellulose (CMC), and ethylenediaminetetraacetic acid (EDTA).4
Collagen dressings are primary dressings used in direct contact with the wound bed and containing live tissue. Collagen is derived from animal sources such as bovine (cow), equine (horse), porcine (pig) and avian (bird). These dressings can be used on granulating wounds with minimal to heavy exudate. Collagen dressings absorb exudate while providing an optimal moist environment to enhance healing. Collagen dressings are available in sheets, particles, amorphous gels, and pads.4
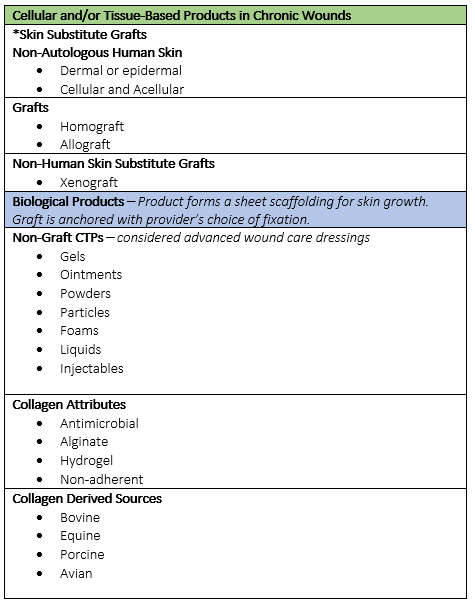
Cellular and/or Tissue-Based Products (CTPs)
Cellular and/or Tissue Based Products (CTPs), also known as skin substitutes, and biological products were primarily developed due to problems encountered with allografts (skin from another human) and xenografts (skin from another species).5 Skin substitutes facilitate healing and regeneration for chronic wounds. These products work by applying the product over the entire wound surface area providing extracellular matrices to encourage immune function and tissue regeneration. Skin substitutes can be used on patients with lower limb diabetic ulcers, venous ulcers, burn wounds, surgical and traumatic wounds (e.g., donor sites and graft, post laser surgery, and post podiatric surgery).6
Growth Factors
Growth factor Becaplermin gel is human derived protein that is not systemically absorbed and does not develop neutralized antibodies. Becaplermin promotes wound healing by enhancing granulation tissue formation. Faster healing rates have been shown with this specific growth factor.3

Collagen Dipeptides Supplement
Collagen dipeptides are highly concentrated Proline-Hydroxyproline (PO) and Hydroxyproline-Glycine (OG) that reach the cellular level in the skin, bones, and joints. The PO and OG send signals to cells, energizing the collagen peptide production by fibrocytes and chrondrocytes to promote growth of hyaluronic acid, aiding in wound healing.7
Payment Rates and Reimbursement Considerations
CTPs in chronic wounds may be billed by providers for chronic wound care patients in the hospital outpatient setting using one or more HCPCS codes per hospital outpatient prospective payment system (OPPS). Skin substitutes and biological products are divided into two groups regarding application procedure payment: 1) High cost skin substitute products, and 2) low cost skin substitute products for packaging purposes. It is imperative that documentation meets specific criteria and sets the standard in reimbursement of advanced wound care dressings and biologicals for payment. This includes the physician order, patient history and physical, diagnostic test results, implemented treatment plan, clinical documentation, and specific codes to validate reimbursement.
Medicare Part B will cover surgical (wound) dressings that are deemed medically necessary for the treatment plan. There may be copayments and deductibles to consider. The OPPS drives payment rates for hospital outpatient facilities, physicians, providers and suppliers billing Medicare administrative contractors (MACs) for hospital outpatient services provided to patients with Medicare benefits.8
Conclusion
The primary goal in chronic wounds is ultimately reepithelialization or wound closure. Sharp debridement removes biofilm, but biofilm begins to reform within 24 hours. We must optimize different strategies in biofilm management to promote wound closure. Combining biofilm management and advanced wound care technologies will support healing and good outcomes in the chronic wound population.
Reference
1. WOUNDS Journal. Effect of a New Purified Collagen Matrix with Polyhexamethylene Biguanide on Recalcitrant Wounds of Various Etiologies: A Case Series. Issue: Volume 30 – Issue 3. ISSN: 1044-7946. March 2018;30(3):72-78 https://www.woundsresearch.com/article/effect-new-purified-collagen-mat…
2. A comprehensive biofilm-based management approach; Improving standard care for all wound types. Gregory Schultz, PhD. University of Florida https://organogenesis.com/pdf/advanced-wound-care-bbwm-perspective-pape…
3. Regranex (becaplermin) gel 0.01% [prescribing information]. Raritan, N.J.: Ortho-McNeil Pharmaceutical, Inc.; 2005. http://www.regranex.com/content/backgrounders/www.regranex.com/www.regr….
4. What you need to know about collagen wound dressings. (2017, April 07). Retrieved January 19, 2020, from https://woundcareadvisor.com/what-you-need-to-know-about-collagen-wound…
5. Debels et al., 2015; Ferreira et al., 2011; Nicholas et al., 2016; Vig et al., 2017
6. Hayes, Skin Substitutes for Chronic Foot Ulcers in Adults with Diabetes Mellitus: A Review of Reviews, November 2018; Nicholas et al., 2016
7. Push Collagen Dipeptide Concentrate: Wound Care Supplement. https://globalhp.com/shop/push-collagen-dipeptide-concentrate/
8. Medicare Learning Network (MLN) January 2019 Update of the Hospital Outpatient Prospective Payment System (OPPS). https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-ML…;
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










Follow WoundSource
Tweets by WoundSource