Ulcerative Wound Symptoms: Identifying Wound Etiology
January 2, 2020
Open wounds in the skin are generally referred to as "ulcers" and can have a variety of etiologies. Ulcerative wound types include venous, arterial, diabetic neuropathic, and pressure. To identify ulcer types, these wounds should be examined thoroughly for their distinct characteristics such as location and shape, as well as in conjunction with other patient information, to ensure an accurate diagnosis and treatment plan.
Venous Ulcers
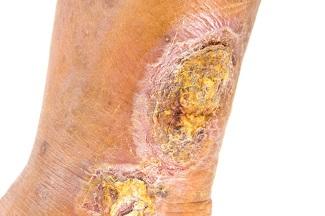
Venous ulcers are commonly caused by chronic venous insufficiency or the improper functioning of the one-way valves in the veins that prevent the proper flow of blood back to the heart. Blood pools in the lower part of the legs, thereby increasing the pressure around the capillaries and preventing oxygen and nutrients from reaching muscle and skin tissue, a process that results in cell death and the formation of an ulcer.1
Characteristics1–3
- Large, but shallow wound
- Red color, with potentially yellow fibrous tissue involved
- Located in the gaiter area, one inch below the knee to above the malleolus
- Irregularly shaped wound margins
- Presence of a moist, granulating base
- Surrounding tissue possibly showing signs of stasis dermatitis
- Mild pain and swelling unless infected
- Symptoms eased when legs are elevated
- Pruritus
- Papillomatosis, or the presence of tiny rough bumps
Venous ulcers commonly occur in individuals with a history of varicose veins, high blood pressure, blood clotting disorders, deep vein thrombosis, or heart failure. They may also occur in patients who are pregnant or who have experienced trauma, fractures, or injuries to the area.4
Arterial Ulcers
Arterial ulcers, sometimes referred to as ischemic ulcers, are commonly caused by blocked arteries that prevent the flow of oxygen and nutrients to tissue. As in venous ulcers, the lack of oxygen and nutrients causes cell death and the formation of an open wound. Characteristics1,2,4–6
- Usually located on feet, heels, or toes
- Deep, full-thickness wound
- Punched-out appearance
- Tight, hairless skin
- Pain, often worsening at night
- No bleeding or bleeding only during debridement
- Cool to the touch (minimal circulation)
- Lower limbs possibly turning red when they are dangling over the side of the bed, but pale when elevated
- Swelling
- Minimal drainage
- Pale pink or gray wound bed
Arterial ulcers commonly occur in older patients, patients with diabetes, or those with vasculitis, high cholesterol, and high blood pressure. Higher-risk patients may also have a history of smoking, kidney failure, atherosclerosis, or trauma to the area.4
Diabetic (Neuropathic) Ulcer
Diabetic ulcers resemble arterial ulcers but are more commonly located over pressure points, such as the heels, plantar aspect, or the tips of the toes. They may also occur between the toes or over bony prominences that experience friction. Characteristics5,6
- Usually occurring at the bottom of the feet, over pressure points, on the heels or toes
- Appearance possibly ranging from pink or red to brown and black
- Presence of neuropathy (numbness, tingling, or burning sensation)
- Hyperkeratosis or fibrotic rimmed wound edges
- Punched-out appearance
- Surrounding tissue possibly inflamed
Diabetic ulcers often worsen because of the presence of neuropathy, which can increase mechanical stresses on the foot.
Pressure Injury
Pressure injuries commonly occur in individuals with limited mobility, such as those confined to bed rest or those who may need a wheelchair. The pressure is caused by the weight of the body being in one position for extended amounts of time or in conjunction with friction, shearing, and/or moisture. One or more extrinsic factors will eventually damage the surface of the skin. Left untreated, this damage will worsen, and an injury will develop. Pressure injuries are commonly classified into six stages. The staging system was developed to determine the tissue level of destruction. Characteristics
- Stage 1 pressure injuries are intact. The patient presents with red and non-blanchable skin. Changes in sensation, temperature, and firmness may precede visual changes. Pressure injuries in patients with darker skin tones may appear differently.
- Stage 2 pressure injuries are partial-thickness wounds. The wound is shallow and is red or pink. There is no granulation tissue present in a stage 2 pressure injury. There also may be a serum-filled blister with this stage.
- Stage 3 pressure injuries are full-thickness wounds. There may be granulation, slough, or eschar present in this stage. Adipose tissue may or may not be visible. Undermining may occur during this stage. There is no exposed structure such as muscle, tendon, fascia, bone.
- Stage 4 pressure injuries are full-thickness wounds. Depth depends on anatomical location. There is exposed structure such as muscle, tendon, fascia, and bone. Undermining and tunneling may be present.
- Unstageable pressure injuries are not staged because the wound bed is not visible. The wound is covered with slough or eschar. Once the wound bed is visible, the wound can be appropriately staged.
- Deep tissue pressure injuries can be intact or non-intact. The injury is localized, with persistent non-blanchable, deep red, maroon, or purple discoloration, or epidermal separation revealing a blood-filled blister.
Conclusion
Identifying wound etiology is not always straightforward when looking at wound location and characteristics. Clinicians should remember to perform a thorough assessment involving the patient. Ask questions, and listen to your patient because that interaction may give you valuable information to help your patient heal their wound.
References
1. Ngan V. Leg ulcer. DermNet NZ; 2004. https://www.dermnetnz.org/topics/leg-ulcer/. Accessed November 29, 2019.
2. London Health Sciences Centre. Venous stasis and arterial ulcer comparison. 2019. https://www.lhsc.on.ca/wound-care-management/venous-stasis-arterial-ulc…. Accessed November 29, 2019.
3. Finlayson K, Miaskowski C, Alexander K, et al. Distinct wound healing and quality-of-life outcomes in subgroups of patients with venous leg ulcers with different symptom cluster experiences. J Pain Symptom Manage. 2017;53(5):871-879.
4. Healthline. Arterial and venous ulcers: what’s the difference? https://www.healthline.com/health/arterial-vs-venous-ulcers; 2018.
5. Cleveland Clinic. Leg and foot ulcers. 2019. https://my.clevelandclinic.org/health/diseases/17169-leg-and-foot-ulcers. Accessed November 29, 2019.
6. Gabriel A. Vascular ulcers. 2018. Medscape.com. .
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.











Follow WoundSource
Tweets by WoundSource