Self-Check for Health Care Providers
May 31, 2020
By the WoundSource Editors Health care providers are currently faced with an all-time high of challenges and strain related to the crisis of COVID-19. They are confronted with short staffing, limited personal protective equipment supplies, delegated duties outside their role, and the worry of being infected with the virus. There are health care workers who are not living at home because of the high risk of infecting their family members and others who are quarantining themselves within their homes away from their families. As health care workers focus on working hard on the frontlines for their patients, they must also remember to take care of themselves. Learning and applying self-care practices are just as important to ensure that health care workers remain safe and healthy to optimize delivery of care for their patients.
Mnemonic Self-Check Screening for Health Care Providers
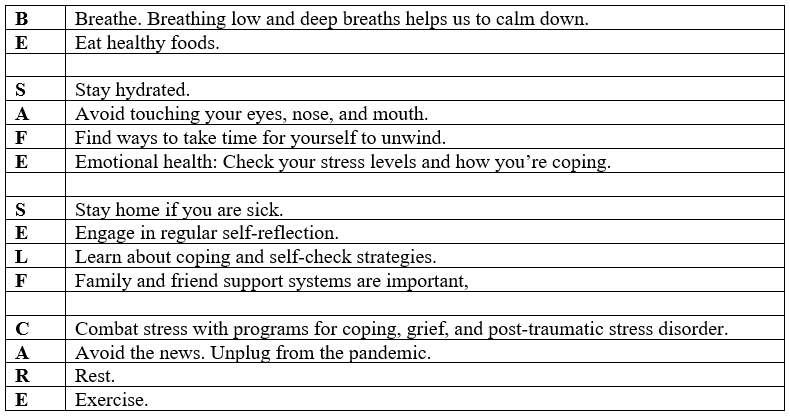
During this crisis, demands are increasing, and many people have already had to move away from their normal routines. It is critical to try as much as possible to maintain structure within your routine. Our body reacts to the unstable “new.” There are various strategies to help manage anxiety, stress, and worry during this testing time. Ensuring you are taking care of yourself may include packing more food for breaks, using a larger water bottle, taking a 10-minute walk outside, and/or listening to a podcast on the way to and from work. Reach out to your support systems: family, friends, or other co-workers for emotional support. Utilize social media platforms, smartphone apps, and other technologies to connect with friends during this time of isolation.1 It is a common saying that health care providers make the worst patients and often have difficulty remembering to care for themselves. Health care workers need to be reminded that it is OK to reach out and ask for support. It is OK to take a break. Life is chaotic right now because of the pandemic, so plan time at home to rest and unwind. Read a good book, watch a movie, or listen to music. There are mindfulness exercise techniques to help recharge.1
Mental Health Signs to Watch for
An important reminder to all frontline workers is that we do not all react the same, and it is normal to experience different reactions to the current situation. There is no one “right way”; your reaction does not define you as weak. How one reacts to stress may vary, from feeling down, muscle tension, and difficulty sleeping, to amplified and persistent stressors. Health care workers who feel burnout, extreme fatigue, fuzzy thinking, increased irritability or anger and/or who begin to isolate or withdraw are experiencing warning signs of excessive stress.2 Post-traumatic stress disorder (PTSD) is a chronic psychiatric disorder that can develop in people who have experienced or witnessed trauma. Most of us think of war and/or physical assaults, but the COVID-19 pandemic is a traumatic event, too, and it may result in PTSD for some. There are already many health care workers experiencing symptoms PTSD. PTSD consists of nightmares, anger, fear, irritability, or intense flashbacks that can often coincide with anxiety and depression. Do not be afraid to ask for help if you are struggling to provide care to your patients, yourself, and/or your family the way you did before COVID-19. If these warning signs are worsening or are lasting for longer than three to four weeks, it is recommended to seek care with a mental health professional.3,4 If you are experiencing suicidal thoughts, please reach out to a mental health professional immediately, or call the national suicide prevention lifeline at 1-800-273-8255 (US only). There are various stress reactions when in crisis. Health care workers may feel like they are in control before the crisis, then when a pandemic develops everything spirals out of control emotionally and physically. Providers and health care workers should team up for support and remind each other that they are not alone. We are in this together. Connect with resources and other support systems during this time. Free Resources for Health Care Professionals2 National Suicide Prevention Lifeline 1-800-273-TALK (8255) https://suicidepreventionlifeline.org/ SAMHSA (Substance Abuse and Mental Health Services Administration) National Helpline 1-800-662 HELP (4357) https://www.samhsa.gov/find-help/national-helpline SAMHSA Disaster Distress Helpline 1-800-985-5990 https://www.samhsa.gov/find-help/disaster-distress-helpline Crisis Text Line Text HOME to 741741 https://www.crisistextline.org/
References 1. American Psychological Association Services, Inc. Self-care advice for health providers during COVID-19. https://www.apaservices.org/practice/ce/self-care/health-providers-covi…. Accessed May 3, 2020. 2. Rogers Behavioral Health. Self-care tips for healthcare workers on the frontlines of COVID-19. https://rogersbh.org/about-us/newsroom/blog/self-care-tips-healthcare-w…. Accessed May 3, 2020. 3. American Psychiatric Nurses Association. Managing stress & self-care during COVID-19: information for nurses. https://www.apna.org/i4a/pages/index.cfm?pageid=6685. Accessed May 3, 2020. 4. American Medical Association. Caring for healthcare workers during COVID-19. https://www.ama-assn.org/system/files/2020-04/caring-for-health-care-wo…. Accessed May 3, 2020.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.







