Understanding Diabetic Foot Ulcer Classification Systems
August 16, 2019
By the WoundSource Editors
In patients with diabetes, the lifetime risk of diabetic foot ulcers (DFUs) is approximately 25%, and these wounds are frequently a source of pain and discomfort. Severe cases can even result in amputation of a portion of or the entire affected extremity. Proper classification of DFUs is essential for selecting the appropriate treatment course and coordinating care for the patient. Several systems are frequently used in classifying DFUs, although there is no universally agreed-on standard.1
Diabetic Foot Ulcer Classification Systems
Wagner Diabetic Foot Ulcer Grade Classification System
The Wagner Classification System (sometimes referred to as Merritt-Wagner) was developed in the 1970s and comprises six ulcer grades, ranging from 0 to 5. This system assesses ulcer depth and the presence of osteomyelitis or gangrene.2 The grades are as follows3:
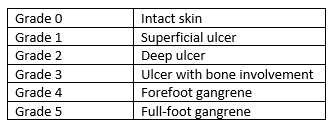
A recent study of classification systems found that despite its simplicity, the Wagner system was quite effective in predicting lower extremity amputation.1 Nonetheless, the United Kingdom's National Institute for Health and Care Excellence does not recommend using this classification system to assess DFUs because it does not adequately address all DFU subtypes and the spectrum of infections.3 Clinicians in the United States are still required to use the Wagner system when determining a patient’s candidacy for hyperbaric oxygen therapy; the DFU must be a Wagner grade 3 or greater for Medicare to reimburse for this indication.4
University of Texas Diabetic Foot Ulcer Classification System
Along with the Wagner Classification System, the University of Texas Diabetic Foot Ulcer Classification System has also proved effective at predicting lower extremity amputation.1 This system uses four grades (0–3) and four stages (A–D) to classify DFUs. The grades correspond to depth, whereas the stages account for the severity of the wound by marking the presence of infection, ischemia, or both.3 This classification system is frequently used in practice.
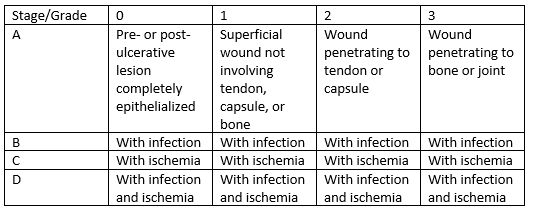
Diabetic Ulcer Severity Score (DUSS)
The Diabetic Ulcer Severity Score (DUSS) is based on the categorization of wounds into specific severity subgroups for a comparison of outcomes. Assessment using the DUSS system includes the presence of pedal pulses, the ability to probe to bone within the ulcer, and ulcer quantity and location. The sum of points determines severity, with the score ranging from 0 to 4.5
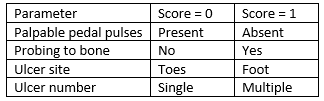
Site, Ischemia, Neuropathy, Bacterial Infection, and Depth (SINBAD) Wound Classification System
The SINBAD system uses five clinical features (site area, ischemia, neuropathy, bacterial infection, and depth), which are graded as either present (0) or absent (1). The maximum score is 6.6 A representation of this classification is as follows3:

Diabetic Foot Ulcer Classification System Overview
This overview contains some of the more frequently encountered classification systems for DFUs, although there are others, including the following6:
- S(AD) SAD system: This system uses five elements – size (area, depth), infection, ischemia, and neuropathy, and each element is scored from 0 to 3.
- PEDIS Classification: This system was designed by the International Working Group of the Diabetic Foot and uses the same five components of S(AD) SAD: perfusion, extent, depth, infection, and sensation. It does not include ulcer location.
- DEPA Classification: This system looks at four aspects of ulcers: depth, extent of bacterial colonization, phase of healing, and associated etiology. Each category is scored from 1 to 3 according to severity.
Lesser-known classification systems also include MAID, the CHS system, Margolis, Saint Elian Wound Score System, Van Acker/Peters, and Foster and Edmonds.6
Conclusion
Ultimately, all of these classification systems work toward grading the severity of the ulcer. These systems work as a tool for risk stratification and assessment and selection of the proper treatment course, which are crucial in achieving better patient outcomes.
References
1. Jeon B, Choi HJ, Kang JS, Tak MS, Park ES. Comparison of five systems of classification of diabetic foot ulcers and predictive factors for amputation. Int Wound J. 2017;14(3):537-545.
2. Swezey L. Diabetic foot ulcer classification systems. WoundEducators.com. 2016. https://woundeducators.com/diabetic-foot-ulcer/. Accessed July 25, 2019.
3. Stang D, Young M. Selection and application of a diabetic foot ulcer classification system in Scotland: part 2. Diabet Foot J. 2018;21(2):100-105.
4. Song E, Kuplicki S, Robinson S, Wong A. Diabetic foot ulcers - classification systems. In Shin L. ed. WoundReference. 2019. https://woundreference.com/app/topic?id=diabetic-foot-ulcers-classifica…. Accessed July 4, 2019.
5. Kumar ST, Arava S, Pavan BM, Kiran GCS, Chandan GB, Kumar NM. Diabetic ulcer severity score: clinical validation and outcome. Int Surg J. 2016;3(3):1606-1610.
6. Game F. Classification of diabetic foot ulcers. Diabetes Metab Res Rev. 2015;32(Suppl 1):186-194.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.







