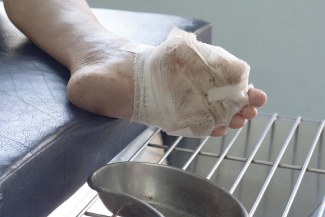
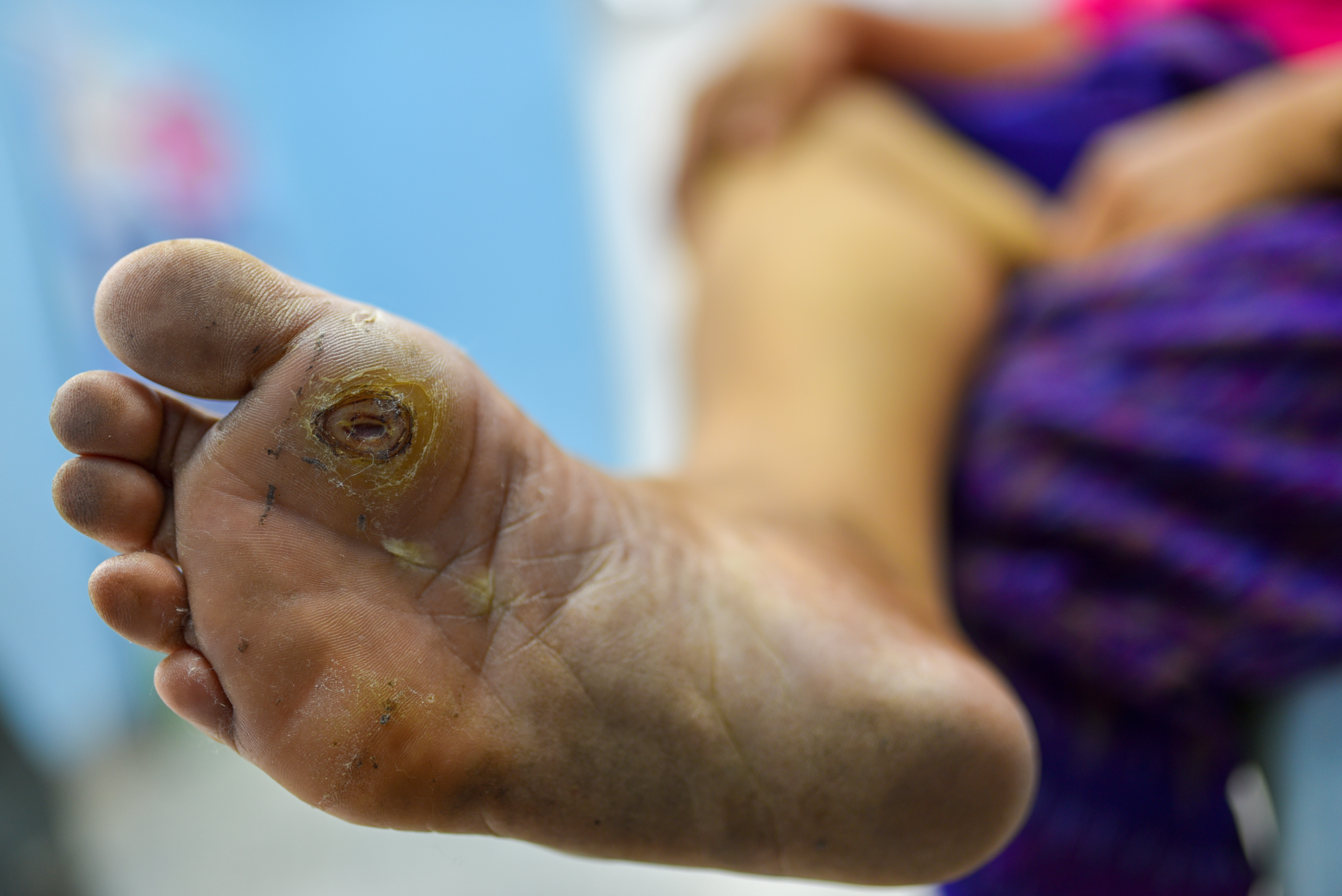
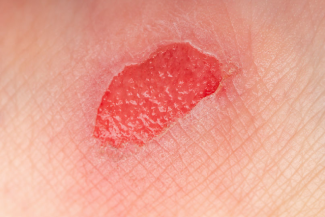
Why Won’t This Heal? Dealing With a Recalcitrant Wound: Part 1
March 25, 2022
Introduction
I’m sure we’ve all hit that point in our wound care careers where we’ve had that one patient who’s wound just doesn’t seem to respond to any treatment. You’ve tried everything that you can think of—state-of-the-art dressings, advanced cellular products, regular debridement, and even hyperbaric oxygen. But despite all of this, the wound seems stuck. This is what’s known as a recalcitrant wound, a wound that fails to progress through the phases of wound healing in a typical timeline and becomes “stuck.” A wound that does not decrease in size by 30% in 3 weeks or by 50% in 4 to 5 weeks is considered recalcitrant. This is significant because wounds that don’t show improvement in size by 50% in 4 weeks have a 91% chance of not healing in 12 weeks.1
A recalcitrant wound can be difficult to treat and can present a challenge for both the provider and the patient who has to live with it. How can clinicians overcome this impasse, to break past the point where the wound has stalled to initiate healing? For many, it can be helpful to take a step back and reassess. Go back to the patient’s original history and physical examination, and really look at some factors that may have led the wound to become recalcitrant. If the etiology of the wound was not discovered or properly addressed, this is an excellent place to start.
Signs of a Recalcitrant Wound
We know a wound is recalcitrant if it stalls in its healing progress, but are there other signs that this condition is occurring? Recalcitrant wounds tend to stall in the inflammatory phase of wound healing. This phase is often indicated by increased erythema, pain, edema, and heat to the area, caused by the increased vasodilation and increased capillary permeability that are hallmarks of this phase.2
These features are often mistaken for signs of wound infection, so it is important to observe the wound for other key features of nonhealing. Such signs can include the absence of beefy red granulation tissue, persistent slough, or a pale or white appearance. These wounds tend to be full thickness and may cause many complications, including chronic pain, increased changes of bleeding and/or infection, decreased mobility (particularly for lower extremity ulcers), and psychological issues, and they may have a higher chance of leading to amputation or even death.
Etiology
If you suspect the wound has become recalcitrant, what should you do? The first thing to do is to step back and reassess. Go back to the patient’s original history and physical and take a look at some factors that may have led to the wound to become recalcitrate. If the etiology of the wound was not discovered or properly addressed, this is an excellent place to start. Going back to the start ensures that the etiology of the wound has been addressed and is being treated. Inherently, the body strives toward healing, but there are often factors that prevent healing mechanisms from occurring. If a patient has untreated arterial insufficiency, a foot or leg wound is likely to stall.
If you have already addressed this, perhaps there’s a second undiagnosed wound etiology. Consider alternative diagnoses that may be leading to failure of the wound to heal. Wound perfusion is an essential factor in wound healing. If the underlying wound etiology is vascular, the wound may have hypoperfusion and therefore may not receive the basic flow of blood and oxygen it needs to progress toward healing. The underlying cause of ischemia will need to be reversed for the wound to improve. Some simple assessments for ischemia can include:
- Assessment of the site temperature
- Assessment of capillary refill, which that should be >3 seconds
- Assessment for dependent rubor, which can indicate poor arterial flow
If ischemia of the lower extremities is suspected, some basic tests for wound ischemia can include an ankle-brachial index, a toe brachial pressure index, or a computed tomography angiogram. Another possible wound etiology may be malignancy. These wounds fail to respond to conventional treatment and may baffle the most proficient provider. Malignant wounds tend to manifest as hypertrophic granulation tissue,3 so performing a biopsy can be an excellent way to check for this.
Dressings
A moist wound is a happy wound. If the dressing is not doing a good job in balancing moisture levels, the wound may become either too wet or too dry. Minimize the time a wound is left open to air because this can cool off and dry out a wound and thus significantly impede healing. If the wound has a dressing that doesn’t adequately absorb the exudate, this can lead to maceration and periwound skin breakdown.
Make sure that the dressing matches the amount of exudate of the wound. In addition to moisture control, an appropriate dressing will allow for thermic regulation. In other words, keeping a wound at body temperature will allow for it to heal more efficiently than if the wound was left exposed to the air. A wound’s natural moisture will lead to evaporative cooling once exposed to air and can dramatically decrease the wound’s temperature. According to Dr Stephen Thomas,4 the ideal dressing should maintain a core wound temperature of 37°C (98.6°F) with a relative humidity of 75%.
The dressing should also be gentle on the wound bed. Gone are the days of wet-to-dry mechanical debridement. Instead, look for dressings that are gentle, to prevent destroying delicate new capillary and granulation tissue formation. If the wound is in need of debridement, consider dressing types that allow for autolytic or enzymatic action, which can remove unwanted tissue while preserving healthy new growth.
Conclusion
In Part 1, we have discussed some clues that might indicate a recalcitrant wound. Signs of a recalcitrant wound can include:
- Stalled inflammation phase: erythema, pain, edema, and heat
- Persistent or increased exudate or slough/eschar
- Absence of granulation tissue
- Failure for wound progression
Determining the underlying cause of the wound will give you clues on how to help a recalcitrant wound towards healing. Explore undiagnosed potential conditions that may be the etiology of the wound. Assess for vascular flow, presence of underlying comorbidities, unrelieved pressure, or other possible reasons for the wound stall. Go back to your patient's history and physical and ask more questions to discover what you might not have seen during your initial exam. And finally, look at the dressings being used for the wound. Assess the amount of exudate and ensure the dressings are appropriate. Are the dressings causing trauma to the wound when removed? Are they allowing for proper temperature control?
There are many types of dressings that can be used, and if the one that is being used isn’t working, look at other options that may provide a better healing environment for the wound. In Part 2, we will continue our conversation about recalcitrant wounds by assessing for other factors that may cause a recalcitrant wound including infection, inflammation, the presence of necrotic tissue, edge effect, nutrition, and socio-economic factors. We will also discuss that some wounds that may never heal due to underlying comorbidities or complications.
References
- Widgerow AD. Deconstructing the stalled wound. Wounds. 2012;24(3): 58-66.
- Landén NX, Li D, Ståhle M. Transition from inflammation to proliferation: a critical step during wound healing. Cell Mol Sci. 2016;73(20):3861-3885. Accessed July 19, 2020. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5021733/
- Doughty D. Why won’t some wounds heal? Adv Skin Wound Care. 2004;17(7):342-344.
- Thomas, S. Surgical Dressings and Wound Management: A reference on the development, properties and clinic use of surgical dressings and modern wound management materials. 2nd Edition. Hinesburg, VT, Kestrel Health Information, Inc, 2012.
About the Author
Becky received her BSN from the University of Vermont where, along with a love of nursing, she picked up a love of hiking and cross-country skiing. She moved to Massachusetts and started to work as a med-surg nurse at a busy Boston hospital. There, she found that she loved mentoring new nurses and returned to school to earn her MSN as an acute care clinical nurse specialist from the University of Massachusetts, Boston. She followed her love of teaching into the acute, sub-acute and university settings, but she found that she missed working directly with patients. She returned to school and earned her Post-Master's Family Nurse Practitioner Certification from Rivier University. It was shortly after this that Becky discovered her love for wound care. She worked part time in wound care and part time in family care while she earned her WCC certification. After several years, Becky decided to take her practice to the next level by opening her own LLC and is currently seeing patients for wound care and regenerative medicine. Becky's philosophy of “Never stop learning” has guided her in her practice and life. Her very supportive husband and daughter are her key inspirations to keep growing and trying new things. In her spare time, Becky loves traveling with her family, going on long walks with her dog, Echo, and reading historical and science fiction.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.