Wound Care Patient Outcomes: Establishing Trust to Improve Wound Healing Results
September 6, 2018
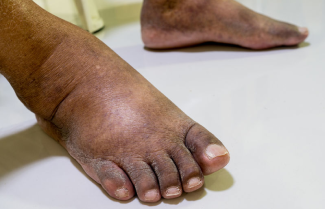
Last spring, I encountered that specific type of patient we sometimes meet, the one who has been through the chronic wound care revolving door so many times that he or she sets out on his or her own path and refuses any byways diverting from it. Ms. A had stage 3 lymphedema after a left knee replacement opened the hidden trap door of undiagnosed lymphedema several years before her admission to our inpatient rehab facility. Her reason for admission was debility from urinary tract infection (UTI). Comorbidities of obesity, severe arthritis of the right knee, diabetes, and chronic lymphedema wounds on both legs were exacerbating factors making discharge home difficult from the acute hospital.
Finding the Middle Ground
On assessment of her bilateral lower leg wounds, I noted a circumferential 25-cm long wound on the left leg and a 4cm × 3cm wound on the right leg. Both wounds were caked with a thick, whitish residue from her custom-compounded topical antibiotic. This was a cream that included antifungals as well as mupirocin, gentamicin, and vancomycin, among other agents. She also had 3+ pitting edema and Stemmer sign (+) on both legs. At this point I paused to reflect that my patient is a partner in her care. Ms. A explained to me on meeting that she was not in the inpatient rehab facility for her wounds, and thus she would like to continue her regimen from home care. She has been unable to tolerate debridement or Unna boots.
She anticipated having the wounds surgically debrided when she had regained her health. She would agree only to gentle cleansing of the wounds, reapplication of the compound, and absorbent bandaging twice per day. She could benefit from aggressive removal of the caked compound or biofilm, a non-adherent contact layer with ultra-absorbent or antimicrobial capability, compression wraps from toes to groin, and manual lymphatic therapy. (Insert sound of the shredding of my pie-in-the-sky treatment plan here.)
I agreed to honor her request to continue twice per day use of the compound and absorbent bandages. She agreed to cleansing with a hypochlorous cleanser, protection of periwound skin with a barrier cream, use of a self-adherent wrap to secure the bandages, elevating her legs in bed when not in therapies, and starting a program of manual lymphatic therapy. During this admission, she was able to reduce the volume of her legs and thus the frequency of dressing changes to daily. Ms. A was discharged home after 17 days with the wounds still caked, but on legs that were lighter and easier to move for her activities of daily living. This was an improvement, as she did not need twice per day dressing changes and had less of a burden of care for her family. She was very pleased with the wound and rehab care. She anticipated surgical debridement in the near future.
Achieving Results
However, not surprisingly, Ms. A was readmitted to our facility 13 days later with an acute hospital diagnosis of recurrent UTI.
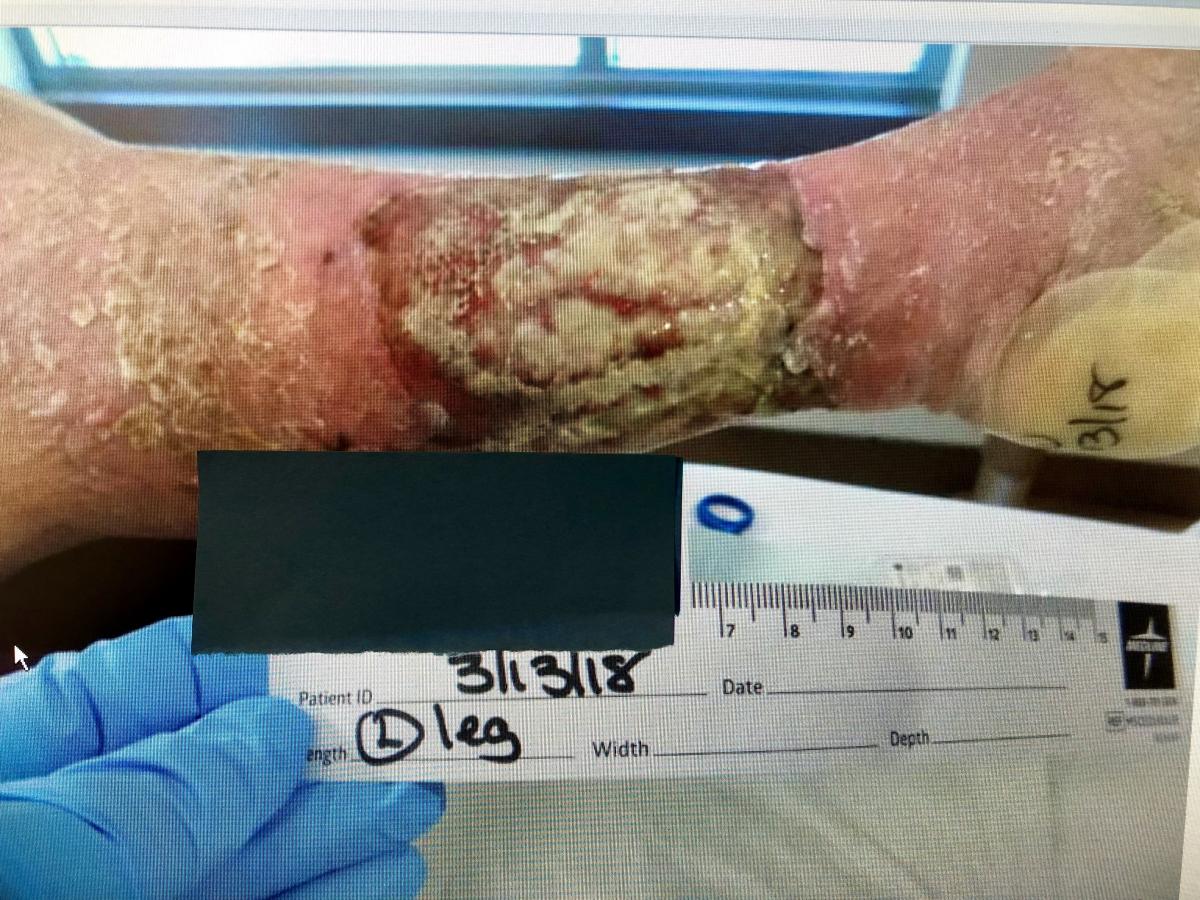
© Janet Wolfson. Used with permission.
The condition of her wounds was nearly the same but with less edema volume. The difference was in the trust that we had built during her first admission. I discussed another treatment option with her: negative pressure wound therapy (NPWT) with instillation and dwell with a new foam dressing. The contact foam had been developed specifically to clean large, complex wounds that could not be surgically debrided. She agreed based on our previous success and her own need to clean up the wounds and possibly avoid surgery. Ms. A tolerated the irrigation NPWT for three days but refused another application as removal of the dressing was painful. (Lesson learned from that: Remove right after the irrigation cycle.)
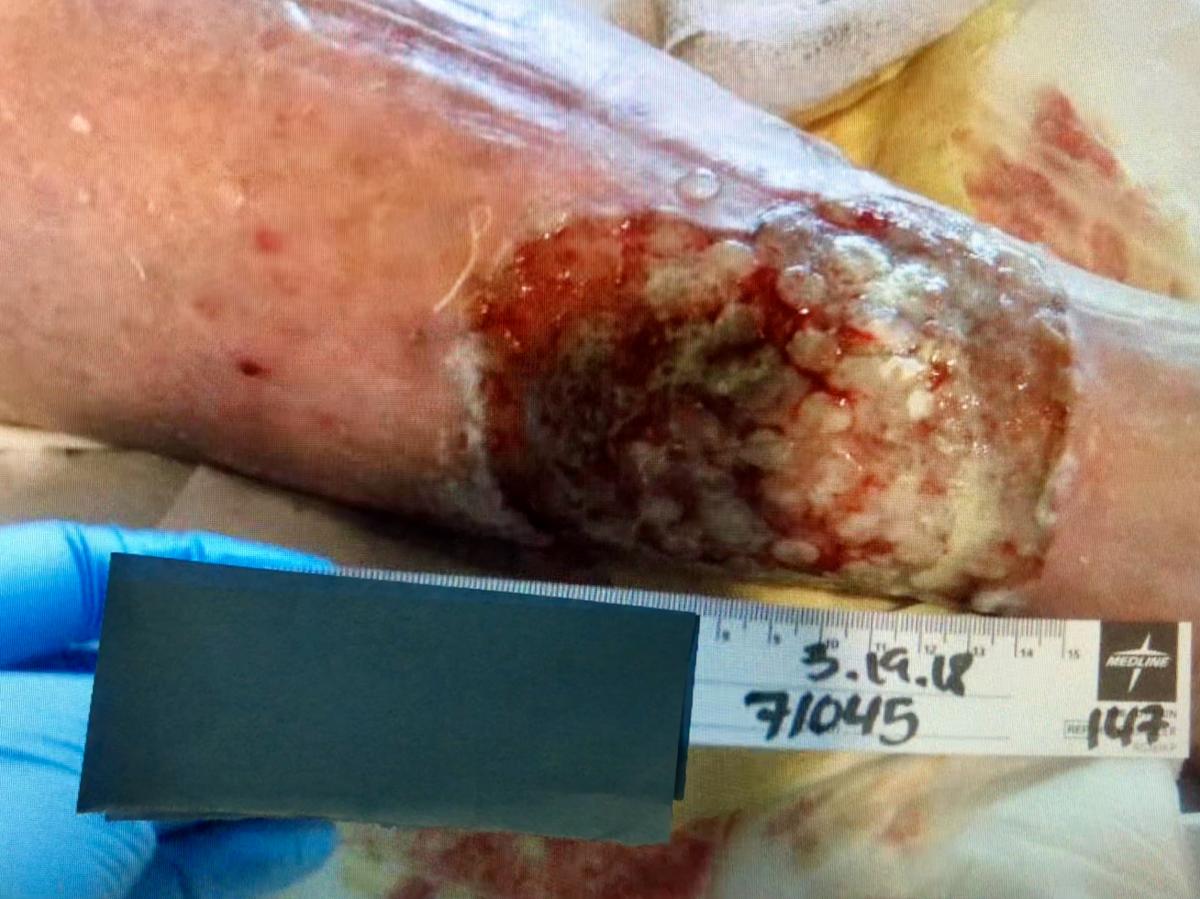
© Janet Wolfson. Used with permission.
The compression regimen was resumed with a non-adherent layer and a saline-moistened antimicrobial foam. On discharge after 15 days, this daily dressing change was reduced to every three days on a fully granulated wound bed.
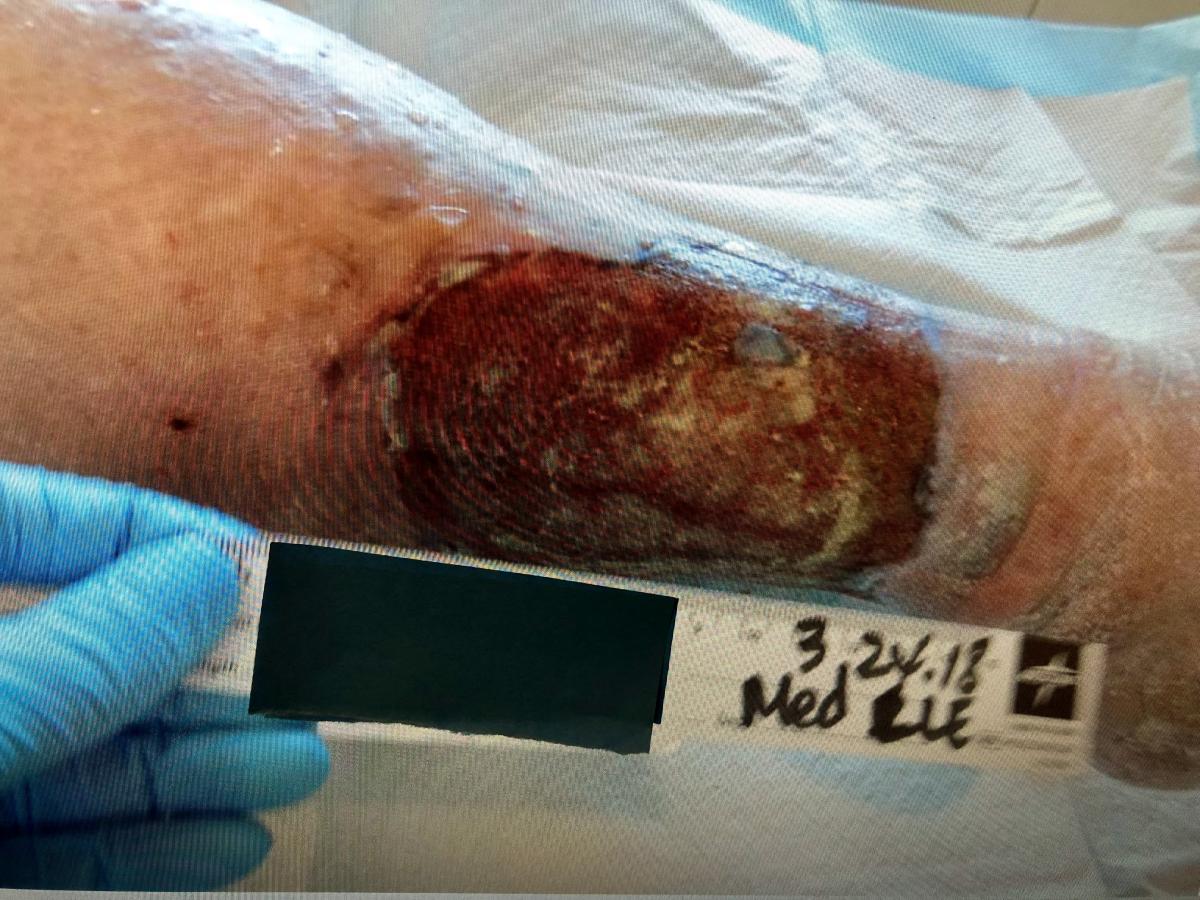
© Janet Wolfson. Used with permission.
Recently, Ms. A was visiting at our facility and stated that she had continued the protocol started during her stay with us and that she was nearly healed on the left leg. Lessons: Building trust is important, and the new instillation and dwell with the special dressing really, really works.
About the Author
Janet Wolfson is a wound care and lymphedema educator with ILWTI, and Lymphedema and Wound Care Coordinator at Health South of Ocala with over 30 years of field experience.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.