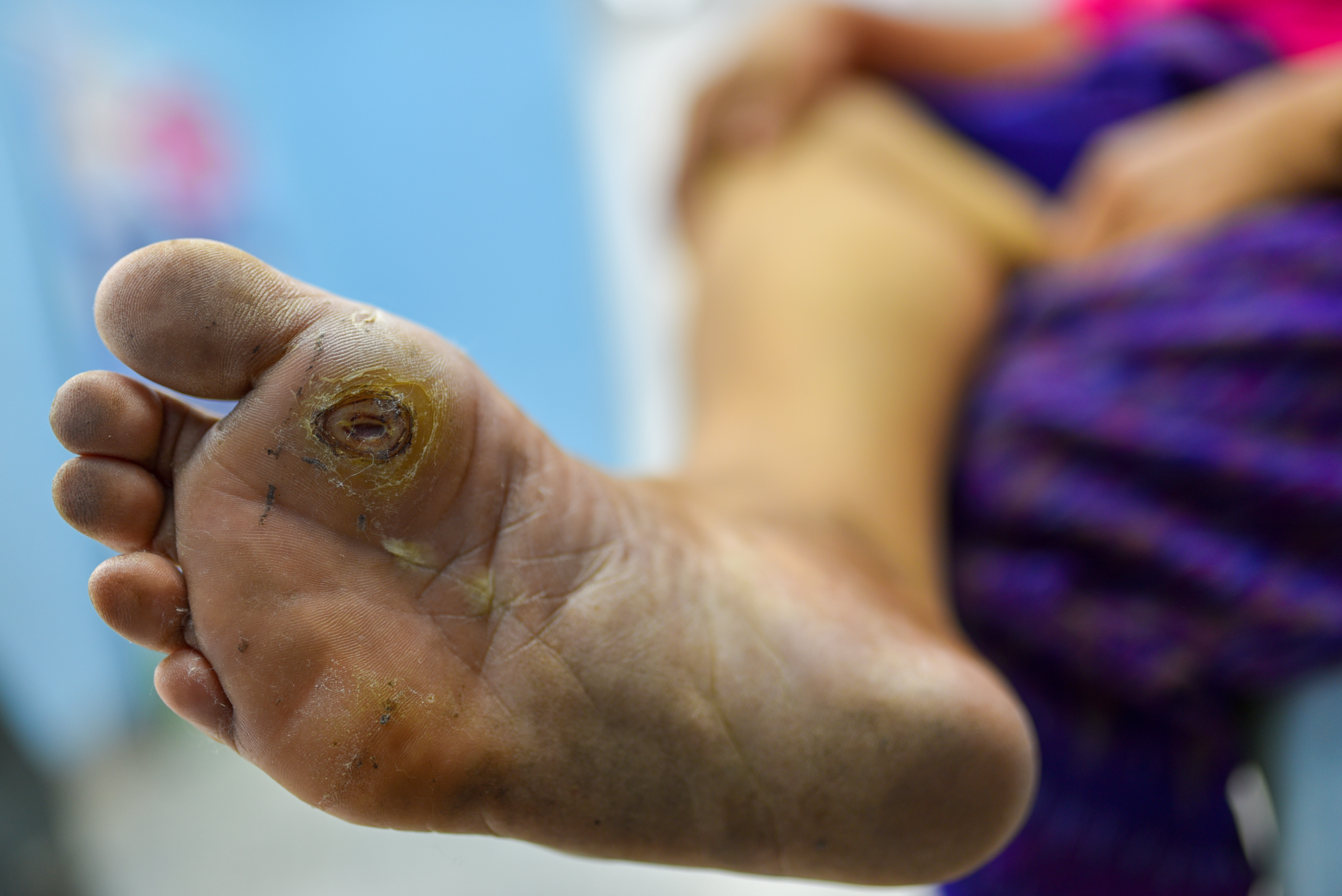
Wound Healing with Platelet-Rich Plasma
February 20, 2020
What if I told you that there is a substance that we can isolate from your own blood that can help to heal the most difficult wound? I envision a scene out of “Star Trek” where Bones does a quick scan of his patient, draws some blood, runs it through some machines, and then out pops a seemingly magical elixir. He studies this new yellow substance and then injects it back into his patient (with a quick and seemingly painless puff from his high-tech injector gun).
The patient (after a dramatic pause) wakes up from what seems like near death and quickly sits up and says something inspirational along the lines of “Things are only impossible until they're not"1, jumps off the table, and joins the crew for their next space adventure. Although this is fun and would be wild if we could actually do something like this, what if I told you that there actually is a treatment available right now that could really do something very much like this. This procedure is known as a platelet-rich plasma (PRP) injection and is currently being done in the United States and throughout the world for acute and chronic orthopedic injuries, aesthetics, restoring hair loss, and wound healing.
Mechanism and Clinical Experience in Wound Healing
PRP is a novel intervention where, much like Bones was able to heal his patient, we are able draw a vial of the patient's blood, spin it in a centrifuge to isolate the plasma, and then inject this into the problematic site.
I have actually been doing this, along with stem cell injections, for the last year to help with orthopedic issues at a local chiropractor's office, but recently I encountered a patient with a chronic gluteal cleft pilonidal cyst that had been recurrent over the last 40+ years despite treatment with advanced dressings and off-loading pressure from the site. The beauty of PRP is that it uses the body's own immune system to initiate a healing response, which can push a wound from the inflammatory phase to the proliferative phase. PRP is plentiful with the bodies' natural healing factors; the cytokines, growth factors, and chemokines, which can jump start healing. PRP can also provide a fibrin scaffold for new tissue to grow onto, thus allowing new skin and tissue to form. If the PRP is injected directly into the wound base and along the edges in the wound, it can help to initiate healing by supporting endothelial and epithelial regeneration, and it can promote angiogenesis and collagen formation.2
I've read about this application for PRP but hadn't yet been able to try it, so when this patient presented himself with his chronic wound, I explained how PRP might help heal him. He was eager to try something new, so we set up an appointment so we could start treatment. Two weeks later, the patient returned to the office. The wound exam showed a partial-thickness wound just above the cleft of his buttocks roughly 1.5 × 0.3 × 0.2 cm.
The base was moist, pale pink with some scattered areas of yellow slough. The edges were intact and without epibole, and the periwound was clean and without erythema or edema. I drew the patient's blood and spun it in the centrifuge for about 10 minutes at 4,800 RPM to isolate the PRP.
During this time, I cleansed the wound with saline, applied a topical lidocaine to anesthetize the area, and gently debrided the slough from the base of the wound with a curette to prepare the wound for the injections.When the centrifuge had completed it's spin, the blood had separated into three distinct layers: the heavier red blood cells had sunk to the bottom of the vial with a sliver-like white layer of white blood cells above this and finally, a beautiful golden yellow layer of PRP floating on top.
I drew this into a syringe, and with a 25-gauge ½-inch long needle, carefully injected 0.2 mL of PRP around the circumference of the wound spaced every 0.2 cm. I also injected 0.2 mL of the PRP along the center of the wound base in the distal, medial, and proximal portion of the wound. I then flushed the entire wound with the remaining 1 mL PRP that was left in the syringe. After this treatment was completed, I applied a collagen dressing with a foam secondary dressing and counseled the patient to change this three times a week. The ideal course of treatment is twice a week, although given time constraints, we were able to set up a weekly schedule for continued injections.
Evidence Base and Reimbursement
In a 2018 observational study, 104 participants with chronic wounds were treated with 10 courses of twice weekly PRP injections. At the 10th visit, 85 (82%) of the patients were healed.3 PRP is an autologous product, and there are very few side effects, although some report localized pain or bleeding during the injection. Patients should not use anti-inflammatory medication before and roughly two to four weeks after injections because this can weaken the overall effect.
At this time, the greatest limitation for having PRP therapy is access. Finding a provider who will perform this service can be a challenge. Currently, most major insurers don't cover PRP for wound care. However, this may soon change. As of this writing, a major private insurer in my state covers PRP injections for orthopedic injuries.
In August 2012, Medicare started covering autologous PRP injections for chronic non-healing diabetic, pressure, and/or venous wounds only if the patient is enrolled in a clinical research study to assess for the effect of PRP with chronic wounds.4 The cost of PRP compared with major surgery or other invasive treatment is something that may start swaying more insurers to pay for it. At this time, PRP injections are primarily done in clinics that are cash based, and each treatment may range from $500 to $2,000 per visit or block of treatments. It may be tough for a patient to pay for an out-of-pocket procedure that, like much of medicine, has no guarantee, but for those patients who have tried everything else, PRP may be an alternative that could be considered.
Conclusion
Using one's own blood to heal an otherwise unhealable wound may seem like science fiction, but for my patient, this science fiction has become fact. As Mr. Spock famously said, "Change is the essential process of all existence." With the advent of new healing technology, it is up to us to create that path for change.
References
1. Quoted from Captain Picard in Star Trek, The Next Generation, Season 1, Episode 16, "When the Bough Breaks." Episode first aired February 13, 1988.
2. Chicharro-Alcántara D, Rubio-Zaragoza M, Sopena-Juncosa J, et al . Platelet-rich plasma: new insights for cutaneous wound healing management. J Funct Biomater. 2018; 9(1):10. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5872096/. Accessed February 11, 2020.
3. Prabhu R, Vijayakumar C, Sweta T, et al. Efficacy of homologous, platelet-rich plasma dressing in chronic non-healing ulcers: an observational study. Cureus. 2018;10(2):e2145. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5880593/. Accessed February 11, 2020.
4. Centers for Medicare & Medicaid Services. Autologous platelet-rich plasma. https://www.cms.gov/Medicare/Coverage/Coverage-with-Evidence-Developmen…. Accessed February 11, 2020.
About the Author
Becky received her BSN from the University of Vermont where, along with a love of nursing, she picked up a love of hiking and cross-country skiing. She moved to Massachusetts and started to work as a med-surg nurse at a busy Boston hospital. There, she found that she loved mentoring new nurses and returned to school to earn her MSN as an acute care clinical nurse specialist from the University of Massachusetts, Boston. She followed her love of teaching into the acute, sub-acute and university settings, but she found that she missed working directly with patients. She returned to school and earned her Post-Master's Family Nurse Practitioner Certification from Rivier University. It was shortly after this that Becky discovered her love for wound care. She worked part time in wound care and part time in family care while she earned her WCC certification. After several years, Becky decided to take her practice to the next level by opening her own LLC and is currently seeing patients for wound care and regenerative medicine. Becky's philosophy of “Never stop learning” has guided her in her practice and life. Her very supportive husband and daughter are her key inspirations to keep growing and trying new things. In her spare time, Becky loves traveling with her family, going on long walks with her dog, Echo, and reading historical and science fiction.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.