Scar Management
Scar formation is part of the last phase of wound healing, the maturation or remodeling phase. This phase can last from 21 days to two years, and it occurs only in full-thickness wounds. Cellular activities include collagen remodeling, capillary regression, and increasing tensile strength. Scar formation involves collagen cross-linking and replacement of the disorganized type III collagen by organized type I collagen. Other clinical observations include continued contraction thinning, and paling of the scar. It results in the restoration of dermal composition and an increase in the tensile strength of the wound over time to a maximum of 80% of the original tensile strength, 50% of which is restored by six weeks.1
Wound care has a direct impact on how your skin heals. With adequate wound care, it is possible to minimize scarring and in some cases even prevent a scar entirely, though prevention of scarring is not possible in full-thickness wounds.2
Types of Scars
Active scars may be red, firm, thick, or raised and can feel sensitive or even limit motion and function.3 However, the eventual appearance of the scar is dependent on multiple factors, including the cause of the wound, the wound size and depth, the part of the body that was wounded, and the wound care received. An overview of the primary types of scars includes the following2:
- Cicatrix: Appearance is flat or slightly raised with a pink or reddish color, although it may also be paler or darker than surrounding skin. It may feel itchy or painful. Proper wound care increases the chances that the scar will become flat rather than raised. Cicatrix is normal scarring.
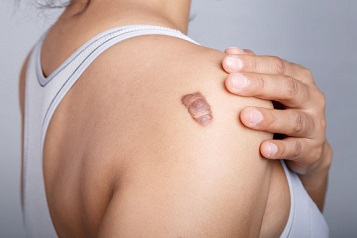
- Hypertrophic: Appearance is raised and firm, and it may feel painful or restrict movement. These scars most frequently form from wounds sustained on the chest, upper back, or shoulder, although they can appear anywhere on the body.
- Keloid: These scars are raised and grow to be larger than the wound that caused the scar. They can appear up to a year after an injury was sustained and can be itchy or painful.
- Contracture: Scars that form when the scar tissue is tighter and thicker than the surrounding skin. They can restrict movement, particularly if the scar is near a major joint, such as a knee.
Risk Factors
Factors that can have an impact on scar formation include the following2,4,5:
- Genetic variations that may be associated with scar formation
- Age
- Bacterial colonization
- Tension on the wound (scars often develop on body areas with high skin tension)
- Systemic inflammation, which can increase the risk of developing hypertrophic scars or keloids
- Hypertension, which is associated with increased keloid severity
- The presence of skin diseases, such as epidermolysis bullosa, which makes skin extremely fragile and results in blistering that forms scars upon healing, or hidradenitis suppurativa, which causes deep wounds in the skin
The extent to which scarring occurs can largely, although not entirely, be controlled by treatment.
Interventions and Treatment
Treatment of scars primarily depends on the type of scar or wound, but it can include one or more of the following options2:
• Pressure therapy: This therapy involves applying pressure with a pressure garment over dressings to a wound while it is healing to reduce a scar or prevent a keloid from forming or returning. Therapy the use of pressure garments can be continued use when dressings are no longer needed.
• Moisturizers: When applied at least twice daily, moisturizers can improve flexibility and help strengthen the area.
• Silicone gel, sheet, or ointment: Silicone gel, sheets or ointments are applied after a wound closes and can be used for several months to reduce the scar’s size, hardness, redness, itching, or stiffness. They can also prevent a scar from becoming raised.
• Polyurethane dressing: These dressings are moist and flexible and can be worn to reduce scarring or reduce the color, hardness, and size of a raised scar.
• Lasers or other light treatment: These treatments are becoming increasingly common because they can prevent raised scars and keloids, reduce the appearance of a scar, decrease scarring after surgery, lessen the color, and reduce the pain, hardness, itch, and swelling of a scar.
• Corticosteroid, 5-fluorouracil, or bleomycin injections: These injections are administered directly into the scar to reduce the size of it and ease itchiness and pain, although they generally require multiple treatments.
• Cryosurgery: This treatment freezes the scar to destroy scar tissue, which reduces the size, pain, itchiness, hardness, and discoloration of the scar.
• Scar surgery: Scars can be removed surgically to reduce the size of a keloid or increase mobility if the scar is limiting it.
• Radiation: Radiation therapy can reduce raised scars and ease some of the itchiness and discomfort.
• Other treatments: Other over-the-counter treatments include onion extract, vitamin A, and vitamin E, although research on their efficacy is limited.
References
1. Commander SJ, Chamata E, Cox J, Dickey RM, Lee EI. Update on postsurgical scar management. Semin Plast Surg. 2016;30(3):122-128.
2. American Academy of Dermatology Association. Scars: overview. 2018. https://www.aad.org/public/diseases/bumps-and-growths/scars. Accessed May 31, 2019.
3. American Society for Surgery of the Hand. Scar management. 2016. http://www.assh.org/handcare/procedures-and-treatment/scar-management. Accessed May 31, 2019.
4. Thompson CM, Hocking AM, Honari S, Muffley LA, Ga M, Gibran NS. Genetic risk factors for hypertrophic scar development. J Burn Care Res. 2014;34(5):477-482.
5. Schmieder SJ, Ferrer-Bruker SJ. Hypertrophic Scarring. Treasure Island, FL: StatPearls Publishing; 2019.






