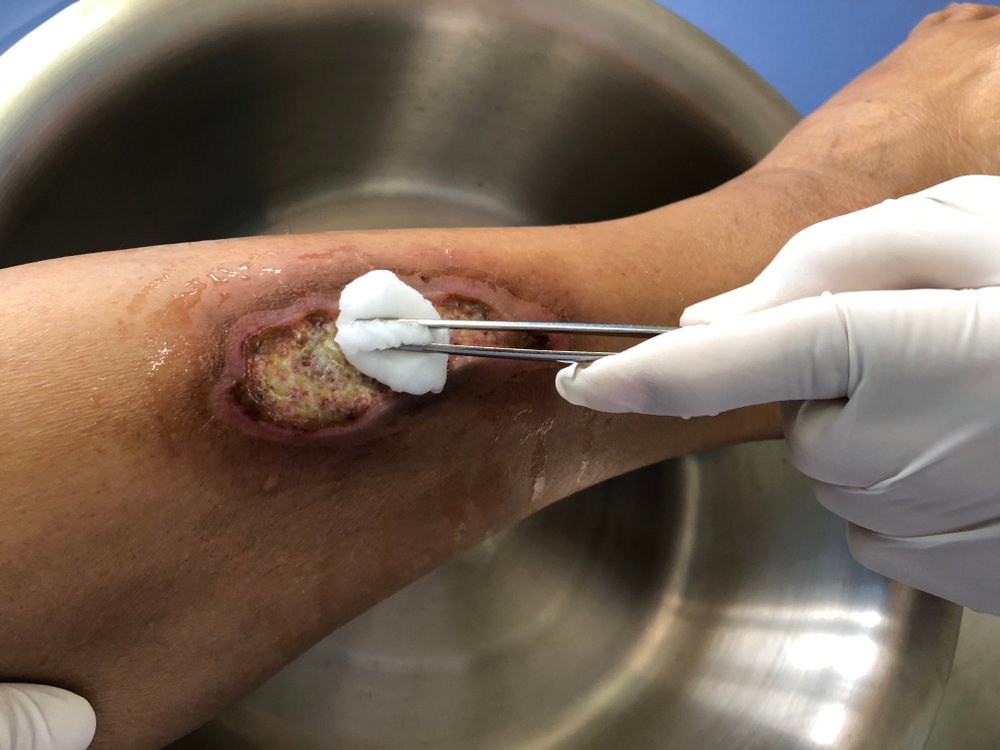
Tunneling Wound Assessment and Treatment
November 15, 2017
By the WoundSource Editors
Perhaps the most difficult type of wound for health care professionals to treat is a tunneling wound. Tunneling wounds are named for the channels which extend from the wound, into or through subcutaneous tissue or muscle. These tunnels sometimes take twists or turns that can make wound care complicated. Tunneling is often the result of infection, previous abscess formation, sedentary lifestyle, previous surgery at the site, trauma to the wound or surrounding tissue, or the impact of pressure and shear forces upon many tissue layers causing a “sinkhole-like” defect on the skin. Tunneling wounds need careful wound assessment and management.
Causes of Tunneling Wounds
Generally, the cause of the tunneling needs to be determined in order to treat the wound. Therefore, the first job of the health care professional is to assess the reason for the tunneling. There are many different reasons for tunneling wounds:
- Infection that has caused the destruction of tissue.
- Shear and pressure on a wound which concentrates on the tissue layers and causes separation and tunneling.
- Stalled wound healing in which an extended inflammatory phase creates tunneling.
- A wound dressing which dehydrated the wound.
- Too much or too little packing of a wound.
- Prolonged use of antibiotics can cause secondary infections which are resistant.
- Corticosteroids can slow down the formation of collagen.
- NSAIDs used for pain or reducing swelling may also suppresses protein synthesis and wound contraction.
- Diabetes can impair blood flow which delays wound healing and increases chances of infection.
Assessment and Management of Tunneling Wounds
Frequently, tunneling wounds have gone through many layers of tissues, creating curved or S-shaped wounds which are difficult to treat. The first step in assessment is to determine through examination of the wound and patient or caregiver interview the progression of the wound and possible causes of the tunneling. Next, the wound should be probed with a soft, non-fibrous explorer such as a soft polyethylene catheter to discover depth, number, and direction of tunnel tracts. It can be helpful to draw this on the skin with a permanent marker in order to help track healing progress. If necessary, sinography, CT scan or MRI can be used to make a complete assessment. Documentation of the track of tunnel measurements should be done using the face of a clock for position and in centimeters.
Treating a tunneling wound requires careful adherence to wound care techniques. Because often a tunneling wound has become chronic and worsened, it is especially important to monitor the healing carefully and be prepared to make changes if there does not seem to be significant progress. Management techniques include:
- Eliminating or reducing any of the identified causes of the tunneling wound.
- Thoroughly cleansing the wound in order to reduce the microbial load.
- After cleansing, the tunneling wound should be packed to avoid creating pressure on the sides of the tunnel where healthy tissue is growing.
- Packing should be careful to be adequate to prevent the wound becoming concave, but not so much to create pressure that forces it beyond the original tunneling wound edges.
- Using alginates, iodine-based dressings, hydrogels, medicated ropes, or collagen dressings to help stimulate granulation tissue formation, if traditional techniques do not produce a satisfactory progress in healing.
- Instructing patients and caregivers on ways to keep pressure and weight off of the tunneling wound site as much as possible.
- Monitoring a tunneling wound site at least weekly to monitor progress and so dressing selection can change if there is no progress in healing.
Goals in the Treatment of Tunneling Wounds
The goal in treating a tunneling wound site is to eliminate the causes, stimulate the growth of granulation tissue and ensure that wound edges don't close up prematurely, forming another abscess. Unfortunately, many of these types of wounds do not respond to mainstream wound care treatments and clinicians may need to create unique treatments for a tunneling wound. If necessary, wounds may require:
- Draining of the cavity to promote granulation.
- Surgical opening and debridement of the tunnels to properly clean and treat them.
- Applying negative pressure therapy.
Unfortunately, tunneling wounds which progress to deeper levels of skin and muscle are not just painful and uncomfortable, they can also increase patient morbidity and even mortality. Therefore, healthcare providers need to be prepared to make careful assessment and management of a tunneling wound a priority and to be proactive in changing to more aggressive treatment options to promote full healing.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.