Recognizing and Treating Wounds Caused by Pyoderma Gangrenosum
December 11, 2012
By Aletha Tippett MD
If you care for wounds and have never encountered pyoderma gangrenosum, count yourself lucky. Drawing from my years of experience and the nearly 20,000 wounds I’ve cared for, pyoderma gangrenosum is the most difficult and most challenging. Fortunately it is rare. It can occur anywhere on the body, but most commonly is seen on the legs. It usually starts as a fairly innocuous injury, such as a nick while shaving the leg, or a chip thrown from weed whacking. Antibiotics are used, which are not effective. The wound continues to worsen and grow in size, and now is referred to a wound center or wound specialist.
By this time, it is a wound covered with slough and necrosis and the first impulse of a wound care provider is to debride the wound, and maybe get a biopsy. I would caution you to do neither, because of a problem known as pathergy that is hallmark of pyoderma gangrenosum. With pathergy, any physical action taken on the wound makes it worse.
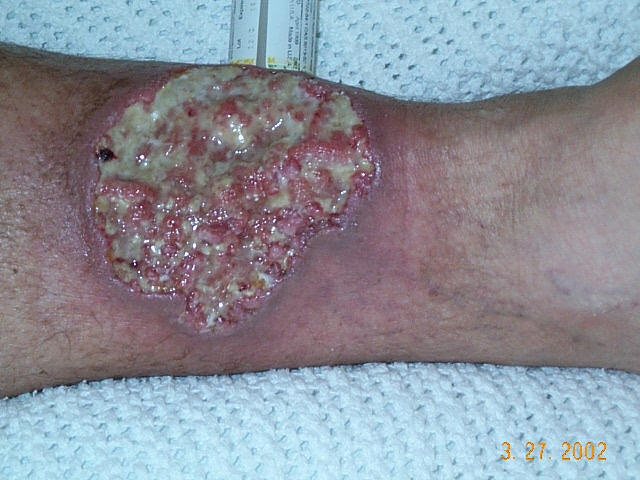
How to recognize pyoderma gangrenosum? First, always think - an enlarging painful wound with violaceous borders are the key characteristics. It is extremely painful. Regardless of what is done it gets larger. And, its borders are violet or blue in color. Look for underlying conditions in your patient, too. Pyoderma gangrenosum is an autoimmune disorder and will be found in people over the age of 40 and often in people with other immune problems, such as ulcerative colitis, rheumatoid arthritis, multiple myeloma, polycythemia vera. About half the time no underlying pathology is evident.
What to do if faced with pyoderma gangrenosum? In our clinic we always start the patient on prednisone. We use topical pain relieving wound dressings. If tolerated, we use multi-layer compression wraps. If the wound is still progressing, we add cyclosporine treatment. We sometimes use green clay on the dressing. We always do wound cultures, checking for bacterial and mycobacterial agents, and treat for any infection. And we always treat for pain with appropriate pain medications.
Success with this wound is not guaranteed. Despite every effort, sometimes the wound continues to worsen and there is nothing that can be done. In one case we had, ultimately the patient’s leg was amputated. Most times, however, the above treatment plan is successful, and we have had many more pyoderma gangrenosum patients who healed their wounds. This is, however, a condition to always be taken seriously. In conclusion, it is important to be able to recognize pyoderma gangrenosum so as to be able to treat it appropriately and with the sensitivity it requires.
About The Author
Aletha Tippett MD is a family medicine and wound care expert, founder and president of the Hope of Healing Foundation®, family physician, and international speaker on wound care.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.






