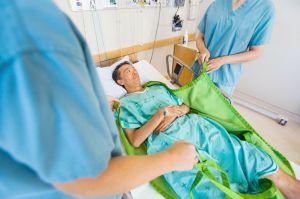
Tools to Maximize Turning and Repositioning Programs for Pressure Injury Prevention
May 26, 2016
I am very passionate about wound care, but pressure injury (pressure ulcer) prevention and awareness is at the top of my list for many reasons. My mother passed away in my arms at the young age of 47 due to complications of diabetes, amputation, and three pressure injuries. My mother's hospital-acquired pressure injuries were avoidable.
With all of the focus on pressure injury legalities, many of us are thinking of new ways to enhance prevention and awareness. I cannot even begin to count how many long-term care facilities and hospitals I have been to for staff education. I pay close attention and observe what types of prevention programs are being implemented. There are countless charts, tools, software, and devices from east to west coast. I am always fascinated when I see some of the clever ways facilities are maximizing pressure injury prevention programs.
The two most common drawbacks are usually a gap in ongoing education, along with sustained turnover in staff. These are only a few of the variables that may make or break a strong pressure injury prevention program. I often think to myself, "Why not use a carbon copy prevention program across the country?" Yes, we follow the same guidelines, but I do not see what I call "bulletproof" prevention and wound management programs. I personally think this approach would blow continuity of care out of the water. No matter where you work, you will know the ropes.
Preventing Pressure Injury Through a Consistent Program
Of course in today's health care, simply turning and repositioning a patient or resident at designated 2 hour intervals may help prevent pressure injuries, but it will not necessarily measure up for MDS coding, RUG scores, and payment purposes in long-term care, swing bed facilities, and hospitals. Also, during Federal and State surveys, pressure injury programs are investigated for ALL pressure injuries. With surveyors obtaining certification in wound care, we must enhance pressure injury prevention programs.
A turning and repositioning program must be consistent. The program must be documented, monitored, and evaluated, showing positioning and realigning of the body, and based on an assessment of the patient's needs. The program should also be tailored to the patient's time in or out of bed. Pay close attention to what your patient is doing all day long. Are they in the bed, sitting in a chair, or in a wheelchair? Pressure is pressure. That is the best perspective to have.
Pressure Injury Prevention Turning and Repositioning Tools
Cuing Innovations – The following tools provide the body location to offload and positioning every 2 hours:
- Turning and repositioning clock with an alarm to cue
- Clock charts at the nursing station that are signed off by Unit Manager
- Music/bells over the loudspeaker to cue every 2 hours
- Turning and repositioning labels placed on the ends of the patient's bed as a reminder
- Tracking, logging, and charting tools (these are signed off by the nursing assistant and nurse)
Wireless Sensor Monitoring System – A sensor is placed on the patient's chest. The sensor monitors and tracks the patient's activity. There is a generated report available for survey, as well.
Turning and Repositioning (TAPS) – This is the most common pressure injury prevention protocols. The problem is unless it is closely monitored, the program is not as successful. Utilizing extra resources and tools as mentioned will help implementation be more consistent.
Tissue Tolerance Test Tool - The State Operations Manual Appendix PP - Guidance to Surveyors for Long Term Care Facilities defines tissue tolerance as "the ability of the skin and its supporting structures to endure the effects of pressure, without adverse effects."
There is normally a three phase process to this test. Phase 1 - After the 1-hour interval, staff repositions the resident off the area exposed to pressure and observes/documents any areas of redness. Recheck the area after 30-45 minutes. If there is persistent red skin, stop the test. Consider the area to be a Stage I, notify the physician and obtain applicable treatment orders. The resident will require repositioning at an interval shorter than one hour. If there is no persistent redness, continue to Phase II.
Turning and Reposition Positioners – There are a variety of devices, pads, and slings that make turning easier and positioning more secure, while helping to reduce pressure injuries.
Pressure injury prevention is paramount. We can utilize the tools mentioned above, but unless we educate, mentor, empower, and monitor, it will not be successful. Protocols should be followed consistently to provide a strong structured prevention program. Use helpful resources provided by the National Pressure Ulcer Advisory Panel (NPUAP) to maximize implementation as well. The NPUAP provides complimentary webinars, illustrations, posters, white papers, policy, and standards. Click here for clinical guidelines and quick reference publications from the NPUAP.
References
The Journal of Post-Acute and Long Term Care Medicine
http://www.jamda.com/article/S1525-8610(10)00501-3/abstract
CMS MDS 3.0 RAI Manual
https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Ins…
The National Pressure Ulcer Advisory Panel - Support Surface Standards Initiative (S3I)
http://www.npuap.org/wp-content/uploads/2012/03/NPUAP_S3I_TD.pdf
The National Pressure Ulcer Advisory Panel - Pressure Injury Prevention Points
http://www.npuap.org/wp-content/uploads/2016/04/Pressure-Injury-Prevent…
About the Author
Cheryl Carver is an independent wound educator and consultant. Carver's experience includes over a decade of hospital wound care and hyperbaric medicine. Carver single-handedly developed a comprehensive educational training manual for onboarding physicians and is the star of disease-specific educational video sessions accessible to employee providers and colleagues. Carver educates onboarding providers, in addition to bedside nurses in the numerous nursing homes across the country. Carver serves as a wound care certification committee member for the National Alliance of Wound Care and Ostomy, and is a board member of the Undersea Hyperbaric Medical Society Mid-West Chapter.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.