Venous Leg Ulcers: Selecting a Treatment
August 31, 2021
Introduction
Hard-to-heal venous leg ulcers (VLUs) comprise the most common type of leg ulcer and impose a major economic burden on the health care system. These wounds can be difficult to heal, and they often experience recurrence within three months of closure, thus further complicating treatment. When managing VLUs, it is important to select strategies that are evidence based and cost-effective. Early diagnosis and implementation of interventions can encourage best outcomes.
Pathophysiology and Factors Complicating Healing
VLUs are caused by improper function of the veins. Veins in the legs carry blood back to the heart. They have one-way valves that make sure that the blood flows up the leg. When these valves are damaged, the blood can flow in the wrong direction, resulting in high pressure in the veins (called venous hypertension), which causes damage to the veins and results in ulcerations in the lower legs.1 Other medical conditions that can cause blood to pool in the veins of the legs and lead to VLUs are varicose veins, deep vein thrombosis, and heart failure.
VLUs can be hard-to-heal wounds because of an imbalanced microenvironment where a multitude of factors causes healing to stall. Various factors that impede healing include inflammation, biofilm, excess matric metalloproteinases, extracellular membrane degradation, fibrosis, compromised growth factor signaling, and lack of response in keratinocytes and fibroblasts.2,3 When one or more of these factors begins to repeat itself, it encourages tissue destruction.
Treatment Goals
Treatment of VLUs may require utilizing multiple methods to achieve closure. The goals of treatment should be keeping the VLU free from infection, managing edema, and maintaining an optimal moist wound healing environment. Other goals include treating and alleviating the underlying condition.1 When selecting treatment methods for patients with VLUs, it is important to take a holistic approach to support better outcomes. Not all patients are the same, and treatment plans should be tailored accordingly.
Standard of Care
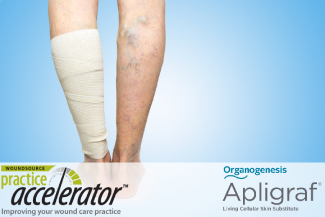
Standard of care in VLUs includes compression therapy, which remains the cornerstone of management. Choosing the right compression product is essential in achieving best outcomes. Graduated compression bandaging helps redirect blood flow back to the heart, reduce edema, and decrease levels of destructive proteases and inflammatory cytokines that may contribute to wound chronicity.4 Patients who have poor calf pump function will benefit most from this therapy. Make sure to provide education to patients: compression therapy will need to be continued even after wound closure to prevent recurrence.5 Treating VLUs should always be based on best evidence to heal chronic wounds faster and more cost-effectively. Start with a comprehensive medical history, a detailed physical examination, and management of the underlying pathophysiology. Options for treatment include compression, local wound care, surgical intervention, medical treatment, and advanced therapies and technologies.
Advanced Therapies
Advanced therapies are especially useful in the management of VLUs that do not adequately heal with standard treatment modalities. These types of therapies continue to grow in the advanced wound care market and include collagen dressings, biological dressings, biological skin equivalents, keratinocytes, platelet-derived growth factors, platelet-rich plasma, and silver products.6 Antimicrobial and antiseptic dressing variations have been shown to improve wound healing in VLUs. These dressings are available in various technologies, formats, sizes, and absorbencies. They can include antimicrobials or antiseptics such as cadexomer iodine, silver, medical-grade honey, and peroxide-based preparations, among others.7 Negative pressure wound therapy (NPWT) has been reported to accelerate wound healing successfully in patients diagnosed with VLUs. It also has had a better effect on healing various types of leg ulcers compared with moist wound treatment alone.8 NPWT has been used as a bridge to surgery and as an end therapy, by reducing exudates and increasing granulation tissue formation.9 Cellular and/or tissue-based products (CTPs) are being used as adjunct therapy to standard care in the treatment and management of VLUs. CTPs facilitate accelerated healing in chronic VLUs while lowering treatment costs and reducing risks and complications in this population. CTPs are biologically active and designed to replace (temporarily or permanently) the form and function of the skin.5
Conclusion
All patients are different and will require different approaches. Early identification in high-risk patients, diagnosis, intervention, and prevention of recurrence are all vital components in VLU management. Utilizing various dressings that support wound healing can be effective to treat and manage VLUs, but it is also important to remember to re-evaluate VLUs regularly and makes changes to treatments as needed and to use a more aggressive approach such as advanced therapies.
References
- Seth AK, Geringer MR, Hong SJ, Leung KP, Mustoe TA, Galiano RD. In vivo modeling of biofilm-infected wounds: a review J Surg Res. 2012;178(1):330-338.
- Cleveland Clinic. Leg and foot ulcers. Cleveland Clinic. Accessed May 24, 2021. http://my.clevelandclinic.org/heart/disorders/vascular/legfootulcer.aspx
- Frykberg RG, Banks J. Challenges in the treatment of chronic wounds. Adv Wound Care. 2015;4(9):560-582.
- Beidler SK DC, Berndt DF, Keagy BA, Rich PB, Marston WA. Inflammatory cytokine levels in chronic venous insufficiency ulcer tissue before and after compression therapy. J Vasc Surg. 2009;49(4):1013-1020.
- Cole W. Management of venous leg ulcers and venous insufficiency. Podiatry Management. August 2018. Accessed May 24, 2021. https://www.podiatrym.com/cme/CME818.pdf
- Greer N, Foman N, Dorrian J, et al. Advanced Wound Care Therapies for Non-Healing Diabetic, Venous, and Arterial Ulcers: A Systematic Review. Washington, DC: Department of Veterans Affairs; 2012. Accessed August 9, 2021. https://www.ncbi.nlm.nih.gov/books/NBK132235/
- O’Meara S, Al-Kurdi D, Ologun Y, et al. Antibiotics and antiseptics for venous leg ulcers. Cochrane Database Syst Rev. 2014;(1):CD003557.
- Yao M, Fabbi M, Hayashi H, et al. A retrospective cohort study evaluating efficacy in high-risk patients with chronic lower extremity ulcers treated with negative pressure wound therapy. Int Wound J. 2014; 11:483-488.
- Argenta LC, Morykwas MJ. Vacuum-assisted closure: a new method for wound control and treatment: clinical experience. Ann Plast Surg. 1997; 38:563-577.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.