Skin Grafts
A skin graft is a section of epidermis and dermis harvested from one part of the body and reaffixed to a site where the skin has been removed or damaged. Unlike flaps, which are connected to a blood supply, skin grafts lack a blood supply of their own and must rely on the recipient wound bed for nutrients.
When contemplating a skin graft in wound reconstruction, the donor site must also be considered. It is often more painful than the recipient wound due to exposed dermal nerve endings. There are two different types of skin grafts: split-thickness and full-thickness.
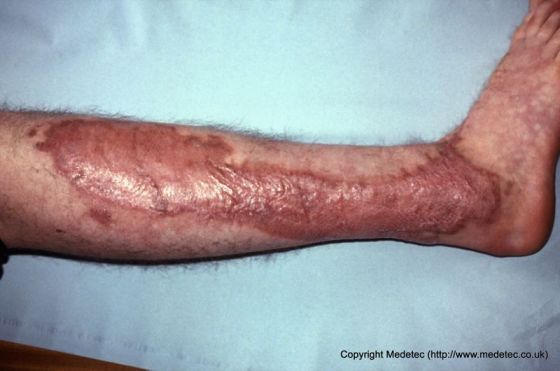
Split-Thickness Skin Grafts
Split-thickness skin grafts (STSG) are thin, including epidermis and a small portion of dermis. leaving behind enough of the dermis for the donor site to heal by reepithelialization. As a result, these grafts can survive on less than ideal recipient beds (with less vascularity). However, the thinner the graft, the more likely it is to contract as it heals. STSGs can then be meshed, allowing for smaller sections of tissue to be used to effectively cover larger areas. The combination of meshed appearance, varying pigmentation, and thinness makes STSGs more pragmatic than cosmetic. The thicker the graft, the more the characteristics of the donor skin will be evident as the wound heals.
Once the wound bed has been properly prepared, the graft is secured in place and an appropriate dressing is applied. Care is taken to provide even pressure across the surface of the graft site. The pressure reduces the risk of heamatoma or seroma formation that can lead to graft compromise. In addition, the dressing should reduce the risk of shear forces to the graft site. For hard-to-dress areas or wounds with irregular contours, tie-over bolster dressings or negative pressure wound therapy may be indicated to protect the graft and provide consistent pressure. Typically, the first dressing is left in place for three to seven days, barring any complications. Prior to removal, the dressing is moistened with sterile saline to minimize any separation of the graft from the wound bed. The dressing should then be reapplied twice a week while monitoring the graft for infection, drainage, pain, and overall success of the procedure.
Full-Thickness Skin Grafts
Full-thickness skin grafts (FTSG) involve the epidermis and the entire dermis as well, allowing for most of the characteristics of the grafted skin to be preserved in the process. FTSGs are limited to smaller wounds and require well-vascularized wound beds in order to support the grafted skin. Since the entire dermal layer is removed and will not support regeneration, the resulting skin graft donor site will be sutured closed. FTSGs maintain more of the normal characteristics of the skin (notably texture, color and thickness), and contract less during healing. As a result, FTSGs are aesthetically pleasing and a good choice for the face or other highly-visible areas of the body.
If the graft covers the entire wound bed and is well adhered, it may not require a dressing except to protect it from mechanical damage.
References
Beldon P. What you need to know about skin grafts and donor site wounds. Wound Essentials. 2007;2:149-155. https://www.woundsinternational.com/resources/details/what-you-need-to-k.... Accessed August 9, 2019.
Havill S. Skin grafting. DermNet NZ. https://www.dermnetnz.org/topics/skin-grafting/. Accessed August 9, 2019.
Hubbard M. Pearls for Practice: Managing Skin Grafts and Donor Sites. Ostomy Wound Management. http://www.o-wm.com/content/managing-skin-grafts-and-donor-sites. Published February 1, 2010. Accessed August 9, 2019.
Khosh MM, Shohet MR. Full-Thickness Skin Grafts. Medscape Reference. http://emedicine.medscape.com/article/876379-overview#a1. Updated April 8, 2016. Accessed August 9, 2019.
Wax MK. Split-Thickness Skin Grafts. Medscape Reference. http://emedicine.medscape.com/article/876290-overview#a1. Updated May 22, 2017. AAccessed August 9, 2019.
Image copyright Medetec (www.medetec.co.uk). Used with permission.






