Accountability and Responsibility: The Cornerstones of Pressure Ulcer Prevention
July 22, 2015
Perspective of Nursing Care from Past to Future by Matron Marley
Most of the residents here are elderly, though some of the more acute rehab patients are quite a bit younger than me. We actually have five women over a 100 out of 116 people, quite impressive with the eldest being 105 years old. As for me, I am a retired British matron just doing a little volunteer work near where my granddaughter works.
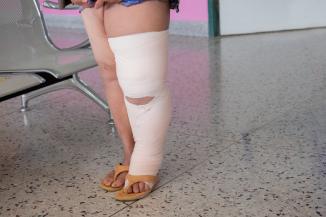
We had a man admitted last week. The reason for his admission is that he needed rehabilitation after his extensive injuries following an MVA. He had a pressure ulcer, which was noticed on admission at our facility. He had been in the critical care unit and was only on the main floor for three days before transferring to us.
The critical care unit had put on an adhesive foam dressing to protect the patient's sacral area and nursed him on a pressure reduction alternating, low air loss surface. Sadly the floor to which he was sent did not look under the dressing and at handover to our team said his skin was in excellent condition and he was on a regular mattress. They did not mention the prophylactic dressing and as it was removed, the evolving deep tissue injury was revealed by the skin peeling away. Non-viable skin peeled and over the next few days the subcutaneous layer turned to slough while we observed, dumbstruck, wondering at exactly what point the injury occurred and how bad would it become as we have seen more than a few.
Introducing Pressure Ulcer Risk Assessment Scales
As a matron all those years ago, before the introduction of intensive care units and saving the lives of unhelmeted motorcyclists, we battled pressure ulcers. It was more to do with not appreciating all the risk factors, and how to reposition safely rather than a lack of care. We used side lying and alcohol rubs, cushioning, padding and donuts. Waterlow, Norton and Braden changed all that in the 1980s and we began to look at the risk of our patients and become proactive with their care. With the growth of saving lives in ICU came more pressure ulcers and better surfaces with offloading devices that worked.
I looked into the eyes of the young nurse that removed this patient’s adhesive foam dressing and saw the tears as she verbalized to me her horror. Horror at the peeling purple beneath. Horror that the Braden they had given him of 19 was in fact 12. Horror that they did not think his lack of movement and sensation below the waist warranted a reduction on both the mobility and activity scale. His nutrition was less than adequate (due to nausea with movement). The condom catheter would drop the moisture score even more as it was described as difficult to keep on. He was young with supple healthy skin masking the distress incurred at his change from ICU status. Her horror deepened as his wife recounted his bolt upright position in bed and the absence of any kind of turning routine.
How can this be, with all we have and all we know, how can this happen? Who is accountable, where is the responsibility? How do educators get across to health care staff the importance of ensuring the people who we care for deserve our very best? We should be caring for them as we would our child, sister, mother or spouse. Such disasters need not happen.
As a matron, I remember being so proud of a sister (charge nurse) on one of the orthopedic floors. It is the first place that I know of to track pressure ulcer data. She had a little red book where she recorded every pressure ulcer that occurred on her ward. It was due to the data she presented to the surgeons on heel ulcers that stopped them tightly securing the heel of patients undergoing pin and plate for fractured neck of femur.
First, she presented the data at the nurse manager meeting. The theater manager was appalled. (My memory is that for one set of 10 hip surgeries, seven developed heel ulcers, all on the affected side). We made a "field trip" to the operating room and the manager showed us the heel cup and how the ankle was strapped to help stabilize the leg during surgery. It took months to get through to the surgeons that the practice had to change. It was also some of her data that assisted in the procurement of specialty mattresses. It was not the nurses that needed to see the data, they saw the pressure ulcers they caused. It was the administrators and directors who needed the lesson. Patients stayed for sufficient time for the staff to see the results of any poor care they delivered. We did not always have the equipment needed to prevent the problems we saw.
I remember one patient with a badly fractured pelvis. There were no specialty mattresses so we laid her on pillows. We put a sheet sideways under her chest and another under her hip area. Four staff members would support her holding the sheet and two more would change and turn the pillows, every 2 hours by day and 3 hours by night. We used a fracture pan for her stool and a female urinal at every second position change. It was a sleek routine but not without its hiccoughs.
Who Is Held Accountable When a Pressure Ulcer Develops?
Today, patients pass through our hands as if lubed to perfection, sliding through a system bent on efficiency, not necessarily care. There is no moment to pause for thought, as the risk assessment score fits the criteria required for the protocol driven care to be delivered. Boxes to check replace the thoughtful process of narrative and these boxes give us data. So much data that I am sure it must be useful, it has to be, doesn't it? Do the nurses see the patient, do they take responsibility for those in their charge and are they held accountable?
If by the next shift there is a different body in the bed, how can we care? There has to be a way because the man I described earlier deserves the best care available. Will the nurses, over the six shifts that passed while his deep tissue injury developed beyond repair, learn of his plight? Will they ever know how big his pressure ulcer became or how much it extended his rehab? How long did it prevented him from going home or whether it meant he lost his job? How did his pressure injury affect his partner and his relationship?
We struggle so hard to prevent pressure ulcers and then the patients under our care have to endure, laying on an ambulance stretcher when transferred for tests, scans, dialysis and outpatient appointments. They lay, reclined and restrained by dialysis paraphernalia, slide while sitting, uncared for by anyone beyond the walls of our facility. I watch as ambulance folk, slide and bundle, wondering why they can’t use the special board and sheet. There was a suggestion that when we transfer patients, we call forward to ensure they get regular pressure relief. One nurse I know recently called to an emergency room to ask if they would please continue our repositioning schedule. She was so worried about calling but believe me when I tell you the future is bright. She was met with an excellent response from the ER nurse.
The time is now. For patients with pressure ulcers on admission, the unit that discharged them should be informed. For transferring patients, a transferring repositioning schedule should be adopted by their receiving unit until full assessment and care plan is established.
The future will be bright, our data does not lie. It gives us ammunition to make staff and the powers that be sit up and realize, "this could be my mother, daughter, husband or son, or me."
About The Author
Based on her extensive nursing experience Margaret Heale, Wound, Ostomy and Continence Nurse, takes us into the blog journal of a fictitious matron, "Perspective of Nursing Care from Past to Future by Matron Marley."
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.