Beauty and Biofilm: The Intersection of Science, Art, and Wound Care
January 19, 2017
You are looking at an amazing image of a dime-sized biofilm of Pseudomonas aeruginosa, grown and photographed by Scott Chimileski – a biologist, photographer, and writer at the Kolter Lab at Harvard Medical School.
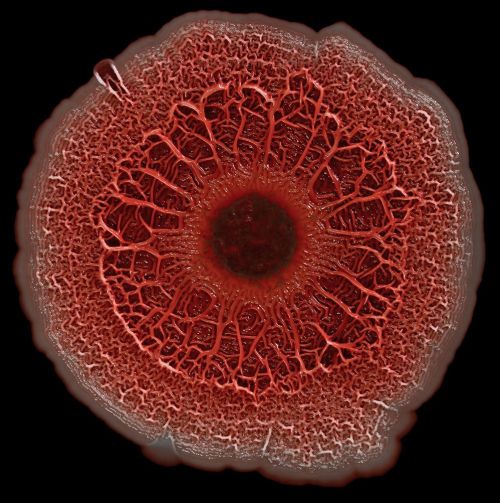
He captured the eerie, otherworldly look of this dangerous organism. The bacterial colony appears red because of the stain that Scott used to demonstrate its chemical structure. This photo is one of the winners of the Federation of American Societies for Experimental Biology (FASEB) 2016 BioArt contest. Part of Scott’s research is on the fundamental processes of biofilm formation, one of the major frontiers in wound healing science today.
The Impact of Pseudomonas Aeruginosa Biofilms on Wound Healing
Pseudomonas is a common gram-negative pathogen that causes pneumonia, urinary tract infections, bacteremia, sepsis, endocarditis, and soft tissue infections. This organism may account for 10% of all hospital acquired infections, and multi-drug resistant strains are on the rise. Those of us who have encountered Pseudomonas in wounds often remember its characteristic sweet odor. Pseudomonas commonly attacks skin rendered vulnerable from edema, vascular disease, and diabetes, and is often hard to eradicate particularly in immunocompromised patients. Here is one of my clinical photos of Pseudomonas infection of leg ulcers:
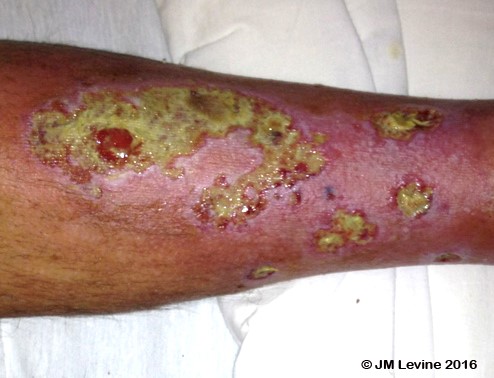
Pseudomonas can occur in burns, post-surgical wounds, pressure injuries, and diabetic foot wounds. The microorganism secretes a variety of materials to form an extracellular matrix that holds the biofilm together, and protects the bacteria from antibiotics and the immune system - making it challenging to eradicate. I’ve always been interested in the intersection of art and science, and Scott Chimileski is right on point. You can see more amazing photographs of microorganisms on his website, http://www.scottchimileskiphotography.com/. Click here to see the results of the 2016 FASEB BioArt Winners.
About the Author
Dr. Jeffrey Levine is a board certified internist and geriatrician with over thirty years of experience in wound care in hospitals, nursing homes, and home care environments. He is Associate Professor of Geriatrics and Palliative Care at the Icahn School of Medicine at Mount Sinai, and has a hospital based wound care practice at the Center for Advanced Wound Care at Mount Sinai Beth Israel Medical Center in Manhattan. He received his fellowship training in geriatrics at the Mount Sinai Medical Center where he began his interest in chronic wounds. He is an elected board member of the National Pressure Ulcer Advisory Panel (NPUAP). Dr. Levine’s interest in pressure ulcers began in the 1980s during his geriatric training when he noticed that many of his nursing home patients had pressure ulcers but there was little reliable information on treatment methods. This motivated him to study not just prevention and treatment of chronic wounds, but to delve into the rich history of wound care over the centuries. He has since published a number of articles on historical topics ranging from wound care in ancient Egypt through the 20th Century.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










