Chronic Venous Insufficiency: Overview and Advanced Treatment Options
July 22, 2014
by Bruce E. Ruben MD
Chronic venous insufficiency (CVI) refers to a long-term condition where the veins inside the legs have lost their ability to move blood back up to the heart from the legs. This occurs because the vein walls have weakened to the point where the venous pumps are no longer sufficient enough to send blood back up, against gravity, to the heart. CVI also affects the tiny valves inside the leg veins. When these valves do not close sufficiently, blood seeps back down past the valves and pools in the lower legs.
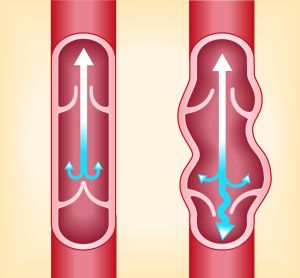
Risk Factors for Chronic Venous Insufficiency
Chronic venous insufficiency crosses all genders, races, and socioeconomic strata. We know what venous insufficiency is but we don’t completely know why some people get it while others don’t. That’s because it’s the quality of the leg veins that creates the condition and not necessarily any activity or lack of activity on the part of the patient.
Given that there is a genetic component to a patient’s propensity to acquire the condition, however, there are various risk factors for CVI. First, we see more cases of CVI in people over the age of 50, people with a sedentary lifestyle, and people who sit or stand for long periods of time.
There is also an increased risk for the disease in patients who have had a previous injury to the legs or who have a family history of venous insufficiency. Additionally, there is a higher incidence of CVI in patients who smoke or are obese.
Symptoms of Chronic Venous Insufficiency
The onset of venous insufficiency is marked by symptoms that may or may not be painful including swelling of the legs, the appearance of varicose veins, skin color changes around the ankles, and flaking, itching or tingling on the legs or feet.
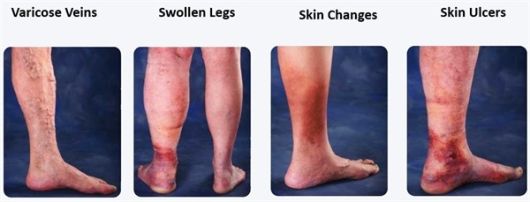
More painful presentation of CVI includes a dull aching, heaviness, burning, throbbing or cramping in the legs. That pain will generally get worse when the patient is standing.
Advanced symptoms include thickening and hardening of the skin on the legs and ankles, and ulcers on the legs and ankles.
Assessment of Venous Insufficiency
Treatment for venous insufficiency begins with a thorough patient history to identify risk factors for the condition and to acknowledge any previous studies performed. For example, a physician may ask if the patient has had any compression therapies in the past.
After the history, the doctor examines the patient for clinical signs of venous insufficiency, which may include changes in skin color, edema and the presence of a venous ulcer usually located on the inside (medial) ankle or calf.
Another clinical observation made is to determine if pain is relieved when the leg is raised or lowered. If pain is relieved when the leg is raised that is consistent with venous insufficiency since raising the leg helps move the blood back to the heart. Conversely, if pain is relieved when the leg is lowered, this may indicate arterial insufficiency since gravity is helping the blood move downward.
After these factors are assessed, the physician may order a venous ultrasound to establish the quality of blood flow in the region. This test will also identify any blood clots and misshapen veins. This is important to establish immediately as blood clots can dislodge at any time and travel upward – creating a life-threatening pulmonary embolism in the lungs or a miocardial infarction in the heart.
Available Treatments for Venous Insufficiency
The first line of treatment for venous insufficiency involves making lifestyle adjustments. First, patients should avoid long periods of standing or sitting. If sitting for a long period is inevitable, such as driving or flying a long trip, then it’s important to stretch and flex the legs, feet and ankles several times every half hour. Also, when standing for long periods of time, take frequent breaks sitting with the legs elevated.
Another lifestyle change is adding in regular exercise to improve cardiovascular health. Walking is especially beneficial. It’s also important to lose excess weight.
Compression Stockings and Wraps
Firm fitting compression stockings and the newer Velcro wraps support the upward flow of blood through the veins. It’s important to care for these products by keeping them clean and dry so they do not irritate the skin.
Venopneumatic Compression Pumps
Venopneumatic compression pumps automatically inflate and deflate sequentially to force fluids back into the veins, and to move those fluids up from the lower extremities back to the heart.
Compression pumps are easy to use and effective for supporting fluid transport. Patients place their legs in special sleeves that are attached to a small, portable pump. The sleeves have built-in compartments that fill with air and then deflate sequentially to push fluids up the legs.
Minimally Invasive Venous Ablation
Venous ablation is the surgical procedure of shutting down one poorly performing vein in the leg so the body will return venous blood more efficiently through its healthier leg veins.
At Encompass HealthCare and Wound Medicine, we perform two types of venous ablation: Radiofrequency Ablation and ClariVein®, a non-thermal vein ablation system. Both methods represent significant advances in medicine, as they are far less invasive with fewer complications and dramatically improved healing rates when compared to outdated procedures like vein stripping or surgical vein removal.
Radiofrequency Ablation
With radiofrequency ablation, a thin, flexible tube called a catheter is inserted into a diseased vein through a tiny incision in the leg. Radiofrequency energy is then delivered inside the vein to provide an even and uniform heat to contract the collagen in the vein walls, causing them to collapse and seal. Once a leg vein is closed, blood flow is redirected to healthy veins.
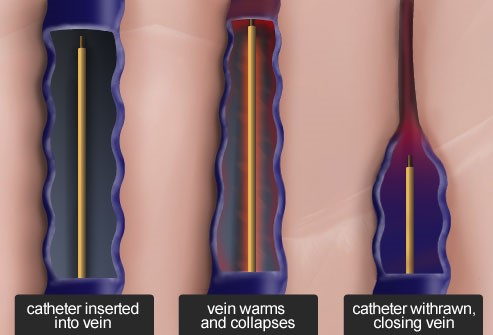
Radiofrequency ablation provides a fast, comfortable recovery so the patient can return to everyday activities, most often within 24 hours of treatment.
ClariVein®
ClariVein is the latest endovascular technique for treating venous reflux disease. It involves inserting a rotating tube (catheter) into the vein, together with a drug, to close and seal it. Nothing but a local anesthetic is needed, so the treatment requires no hospital stay.
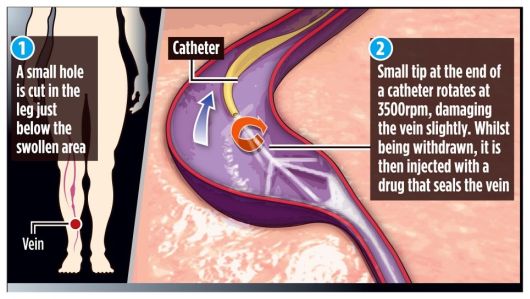
Compared to other similar techniques like laser ablation, ClariVein provides greatly reduced pain levels and virtually no discomfort or bruising during and post procedure. This is because the technique disrupts the lining of the vein, the endothelium, which then allows the highly effective use of sclerosants to close the vein.
This revolutionary device and technique have significant benefits for clinicians, patients, and health care providers:
- ClariVein is safe and effective and requires minimal local anesthesia.
- It eliminates the risk of nerve or skin damage or parathesia (the feeling of prickling, tingling or burning) from thermal energy.
- Excellent results are achieved by combining painless mechanical agitation within the vein along with proven sclerosants that shrink and collapse the vein.
- ClariVein is ideally suited to treat the great or small saphenous veins.
- There is virtually no bruising or pain and the patient can go back to work and resume regular activities almost immediately.
There are a number of methods for treating venous insufficiency. A thorough patient assessment is important in determining the best course of treatment for individuals with this long-term condition.
Select images courtesy of Clarivein (Vascular Insights, LLC). Used with permission.
About the Author
Dr. Bruce Ruben is the Founder and Medical Director of Encompass HealthCare, located in West Bloomfield, Michigan. Encompass Healthcare is an outpatient facility featuring advanced wound care, IV antibiotic therapies, hyperbaric oxygen treatment, nutritional assessment, and other treatment modalities. Dr. Ruben is board certified in Internal Medicine, Infectious Disease, and in Undersea and Hyperbaric Medicine. He is a member of the Medical and Scientific Advisory Committee and National Spinal Cord Injury Association (NSCIA) board.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.






