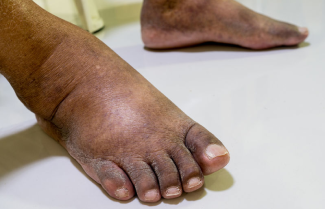
Help Make Lymphedema Treatment More Accessible For Your Patients
June 2, 2016
By Janet Wolfson, PT, CLWT, CWS, CLT-LANA
Long ago, in a Physical Therapy Department far away, I met my first lymphedema patient, but did not know that was the cause of her recurring wounds. Into the next decade, I treated more patients with chronic swelling in their legs and we put something called Unna boots on them. But the boots did not work for everybody. By the end of the decade, there were layered compression wraps and I had started to see courses for therapists in manual lymphatic drainage. Hmmm, curious…
Patient Access to Lymphedema Treatment
In the next decade, I was fortunate to meet a Certified Lymphedema Therapist (CLT) and the lights came on. This was why some wounds recurred, why Unna boots did not always work and why compression garments are medically necessary for lymphedema patients. I was fortunate to have my employer send me to the essential, yet expensive course that would allow me to provide better care to my lymphedema patients. I had become certified in wound care and so knew the physiology of wound healing, and now I knew how to treat the cause of these wounds. As a newly minted CLT, I provided manual lymphatic drainage (a massage technique to move the fluid congesting the patients' body to functioning lymph nodes), instruction in decongestive exercises and meticulous skin care to prevent infections. I also wrapped their extremities and sometimes trunk in bandages to direct fluid out of their swollen body parts and prevent its return. With their participation in this program, they were ready for graduation into a compression garment. This is where the light would dim for some. The garments were unbelievably expensive for some and unaffordable. They were sadly not covered by Medicare and therefore not by most insurance companies.
Another light was shining where I then lived in Georgia in the form of the Lighthouse Lymphedema Network (LLN). Birthed in 1993 in the kitchen of its founder, Joan White, LLN not only educated the community and medical professionals about lymphedema, but also fundraised to provide needy lymphedema patients with monies for compression garments. When Medicare could not help prevent hospitalizations due to infection (cellulitis or open wounds) and chronic swelling, this amazing group has provided hundreds of garments to Georgia residents. (Learn more at www.lighthouselymphedema.org.)
The Lymphedema Treatment Act
So now I must be really old, as we are in yet another decade… But the lack of coverage for lymphedema compression garments is really old. So along came another astounding woman with a son who needed lymphedema care (yes it can affect newborns and people of any age). Heather Ferguson, of North Carolina, convinced her state legislature to mandate insurance coverage for lymphedema treatments including compression supplies. In 2009, she secured the support of her congressman in the first ever federal Lymphedema Treatment Act. By 2010, she had founded the Lymphedema Advocacy Group to raise awareness and support needed to pass the bill through Congress. In 2015, HR 1608, the Lymphedema Treatment Act was introduced and to date has 227 cosponsors. The Senate version, S.2373 was introduced in late 2015 and has 18 cosponsors. These members of Congress have recognized the medically necessary service HR 1608 and S.2373 can provide and the monies saved by avoiding infection and hospitalization.
So today, to make my long story shorter: if you have ever treated a patient with lymphedema or even repeatedly treated them, please visit following link for more information and consider joining the American Medical Association as well as many other healthcare organizations in supporting the Lymphedema Treatment Act. Go to www.LymphedemaTreatmentAct.org and follow the "how you can help" menu. Help shine a laser beam to focus Congress on this Bill before the end of 2016.
About the Author
Janet Wolfson is a wound care and lymphedema educator with ILWTI, and Lymphedema and Wound Care Coordinator at Health South of Ocala with over 30 years of field experience.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.