How Scar Tissue Causes Pain and Tips for Management
April 28, 2021
I have again been inspired by my son to blog on a not so talked about topic, scar tissue pain. I have had patients through the years report scar pain, and I admit I did not know too much about it. I decided to dive into this topic a bit more when my son started experiencing frequent pain in his chest. He had a traumatic injury to the chest 14 months ago that healed in six weeks. There is a large amount of thickened traumatic scar tissue because of the depth of the injury.
The pain started approximately two months after the wound healed, and he described it as a sharp stabbing pain that would take his breath away. We started researching different ways to manage the scar tissue care and help with the pain. What has worked best for him is using an unscented advanced repair moisturizing lotion containing petrolatum and dimethicone. He massages it into the scar tissue every day after showering. After five weeks of this scar tissue regimen, he has finally reached a substantial amount of pain relief. He continues this scar tissue care as part of his daily routine.
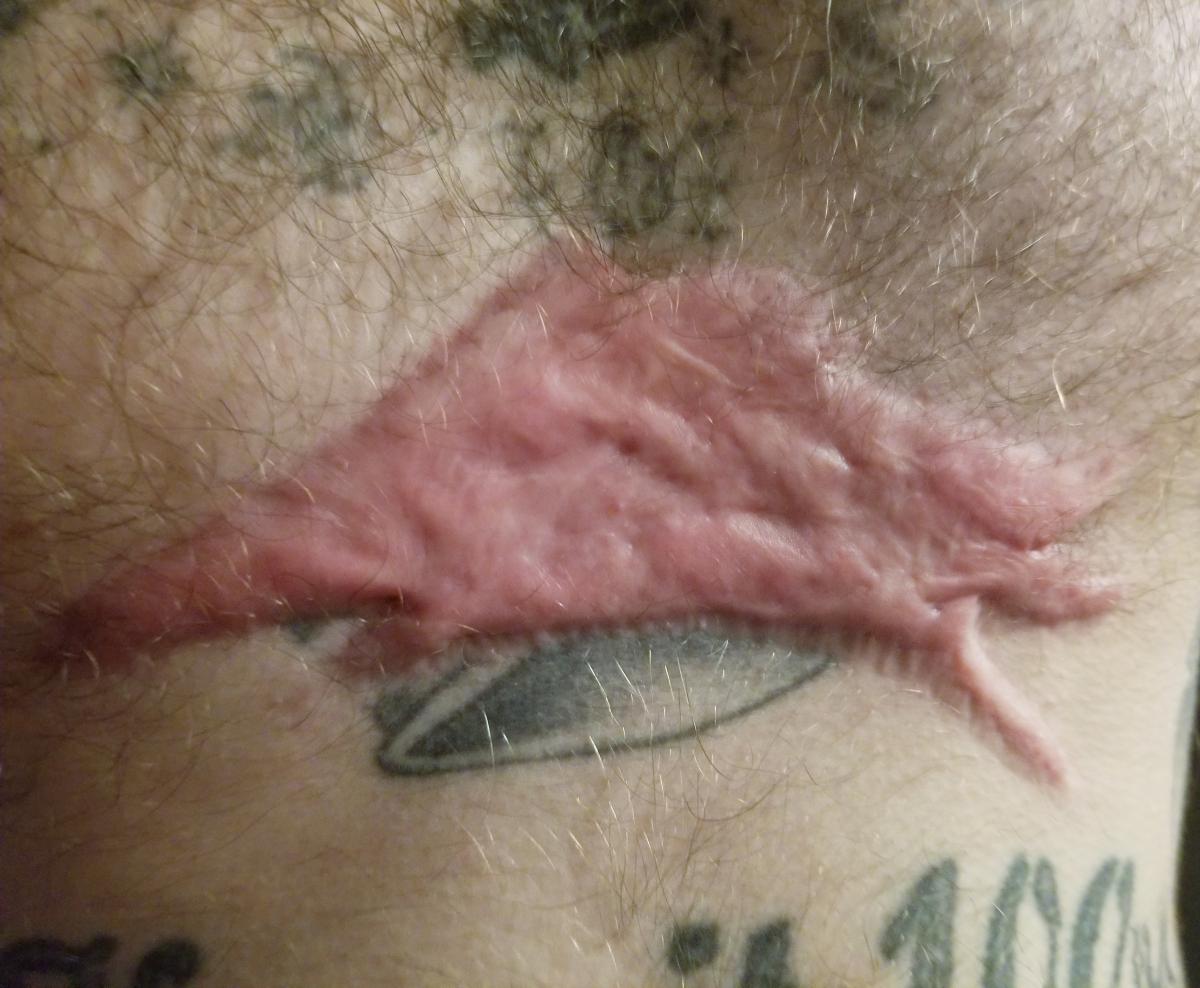 Provided with patient's consent; © Cheryl Carver
Provided with patient's consent; © Cheryl CarverScar Tissue
Wounds heal by primary or secondary intention. Healing by primary intention occurs when wounds are approximated with sutures, staples, or other tools that will allow the wound to heal. Healing by secondary intention occurs when wounds are left to heal on their own by filling in with granulation, contraction, and epithelialize from the bottom up. As expected, more superficial wounds are confined to the epidermal layer and ultimately heal faster. As for deeper, full-thickness wounds, the injury is extensive and requires more time to heal, and this results in a more noticeable, thicker scar. Scar tissue is not the same as skin tissue. There is less elasticity, and this may lead to tightness, limited movement, and sometimes pain. In scar tissue formation, collagen proteins grow in one direction rather than in a multidirectional pattern as in healthy skin. Scar tissue can take 12 to 18 months to mature but will only ever reach 80% of tensile strength of unwounded skin.1
Scar Tissue Pain
Scar tissue is not always painful. If there is pain, it may be caused by nerve damage from the injury. There are also instances where scars do not become painful until later. This is because nerve endings regenerate over time. Pain can also result from fibroblasts causing prolonged inflammation, with symptoms of itching, swelling, tenderness, and sensitivity. This condition is called fibrosis.
Scar Types
Depending on the type of injury, such as burns or stab wounds, the wound may develop one of several different types of scars.
- Traumatic scars: When a significant injury to the skin heals, it leaves a traumatic scar. Traumatic scars frequently cause abnormal sensations, pain, and itching. Traumatic scars may affect patients physically, psychologically, and socially. Patients can develop depression and anxiety over scar disfigurement, especially patients with burn wounds.2
- Atrophic scars: These scars are sunken or “ride low” and are thinner than the surrounding skin. Examples are chickenpox and acne scars.
- Hypertrophic scars: These scars are raised or “ride high” above the skin and are thicker, remaining within the original wound margin at injury.
- Contractures (scar tightening): Contractures are located over joints. When the scarring involves the muscles and nerves over a joint, contractures will make it difficult to move and will cause pain.
- Keloid scars: These scars “ride high” above the skin surface and extend beyond the original wound margin at injury. Their color is normally a red plaque that forms on tissues after an injury. The location of keloids often appears on the earlobe, breastbone, shoulder, back, and face.
- Surgical scars: Large or deep surgical incisions can take six to eight weeks to heal. Healing depends on the patient’s overall general health and the type of surgery.
- Stretch marks: In skin that has quickly expanded or shrunk, the connective tissues underneath may become damaged, causing stretch marks. These are commonly known to occur during pregnancy or after gaining or losing a substantial amount of weight.
Scar Tissue Care and Treatment Options
There are some scars that are better off left undisturbed. For scars that do require attention when certain patterns emerge, there are at-home treatments to try. If there is no success with at-home treatments, then other medical procedures may help lessen scar appearance and/or pain. When deciding which treatment is best with a provider, it will depend on the scar’s location, symptoms, and length of duration (age).3

Physiological and Social Scars
Scars can be emotionally devastating and can lessen self-esteem. Scars do not all have the same cause. Changes in appearance can negatively affect body image and confidence. Patients with scars do not have as many treatment options available to address their psychological burden. Providers tend to lack training in identifying and managing these psychosocial issues.
References
1. Martin P, Nunan R. Cellular and molecular mechanisms of repair in acute and chronic wound healing. Br J Dermatol. 2015;173(2):370-378.
2. Jagdeo J, Shumaker PR. Traumatic Scarring. JAMA Dermatol. 2017;153(3):364. doi:10.1001/jamadermatol.2016.5232.
3. American Academy of Dermatology. Scars: overview. https://www.aad.org/public/kids/skin/scars. Accessed April 13, 2021.
About the Author
Cheryl Carver is an independent wound educator and consultant. Carver's experience includes over a decade of hospital wound care and hyperbaric medicine. Carver single-handedly developed a comprehensive educational training manual for onboarding physicians and is the star of disease-specific educational video sessions accessible to employee providers and colleagues. Carver educates onboarding providers, in addition to bedside nurses in the numerous nursing homes across the country. Carver serves as a wound care certification committee member for the National Alliance of Wound Care and Ostomy, and is a board member of the Undersea Hyperbaric Medical Society Mid-West Chapter.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.