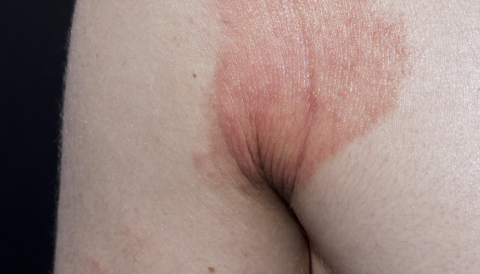
Microclimates in Skin Folds: The Growing Impact of Moisture and Friction
May 8, 2026
Why This Matters
- Skin fold microclimates significantly increase the risk of MASD, fungal infection, and skin breakdown, particularly in patients with obesity, immobility, and contractures.
- Intertriginous conditions are common but underrecognized, with prevalence estimates reaching up to 30% in high-risk populations and contributing to increased healthcare utilization.
- Growing patient complexity and emerging technologies underscore the need for focused education, making this topic highly relevant for clinicians seeking to improve outcomes in vulnerable populations.
Moisture-associated skin damage (MASD) remains a persistent and costly challenge across care settings, but its impact is amplified in patients with deep skin folds, bariatric anatomy, limited mobility, or contractures. These patients are uniquely vulnerable to localized “microclimates”—enclosed environments characterized by elevated moisture, heat, pH shifts, and friction—which accelerate skin barrier breakdown and increase susceptibility to infection.
As the prevalence of obesity and chronic disease continues to rise in the United States and globally, the number of patients at risk for intertriginous complications is expanding significantly. According to the Centers for Disease Control and Prevention (CDC), approximately 41.9% of U.S. adults are classified as obese, with severe obesity affecting nearly 9.2% of the population.1 This demographic shift has direct implications for wound care, as increased adiposity is strongly associated with deeper skin folds, higher perspiration rates, and greater mechanical stress on the skin.
Despite this growing risk profile, pannus and skin fold management often remain underemphasized in wound care education and clinical workflows—creating a critical gap in prevention-focused care.
Epidemiology and Burden of Intertriginous Skin Damage
Intertriginous dermatitis, including intertrigo and fungal infections, is one of the most common dermatologic conditions affecting patients with obesity and limited mobility. Studies suggest that intertrigo may affect up to 20%–30% of individuals with obesity, with higher rates observed in institutionalized or immobile populations.2
Moisture accumulation in skin folds promotes maceration, which weakens the stratum corneum and increases permeability to irritants and pathogens. This environment is particularly conducive to Candida species, which are frequently implicated in secondary infections. Candida colonization rates in intertriginous areas have been reported to exceed 60% in high-risk populations.3
In addition to fungal involvement, bacterial overgrowth and polymicrobial colonization further complicate the clinical picture. The presence of excess moisture and friction also increases the risk of skin tears, erosions, and progression to partial-thickness wounds—particularly in patients with fragile skin or comorbidities such as diabetes and vascular disease.
From a health system perspective, MASD and intertriginous complications contribute to increased length of stay, higher treatment costs, and greater nursing burden. A systematic review found that MASD prevalence in acute care settings ranges from 5% to 27%, with higher rates in critical care and long-term care populations.4 These figures likely underestimate the true burden in skin folds, where assessment challenges may lead to underreporting.
The Role of Microclimates in Skin Breakdown
Microclimates within skin folds represent a convergence of several risk factors that compromise skin integrity. Elevated humidity and temperature alter the mechanical properties of the skin, reducing tensile strength and increasing susceptibility to frictional injury.5
Friction and shear forces are particularly problematic in areas where skin surfaces are in constant contact, such as beneath the pannus, in the groin, or under the breasts. These forces disrupt the epidermal barrier, creating pathways for moisture penetration and microbial invasion. Over time, repeated exposure to these conditions can result in chronic inflammation and tissue damage.
Emerging research highlights the importance of microclimate control as a key factor in preventing skin injury, particularly in high-risk populations.6 However, awareness of this concept remains variable among clinicians, underscoring the need for targeted education.
Friction, Pannus, and Mechanical Stress: A Compounding Risk
The presence of a pannus—a large overhanging abdominal fold—introduces additional biomechanical challenges. The weight and movement of the pannus increase pressure and shear forces on underlying skin, exacerbating risk of friction-related injury.
From an epidemiologic standpoint, pannus-related complications are closely linked to obesity severity. Individuals with class III obesity (BMI ≥40 kg/m2) are disproportionately affected, with higher rates of skin infections, hospitalizations, and surgical complications.7
These issues extend beyond physical health. Skin fold conditions are associated with pain, odor, and psychosocial distress, all of which can negatively impact quality of life and patient engagement in care.
Why This Topic Deserves Attention
The increasing prevalence of obesity, aging populations, and chronic disease is reshaping the landscape of wound care. As a result, clinicians are encountering more patients with complex anatomical and mobility-related risk factors that contribute to microclimate-driven skin damage.
Despite the significant burden associated with intertriginous conditions, pannus management and microclimate control remain underrepresented in many educational curricula. Addressing this gap is essential for improving patient outcomes, reducing complications, and supporting more proactive approaches to skin integrity.
Ultimately, advancing knowledge in this area is not only a matter of improving skin health—it is a critical component of comprehensive, patient-centered wound care.
References
- United Ostomy Associations of America. Ostomy statistics. Accessed May 6, 2026. https://www.ostomy.org/ostomy-statistics/
- Colwell JC, Pittman J, Raizman R, Salvadalena G. A randomized controlled trial determining variances in ostomy skin conditions and the economic impact (ADVOCATE trial). J Wound Ostomy Continence Nurs. 2021;48(1):50-57.
- Bray F, Laversanne M, Weiderpass E, Soerjomataram I. The global cancer burden 2020: GLOBOCAN estimates of incidence and mortality worldwide. CA Cancer J Clin. 2021;71(3):209-249.
- Salvadalena G. Incidence of complications of the stoma and peristomal skin among individuals with ostomies. J Wound Ostomy Continence Nurs. 2020;47(5):423-428.
- Nichols TR. Health utility, social functioning, and peristomal skin complications. J Wound Ostomy Continence Nurs. 2021;48(2):141-146.
- Pittman J, Colwell JC, Raizman R, et al. Characteristics of the patient with an ostomy associated with leakage. J Wound Ostomy Continence Nurs. 2021;48(1):43-49.
- Taneja C, Netsch D, Rolstad BS, Inglese G, Eaves D, Oster G. Clinical and economic burden of peristomal skin complications in patients with recent ostomies. J Wound Ostomy Continence Nurs. 2020;47(2):141-149.
- Claessens I, Probert R, Tielemans C, et al. The Ostomy Life Study: the everyday challenges faced by people living with a stoma. J Wound Ostomy Continence Nurs. 2021;48(2):163-170.
- Nichols TR, Inglese GW. The burden of peristomal skin complications on quality of life. J Wound Ostomy Continence Nurs. 2020;47(5):432-438.
- Colwell JC, Beitz J. Survey of WOC nurse clinicians on stoma and peristomal complications. J Wound Ostomy Continence Nurs. 2022;49(3):251-257.
- Wound, Ostomy and Continence Nurses Society. Management of the adult patient with a fecal or urinary ostomy: clinical guideline. WOCN Society; 2022.
- Gray M, Colwell JC, Doughty D, et al. Peristomal moisture-associated skin damage in adults with fecal ostomies: a comprehensive review and consensus. J Wound Ostomy Continence Nurs. 2021;48(2):101-107.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.