When Prevention Fails: Pressure Injury Management
October 31, 2020
When pressure injury prevention fails as a result of non-adherence, various comorbidities, or gaps in care, it makes a major impact on the nation’s economy and has estimated costs of more than $100 billion in the United States.1 There are differences in each health care setting when it comes to prevention programs, budgets, and availability of equipment, and policies and procedures may hinder implementation of a pressure injury prevention program. Penalties related to pressure injury prevention may be a consequence of failure to prevent these injuries. Thousands of lawsuits are filed annually, and most cases are settled in favor of the patient.2 Facilities should use the latest evidence-based guidance in leading their prevention team.
Failure of Pressure Injury Prevention Programs
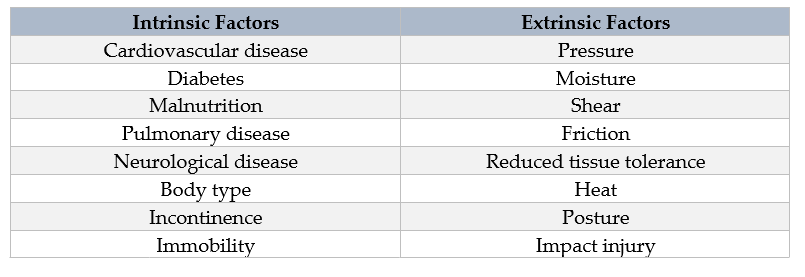
Various factors are associated with failure of preventative measures, including gaps in education, inadequate communication, low socioeconomic status, various dressing product categories, reimbursement guidelines, and mental or cognitive issues. There must be a commitment between the patient and provider to solve the problem and meet the needs of the patient. The provider should be able to provide expert care or refer the patient to a wound care specialist that will help support the best guided plan of care, and the patient should be willing to adhere to prescribed interventions or preventative measures in order to ensure best outcomes.3 Pressure injuries are caused by a complex interplay of various intrinsic and extrinsic factors. Advanced age, chronic conditions, and the use of certain medications are some of the risk factors affecting tissue health.4
Basic Management Strategies
Management of pressure injuries includes standard wound care techniques, as well as meticulous skin care and optimal nutrition. Patients should receive daily skin care checks to monitor for areas of potential breakdown, and a Registered Dietitian should be consulted to conduct a nutritional assessment as poor nutrition can be a major factor leading the pressure injury development.
Advanced Wound Care Modalities
Foam Dressings
In pressure injuries, pressure, friction, shear, and microclimate stresses damage the skin. Foam dressings have been recognized, clinically and statistically, to aid in pressure injury reduction by diminishing the effect of these pathogenic processes. Topical dressings with multiple layers and soft silicone are also shown to have an added benefit in prevention of pressure injury.5,6
How much do you know about pressure injury prevention? Take our 10-question quiz to find out! Click here.
Cellular and/or Tissue-Based Products
Cellular and/or tissue-based products (CTPs), also known as skin substitutes, and biological products were primarily developed to counteract problems encountered with allografts (skin from another human) and xenografts (skin from another species). Skin substitutes facilitate healing and regeneration in chronic wounds. Stage 3 and 4 pressure injuries can be complex, warranting additional advanced treatment modalities such as CTPs to support tissue growth and wound closure. When the product is applied over the entire wound surface area, CTPs provide extracellular matrices to encourage immune function and tissue regeneration.7,8-11
Collagen Dressings
Collagen dressings are primary dressings containing live tissue used in direct contact with the wound bed. Collagen is derived from various animal sources such as bovine, equine, porcine, ovine, and avian. These dressings can be used on acute or chronic wounds with minimal to heavy exudate, thus making them ideal for pressure injuries. Collagen is conformable to fit into difficult to reach wounds areas while managing exudate and providing an optimal moist environment to enhance healing. Collagen dressings are available in sheets, particles, amorphous gels, and pads. In wound healing, collagen attracts fibroblasts and encourages deposition of new collagen into the wound bed. Collagen dressing technology helps stimulate new tissue growth while encouraging autolytic debridement, angiogenesis, and re-epithelialization.7
Negative Pressure Wound Therapy
Negative pressure wound therapy (NPWT) is proving to be a promising option for patients with full-thickness pressure injuries. The wound must be adequately debrided before dressing application. NPWT is a vacuum-assisted machine with carefully controlled suction (negative pressure). NPWT has many effects, including reducing edema, increasing perfusion, stimulating granulation tissue formation, managing moist wound healing, and removing infectious material and exudates, thereby keeping wounds cleaner,12,13 NPWT dressings can also provide a barrier to adjacent fecal flow. Pressure injury guidelines for both prevention and management advise that NPWT is used for pressure injuries that have high exudate, to reduce the number of dressing changes.14
Conclusion
Continuity of care requires communication, education, understanding, and teamwork between the provider and patient. Utilizing intervention methods, advanced treatment modalities, and education in complex patients will help reduce pressure injury worsening and recurrence.

References
1. Noncompliance with Medication Regimens: An Economic Tragedy. Emerging Issues in Pharmaceutical Cost Containing. Washington, DC: National Pharmaceutical Council; 1992;1-16.
2. World Union of Wound Healing Societies consensus document. Role of dressings in pressure ulcer prevention. Wounds International. 2016. https://www.woundsinternational.com/download/resource/5930. Accessed October 23, 2020.
3. Gaude GS, Hattiholi J, Chaudhury A. Role of health education and self-action plan in improving the drug compliance in bronchial asthma. J Family Med Prim Care. 2014;(1):33-38.
4. Hommel A, Santy-Tomlinson J. pressure injury prevention and wound management. In: Hertz K, Santy-Tomlinson J, editors. Fragility Fracture Nursing: Holistic Care and Management of the Orthogeriatric Patient. Cham, Switzerland: Springer; 2018. doi: 10.1007/978-3-319-76681-2_7. https://www.ncbi.nlm.nih.gov/books/NBK543831/. Accessed October 22, 2020.
5. Agency for Health Care Policy and Research (AHCPR). Pressure Ulcers in Adults: Prediction and Prevention. Clinical practice guideline no. 3. AHCPR publication no. 92-0047. Rockville, MD: AHCPR; 1992.
6. Santamaria N, Gerdtz M, Sage S, et al. A randomised controlled trial of the effectiveness of soft silicone multi-layered foam dressings in the prevention of sacral and heel pressure ulcers in trauma and critically ill patients: the border trial. Int Wound J. 2015;12(3):302-308.
7. What you need to know about collagen wound dressings. (2017, April 07). Retrieved January 19, 2020, from https://woundcareadvisor.com/what-you-need-to-know-about-collagen-wound…
8. Devels H, Hamdi M, Abberton K, Morrison W. Dermal matrices and bioengineered skin substitutes: a critical review of current options. Plast Reconstr Surg Glob Open. 2015;3(1):e284. https://pubmed.ncbi.nlm.nih.gov/25674365/. Accessed October 223, 2020.
9. Ferreira et al., 2011;
10. Nicholas et al., 2016;
11. Vig et al., 2017
12. Dumville JC, Webster J, Evans D, Land L. Negative pressure wound therapy for treating pressure ulcers. Cochrane Database Syst Rev.2015(5):CD011334. doi: 10.1002/14651858.CD011334.pub2.
13. Niezgoda JA. Combining negative pressure wound therapy with other wound management modalities. Ostomy Wound Manage. 200551(2A Suppl):36S-38S.
14. National Institute for Health and Clinical Excellence. Pressure ulcers: prevention and management of pressure ulcers. Clinical guideline 179. 2014. https://www.nice.org.uk/guidance/CG179. Accessed October 22, 2020. .
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










