Why Not Use Maggots to Treat Wounds?
March 5, 2015
Recently I had a discussion with several other physicians and a topic that came up was why maggots were not more widely received. I was not aware that maggots were not widely received since I have used them regularly for 15 years. So, the question is, why not use maggots? In the wound care field, providers frequently come across infected wounds, wounds with necrotic tissue, wounds with wet gangrene, or wounds that are slow to granulate. All of these wounds could be helped with maggot therapy. There is no size limit or requirement for using maggots. You just need at least 10 maggots per square centimeter of wound. For small wounds I try to estimate the 10 per square centimeter and use at least that number of maggots. For large wounds, for example, the whole foot, I just use the entire vial of maggots.
How Medicinal Maggots are Supplied
Maggots come in a vial with 300 to 500 maggots in the vial, FDA approved by the way. The number is printed on the vial. They are in the vial with small strips of sterile gauze. My technique is to use what is called “free range” maggot therapy. Whatever number of maggots I need, I just use sterile gauze pads to collect and apply to the wound. I then cover the maggots with a moist gauze pad, then cover this with a piece of chiffon, then pull a nylon stocking over the foot (assuming we are doing this on a foot). The top of the nylon footie has already been cut off to remove the tight binding, then the top is taped securely in place around the limb. This is where maggots would try to get out if they were done before removed. Then gauze and gauze wrap are placed around the wound area. If the maggots are successful there will be dark drainage after about six hours. My instructions are to change this gauze wrap every 8 hours if there is dark drainage. After 48 hours the entire wrap and dressing is removed and placed in a biohazard bag. The foot is rinsed well. Sometimes if the maggots are in a crevice they can be removed with forceps, but that is not usually required.
The wound can then be dressed however desired and followed as usual. If needed, more rounds of maggot therapy can be done, usually about one every week. While the patient has the maggot dressing in place, there is no limit to their activity other than to not get the dressing wet. Some patients have even gone to work. If the wound is on an area other than foot, the process is the same, but instead of pulling the stocking up over the foot, a large piece of stocking is placed over the wound, and taped in place, then gauze padding placed over this. To me, this procedure is very simple and safe. The vial of maggots is kept in the refrigerator until used. Any leftover maggots are discarded (unfed maggots disintegrate). Maggots can be ordered Monday through Friday, so can be placed Tuesday through Saturday. They are removed two days later.
How Patients Perceive Maggot Therapy
Patients love the maggots and are eager to be involved in their use and care. No one has ever refused maggots, especially when they are portrayed as “our friends” who can help us with this problem. Many patients recall a friend or relative in the service who was saved by maggots, or they have seen a show about maggots and are excited to give it a chance. One patient released his maggots instead of destroying them in the biohazard bag. He said “why would I destroy what saved my leg and life?”
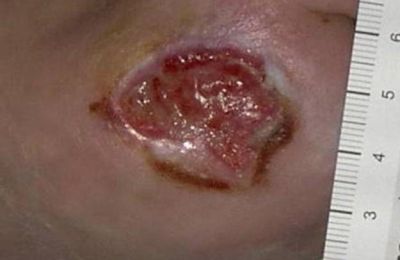
Maggots are available in the U.S. only from Monarch Labs. There are different suppliers in other countries. If one does not want to use free range maggots as I described here, there are dressings available from Monarch Labs, with instructions. There are also “biobags” available with the maggots entirely contained in a small bag. Personally, I have tried a biobag and did not find it as effective as free range maggots. The bottom line though is that there are a number of ways to utilize maggots, all providing the benefits of this therapy—elimination of infection, stimulation of collagen and granulation, reduction of odor, elimination of necrotic tissue and gangrene, often saving limb and life. So, when confronted with a problematic wound one should consider “why not use maggots?” To learn more about this company and product visit http://www.woundsource.com/company/monarch-labs-llc Photo credit: Aletha Tippett. Used with permission.
About The Author
Aletha Tippett, MD is a family medicine and wound care expert, founder and president of the Hope of Healing Foundation®, family physician, and international speaker on wound care.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.