Wound Bed Preparation and the Whole Team Approach
June 25, 2019
The prevalence of non-healing wounds is a challenge and concern for all levels of health care professionals. Clinical evidence has proven that using a multidisciplinary team approach to wound care is key in providing quality of care across the continuum. Clinicians should keep the mindset of always viewing the patient as a whole. A multidisciplinary team consists of members from many different disciplines using their areas of expertise to focus on the wound care patient. Bringing the knowledge and skills together of the wound team will provide guidance to better clinical, health, and financial outcomes.
Education of Team Members
Remember to educate other team members along the way. There may be a multidisciplinary team, but encompassing the rest of the “caregiver team” is just as important. These are the front-line workers who are providing one-on-one personal care to patients. Integrating interventions for persons with wounds should include thorough assessment, implementation of care, monitoring, and follow-up, thereby closing the gap in care. Professionals working together have individual goal sets but will communicate with the patient and team to collaborate treatment goals.1 Patients should have knowledge of their wound etiology and treatment care plan, but this is not always possible. Multidisciplinary team members can help bolster compliance by empowering and educating their patients. Patients who want to share in decision making tend to have better outcomes.2
Communication Gaps
Proper communication among members of the multidisciplinary team is critical. Mutual respect and consideration of each other’s roles on the team is also important. Regular meetings, email, phone, fax, pager, and face-to-face interactions are all ways to close the gap of poor communication. Communicating different treatment options, wound healing progress, plan of care, and a multitude of perspectives will all help move toward the ultimate goal of wound healing.1,2 The most common gaps in communication are as follows:3
- Nursing assistant or caregiver to nurse to physician
- Wound clinic to facility (long-term care, skilled nursing, assisted living, etc.)
- Nurse to physician and physician to nurse
- Physician to physician
- Patient to family and family to patient
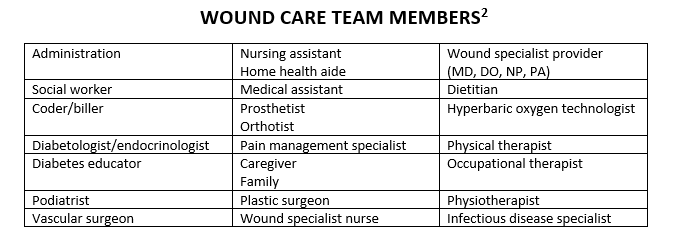
Development of a Successful Wound Care Team
To develop an effective and successful wound care team, there are many core key elements. You can develop a wound care team in every health care setting. The way you conduct team interactions may vary, but it all comes down to teamwork. Every team member is just as important as another. Weekly wound rounds or assessments provide consistency. Wound rounds should be done as a team or between the provider and clinical staff in other health care settings. The wound consultant or provider should work together with the wound nurse or charge nurse to discuss the patient’s history and activities of daily living (ADLs), wound etiology, treatments, and plan of care. Involve front-line workers such as nursing assistants and caregivers who are providing the one-on-one care.
They are with the patient on a daily basis and can answer many questions, such as what prevention measurements are in place, current appetite, pain complaints, offloading techniques, compliance, suggestions in care, and redistribution equipment, etc. This information can help assist in the appropriate treatment that is best for the patient. Administrative staff members assist with appointments, transportation, coding or billing, and payer verifications.
The dietitian evaluates patients’ nutritional status, determines any supplement needs, and orders blood work needed to monitor protein levels. Physical therapists (PTs), occupational therapists (OTs), and speech therapists (STs) provide therapy toward benefits that rehabilitation interventions can provide to help heal wounds. Providers of different specialties should discuss comorbidities, wound classification, treatments, follow-up appointments, and goals to work toward the best collaborative approach to wound management. Patients and family caregivers should always be provided with handouts, written orders, and education regarding wound etiology and wound management to minimize misunderstandings while providing patient satisfaction.1,2,3
Conclusion
Communication is the key factor to managing a strong wound care team. Wound care team players must be open to suggestions, participate in ongoing education, follow dressing formularies, and provide good documentation to avoid misunderstandings or discrepancies. Collaboration of health care professionals, along with good communication, can improve patient outcomes.
References
1. Moore Z, Butcher G, Corbett LQ, et al. Exploring the concept of a team approach to wound care: managing wounds as a team. J Wound Care. 2014;23 Suppl 5b:S1-S38.
2. Physiopedia. Multidisciplinary/interdisciplinary management of the amputee. https://www.physio-pedia.com/Multidisciplinary/interdisciplinary_manage…. Accessed June 13, 2019.
3. Cioroiu M, Levine JM. Improving communication in the wound clinic. Today’s Wound Clinic. 2013;7(3). https://www.todayswoundclinic.com/articles/improving-communication-woun…. Accessed June 13, 2019.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










