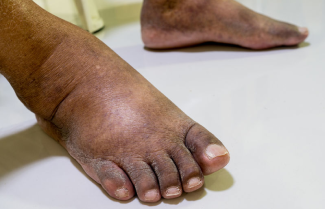
Wound Care Challenges: When The Lymphatic System Doesn't Work
October 17, 2017
If you had a chance to read last month's blog on lymphedema and the lymphatic system, you're probably still amazed that such a wonderful system that provides immunity and handles fluid in our bodies exists in such secrecy. This blog discusses what can go wrong with the lymphatic system. Because this network has many parts throughout the body, with cells that generated and living in different areas, whose complexity needs consideration with other disease processes or surgery, and must be constructed in 9 months of gestation... A lot could go wrong!
Development of the Lymphatic System
Due to difficulty defining lymphatic markers, difficulty visualizing vessels with traditional methods, and emphasis on the vascular system, research into the development of the lymphatics is still in its infancy–with many theories still to be proven. Without a doubt, it starts development in week 5, perhaps from the veins or the mesenchyme. Then, in weeks 6-9, sacs are formed in the neck, groin, posterior abdominal wall, and in the gut. Ducts grow and connect the different sacs while lymphatic vessels grow peripherally to the head, neck, arms, gut, and legs. The sacs become the lymph nodes, except for the upper portion of the gut sac: the cisterna chyli. Mesenchymal cells infiltrate the nodes and develop channels, capsule, and node framework. Lymphocytes appear just before birth in the nodes from the thymus. Lymph organs form from mesenchymal cells and clumping of lymph nodules.
So, from week 5 to the final week of gestation, the lymphatic system is developing. A spontaneous mutation at any point, injury to the fetus, a hereditary malformation, or a preterm delivery can all affect the lymphatic system of a child. This deficit can be apparent at birth, or latently appear at any time in their life, depending on where the deficit is.
I am sure you're questioning if there is any way to diagnose if there could be lymphatic abnormalities prior to conception or delivery. Modern molecular science has identified some genetic lymphatic markers, allowing for research into congenital lymphedema. Many families with hereditary lymphedema (that were eventually diagnosed after decades of passing it down) volunteered their time and genes to assist in the Lymphedema Family Study at the University of Pittsburgh, as well as other entities. Seven genes have been identified that, when mutated, will cause lymphedema due to either malformation or malfunction of the lymphatic system. Still other markers have identified women at increased risk of developing lymphedema post-mastectomy, and stem cell therapy has relieved symptoms in an affected patient. Growth factors that facilitate lymphatic growth have been identified, and subsequently used in successful treatment of mice and rabbits with lymphedema.
Causes of Lymphedema
There are other causes than genetic factors that can initiate the lymphedema cascade. Worldwide, the greatest cause of lymphedema is a parasitic infection called filariasis. The Wuchereria bancrofti larva are injected into human hosts by mosquitos, and develop into the adult worm in the lymphatic system, causing filariasis lymphedema. The cycle is perpetuated when the human host is bitten by mosquitos that then pick up larva. In the USA, the most common causes are trauma, burns, infections, tumors, surgery, and/or cancer treatments. These cases are most commonly diagnosed once the edema appears. Proactive practitioners and clinics will educate their client about the possible side effect of lymphedema.
More next month on how necessary medical care and disease processes can affect the lymphatic system, and if there is anything to be done prophylactically...
Have you called your Senator for their support in the Lymphedema Treatment Act? Call 202-224-3121 and follow instructions, OR go to lymphedematreatmentact.org.
Sources
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC151891/
m.pnas.org/content/98/22/12677.long
stemcellsportal.com/Stem%20Cell%20Injections%20Help%20Woman%20with%20Lymphedema%20Caused%20by%20Cancer%20Treatment
discovery.lifemapsc.com/library/review-of-medical-embryology/chapter-128-development-of-the-lymphatic-system
lymphedema.pitt.edu/research.update.php
www.cdc.gov/parasites/lymphaticfilariasis/biology_w_bancrofti.html
www.medicinenet.com/lymphedema/article.html
About the Author
Janet Wolfson is a wound care and lymphedema educator with ILWTI, and Lymphedema and Wound Care Coordinator at Health South of Ocala with over 30 years of field experience.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.