Lymphedema / Phlebolymphedema
Lymphedema (alternate spelling: lymphoedema) is a condition marked by the retention of interstitial fluid (lymph) and the swelling (edema) of surrounding soft tissue, often affecting the extremities. It is also referred to as lymphatic obstruction.
The lymphatic system is responsible for carrying interstitial fluid originating from the blood to the right lymphatic duct and the thoracic duct, also known as the left lymphatic duct, and then back into the bloodstream. En route, the lymph (interstitial fluid) is passed through several secondary lymphoid organs, such as the lymph nodes, where lymphocytes (a specific type of white blood cell) defend the patient against bacteria that has been picked up along the way. The lymphatic system is not closed and has no centralized mechanism for circulation, unlike the cardiovascular system. Therefore, the transport of lymph is slow and erratic, relying on peristalsis (propagating contractions in smooth muscles used to push contents along the digestive tract), compression of the interstitial fluid from the contraction of nearby skeletal muscles and pulsation of nearby arteries, and a series of valves in the lymphatic channels preventing the lymph from flowing backwards. However, if the hydrostatic pressure within these channels becomes too high, for example due to enlarged lymph nodes or obstruction of the vessel by a nearby tumor, lymph can build up in the interstitial space, causing the surrounding tissue to swell. Another common cause of slowed lymph flow is the lack of muscles contracting, often due to immobility.
Phlebolymphedema results from mixed venous and lymphatic insufficiency. In the presence of venous hypertension, the increase in lymphatic burden becomes greater than the transport capacity of the lymphatic system.
Symptoms of Lymphedema / Phlebolymphedema
In the affected limb:
- Swelling of part or the entire limb, including the digits
- Heaviness or tightness
- Weakness
- Diminished joint flexibility
- Aching or discomfort
- Recurring infections
- Hardening, thickening, or discoloration of the overlying skin
In the head or neck: localized lymph accumulation.
Note: Symptoms of lymphedema can occur several years following injury to the lymphatic system, or more quickly if there is injury to or infection of the affected limb.
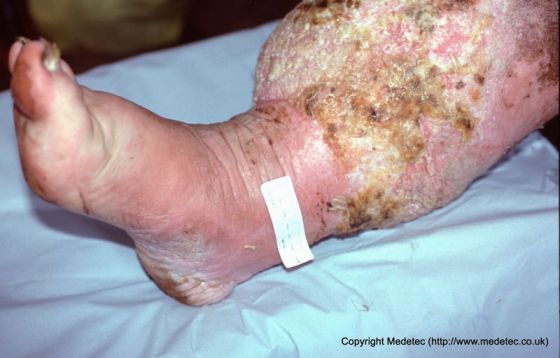 Figure 1
Figure 1
Etiology
Primary lymphedema results from the abnormal development of the lymphatic system, often due to abnormal or missing lymph nodes or channels. Secondary lymphedema is caused by damage to the lymphatic system, most commonly from dissected lymph nodes as a result of cancer surgery. Other common causes of damage are infection, injury, radiation, and scar tissue resulting from radiation or surgery.
In the United States, the most common cause of lymphedema is damage to the lymphatic system resulting from breast cancer surgery, especially when followed by radiation therapy.
Worldwide, the most common cause of lymphedema is a parasitic infection called filariasis (philariasis), affecting millions of people in the sub-tropics and tropics of Africa, Asia, the Western Pacific, and certain regions of Central and South America.
Risk Factors
- Axillary surgery and/or axillary radiation therapy for breast cancer
- Lymph node removal
- Sentinel node biopsy
- Obesity
- Local surgery
- Local radiation
- Delayed wound healing or burns
- Extensive or localized trauma
- Tumor causing lymphatic obstruction
- Scarring of the lymphatic ducts by either surgery or radiation
Complications
The most serious and prevalent complication resulting from lymphedema is the increased vulnerability of the affected limb to infections. Any injury to the limb is a potential gateway to infection. Two common forms of infection are cellulitis, an inflammation of connective tissue as well as the dermal and subcutaneous layers of the skin, and lymphangitis, the inflammation of the lymphatic channels, also referred to as "blood poisoning".
Lymphangiosarcoma, a rare soft tissue cancer affecting the lymphatic vessels, can also result from severe cases of chronic lymphedema.
Diagnostic Studies
- Lymphoscintigraphy
- Magnetic resonance imaging (MRI)
- Bioimpedance Spectroscopy or Electrical Impedance Tomography
Treatments & Interventions for Lymphedema / Phlebolymphedema
The following precautions can help minimize the risk of developing lymphedema in at-risk patients and to minimize complications in patients already exhibiting symptoms:
- Clean the affected area daily with a pH neutral and unscented soap, monitoring for signs of infection, and apply moisturizers afterwards to prevent dry, cracked skin.
- Thoroughly clean wounds apply antibiotics (if physician prescribed) and monitor for signs of infection.
- Wear gloves while cooking, gardening and other activities with heat and sharp objects to reduce the risk of cuts, burns and scrapes.
- Likewise, use an electric razor to shave in order to reduce the risk of cuts and skin irritation
- Avoid going barefoot.
- Avoid tight clothing and jewelry that could constrict the affected limb.
- Avoid applying heat to the affected limb, including heating pads, hot tubs, or steam baths.
- Keep the affected limb above your heart when possible.
- Avoid heavy lifting or strenuous activity with the affected limb.
- During activity, monitor the affected limb for any change in size, shape, tissue, texture, soreness, heaviness, or firmness.
- Pay particular attention to the limb during air travel, as the decrease in pressure and extended time seated can exacerbate existing lymphedemic conditions. Consider wearing a compression garment for such travel.
- If possible, avoid medical procedures such as vaccinations, blood draws, and blood pressure readings in the affected limb.
- For patients at risk of developing lymphedema in the lower extremities, avoid crossing your legs while sitting as well as sitting or standing for extended periods. Similarly, for patients at risk for upper extremity lymphedema, avoid carrying heavy bags or purses on the affected arm.
While there is no cure for lymphedema, treatments exist to minimize discomfort and reduce the swelling in the affected area. Several forms of compression treatments are available to reduce swelling and prevent scarring of the overlying skin, including:
- Static and dynamic compression devices, which provide a pressure gradient encouraging the flow of lymph from the end of the limb towards the trunk
- Manual compression, a form of massage also known as manual lymph drainage
- Light exercise used to gently stimulate the muscles in limb to increase lymph flow.
- The use of compression garments such as hosiery and sleeves for static compression.
Surgical treatments are also used in extreme cases of lymphedema to improve mobility by removing excess tissue. Lymph node transfers and lymphovenous bypasses are available to greatly reduce lymphedema.
References
Mayo Foundation for Medical Education and Research. Lymphedema. Mayo Clinic. http://www.mayoclinic.com/health/lymphedema/DS00609. Published November 15, 2011. Accessed August 3, 2012.
National Institutes of Health. Lymphedema (PDQ). National Cancer Insitute. http://www.cancer.gov/cancertopics/pdq/supportivecare/lymphedema/Patient. Updated August 19, 2011. Accessed August 3, 2012.
Society for Vascular Surgery. Lymphedema. VascularWeb. https://www.vascularweb.org/vascularhealth/Pages/lymphedema.aspx. Updated December 2011. Accessed August 3, 2012.
Stoppler MC. Lymphedema. MedicineNet.com. http://www.medicinenet.com/lymphedema/article.htm. Updated September 20, 2012. Accessed August 3, 2012.
Thiadens SRJ. A Brief Overview. National Lymphedema Network. http://www.lymphnet.org/lymphedemaFAQs/overview.htm. Accessed August 3, 2012.







