Wound Odor
Wound odor, also referred to as malodor, is typically the result of necrotic tissue or bacterial colonization in the wound bed. Certain dressings like hydrocolloids, also tend to produce a characteristic odor as a result of the chemical reaction that takes place between the dressing and wound exudate, causing odor. While not directly harmful to the patient, wound odor is often indicative of bioburden or other barriers to wound healing. In addition, the psychological effects of malodorous wounds on the patient, relatives, or caregiver can be significant.
Assessment of Wound Odor
Though there is no universally recognized scale for measuring wound odor, the following can be used to qualitatively assess wound odor for documentation purposes:
Very strong: Odor is evident on entering the room (6–10 feet or 2–3 meters from the patient) with the dressing intact.
Strong: Odor is evident on entering the room (6–10 feet or 2–3 meters from the patient) with the dressing removed.
Moderate: Odor is evident at close proximity to the patient when the dressing is intact.
Slight: Odor is evident at close proximity to the patient when the dressing is removed.
No odor: No odor is evident, even at the patient’s bedside with the dressing removed.
From: Haughton and Young (1995)
Etiology
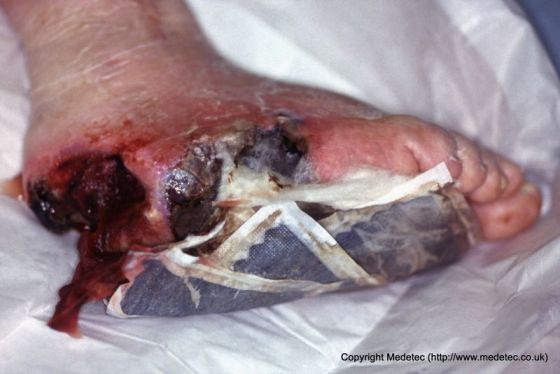
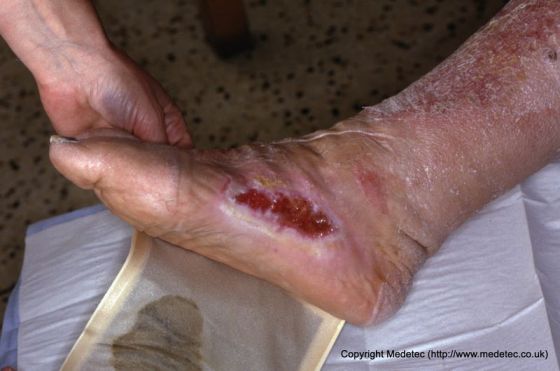
Most wound odors are thought to arise from the metabolic processes of anaerobic bacteria. In chronic wounds; such as pressure ulcers, leg ulcers, and diabetic foot ulcers, the odor may also be due to tissue degradation. The aptly named, foul-smelling compounds called cadaverine and putrescine, are released by anaerobic bacteria as part of the putrefaction of tissue.
Treatment of Wound Odor
Implementing one or more of the following precautions can help minimize the risk of developing malodorous wounds in at-risk patients and minimize complications in patients already exhibiting symptoms:
- Cleanse the wound as often as advisable to reduce bioburden
- Ensure the patient is practicing good hygiene
- If not contraindicated, increase the frequency of dressing changes
- Change bed linen as soon as it becomes soiled
- Use products designed to decrease or mask odor (i.e., calcium alginate)
- Use cleansers designed to break through biofilm or bioburden
- Use wound cleansing products that are biocides designed to kill odor causing bacteria
Treatment of malodorous wounds is typically aimed at treating the underlying infection or debridement of the devitalized tissue responsible for the odor. While topical or systemic antibiotics may be effective, it is difficult to reach the necessary concentration of antibiotics at the infection site. One formulation that has found wide use in the wound care community is metronidazole gel or powder, which even though it is most effective against anaerobic bacteria may have some effect on a range of aerobic organisms at the concentrations typically used.
If it is not feasible to eradicate the cause of the wound odor, odor-controlling dressings can help mitigate the psychological effects of excessive wound odor. Activated charcoal is widely used as a deodorizing agent in dressings for these purposes. Cleansing and/or debridement of the wound may be necessary before applying the dressing to achieve the desired effect. If these measures are not enough by themselves to mitigate odor from the wound in question, external deodorizers (air fresheners, scented candles, essential oils, coffee grounds, etc) can be used to mask the odor.
References
Holloway S. Recognising and treating the causes of chronic malodorous wounds. Nursing Times. http://www.nursingtimes.net/recognising-and-treating-the-causes-of-chron.... Published March 1, 2004. Accessed July 28, 2017.
Thomas S, Fisher B, Fram P, Waring M. Odour Absorbing Dressings: A comparative laboratory study. World Wide Wounds. http://www.worldwidewounds.com/1998/march/Odour-Absorbing-Dressings/odou.... Published April 7, 1998. Accessed July 28, 2017.
Image Source: copyright Medetec (www.medetec.co.uk). Used with permission.






