Alternatives to the Total Contact Cast in Managing Diabetic Foot Ulcers
March 29, 2018
Editor's note:This blog post is part of the WoundSource Trending Topics series, bringing you insight into the latest clinical issues and advancement in wound management, with contributions by the WoundSource Editorial Advisory Board.
According to the American Diabetes Association, there are 29.1 million Americans with diabetes, 8.1 million of whom are walking around undiagnosed.1 This number is dwarfed by the 86 million Americans who have been classified as having prediabetes and who are at risk for developing diabetes in the near future. Each year, 1.7 million Americans age 20 years or older — 4,660 per day, or one every 19 seconds — are added to the rolls and begin a slow but steady acquisition of the devastating complications of the disease.
Medical science has come a long way in treating the disease, but despite our advances, complications such as hypertension, dyslipidemia with accompanying cardiac disorders such as cardiovascular disease including heart attack, and stroke still occur. It also leads to peripheral vascular disease with progressive loss of peripheral circulation that disproportionally affects the lower extremities. Small-vessel disease leads to eye problems, or even blindness, kidney disease, and glycosylation of the nervous system that leads to progressive peripheral neuropathy with a loss of peripheral protective sensation that often leads to ulceration and/or amputation.1
Looking at the "Gold Standard" of Treatment
Offloading the neuropathic foot is the cornerstone of diabetic wound management, and the total contact cast (TCC) has been recognized as the “gold standard” for treatment for decades.2-7 The success of the TCC has been attributed to its ability to “unload” the plantar foot and maintain immobilization by the non-removable cast. Reducing plantar pressures allows for unimpeded wound healing and achieves complete closure in most wounds by 12 weeks. A high recurrence rate plagues these wounds, and failure to transition patients to their final footwear often has them back in the clinic in a short period of time. The use of an appropriate shoe-foot interface to achieve a redistribution of forces from areas prone to ulceration to the remainder of the foot has not been adequately studied, except for the total contact molded innersole, and countless devices, techniques, and modifications have been tried with varying success.8-14
These have included total contact insoles, pixelated offloading insoles, segmented diabetic healing shoes and insoles, and innovative sole designs for depth footwear for everyday use. TCC "kit" systems have been developed by several companies to streamline the application of the modality and increase its use by practitioners who have been slow to embrace the TCC despite convincing research to validate its use.
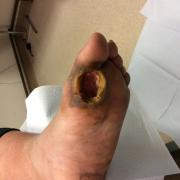 Image Credit: James McGuire. All rights reserved.
Image Credit: James McGuire. All rights reserved.The TCC is underutilized in daily practice.15,16 In an analysis of data from the wound registry, Fife et al.16 found that only 6% of patients with a diabetic foot wound received treatment with a TCC. Similarly, after surveying 895 clinics, Wu et al.15 concluded that only 1.7% of centers routinely use TCCs, and a majority of centers surveyed did not consider the TCC as the gold standard for treating a non-infected diabetic foot ulceration. The most commonly used offloading device by clinicians (41.2%) was a shoe-based system, with patient intolerance (55.3%), clinic application time (54.3%), cost of materials (31.6%), reimbursement issues (27.5%), lack of familiarity with the TCC (25%), and clinician coverage (10.6%) the most common reasons.15 Many clinicians have a fear of complications associated with TCC use, despite research to the contrary.17 This has led me to question the "gold standard" label given to the TCC and suggest that is not the TCC but the fact that it is non-removable that makes it the gold standard. The gold standard is therefore the non-removability of the device, and not the magic of the TCC itself.
Alternative Solutions to the Total Contact Cast
The International Working Group on the Diabetic Foot (IWGDF) released a guideline in 2015 with recommendations on footwear and offloading interventions to prevent and heal foot ulcers in patients with diabetes.18 We use the guideline to apply evidence-based clinical decision making to our approach to offloading. Choosing an appropriate offloading device is not as simple as ordering your patient into a TCC. As we have seen, there are numerous barriers to the routine use of the TCC. Even if you are fortunate enough to have your patient agree to the application of the TCC, there need to be transitional devices used between the cast and the patient’s final shoe.
The strongest recommendation from the IWGDF with the highest quality of evidence is to offload with a non-removable knee-high device (TCC or iTCC) with an appropriate foot-device interface, such as a total contact sole or tested interface device such as a pixelated innersole.18 The iTCC was developed by Dr. David Armstrong and is simply a removable cast walker made non-removable by wrapping it in self-adherent wrap or cast material or by using a cable tie connector to prevent removal by the patient. When those can’t be used, alternative non-removable devices such as the Rader football dressing or the felted foam dressing can be substituted. When a knee-high device (removable or non-removable) is contraindicated or cannot be tolerated by the patient, the IWGDF recommends offloading with a forefoot offloading shoe, a cast shoe, or a custom-made temporary shoe,18 but the evidence for this is weak and it should be considered only when the patient can be expected to be adherent to wearing the shoes. This is an unlikely scenario when you consider that when patients are able to remove their offloading devices, they wear them during less than 30% of their total daily activity.19
Proper Care Following the Removal of the Restrictive Offloading Device
At some point during the management of the wound, a restrictive offloading device must be removed. At that time, a decision must be made about whether the patient can return to the final offloading footwear or whether a transitional device will be required. I developed the concept of transitional offloading back in 2006, when I recommended a step-down approach to offloading the diabetic foot. Following the IWGDF guidelines, I begin with a knee-high non-removable device and, around the time of wound resolution, transition to a removable device to evaluate how the patient performs with cast breaks for bathing, sleeping, and early range-of-motion exercises.
Rapid transition to standard footwear after the wound closes, regardless of the patient’s insistence, may contribute to wound recurrence,20 so transition to a shoe-based device with an appropriate foot-device interface should be monitored carefully. If at any time during the process there is a setback to the patient’s ulcer healing progression, the patient should revert to the previous level of offloading until the wound improves. Devices such as the Carville healing sandal or a rocker-bottom surgical shoe with a pixelated offloading insole can be considered for transitional offloading to allow for ambulation with a free ankle. Shoe-based offloading systems allow the skin to thicken and mature during the 3- to 4-week period after closure of the wound but still maintain a level of protection and control of activity.
Depth shoes that have molded inserts should not be used during this stage because they encourage the patient to use a normal gait and ambulate at a faster pace; however, once the wound has remained closed for 3 to 4 weeks, the patient can be transitioned to these shoes for their permanent footwear.20
References
1. American Diabetes Association. Statistics About Diabetes. http://www.diabetes.org/diabetes-basics/statistics/. Accessed on February 27, 2018.
2. American Diabetes Association. Consensus development conference on diabetic foot wound care: 7–8 April 1999, Boston, Massachusetts. Diabetes Care. 1999;22:1354–60.
3. Coleman W, Brand PW, Birke JA. The total contact cast: a therapy for plantar ulceration on insensitive feet. J Am Podiatr Med Assoc. 1984;74:548–52.
4. Total contact casting in diabetic patients with neuropathic foot ulcerations. Arch Phys Med Rehabil. 1984;65:691–3.
5. Walker SC, Helm PA, Pulliam G. Total contact casting and chronic diabetic neuropathic foot ulcerations: healing rates by wound location. Arch Phys Med Rehabil. 1987;68:217–21.
6. Sinacore DR, Mueller MJ, Diamond JE. Diabetic plantar ulcers treated by total contact casting. Phys Ther. 1987;67:1543–7.
7. Mueller MJ, Diamond JE, Sinacore DR, et al. Total contact casting in treatment of diabetic plantar ulcers: controlled clinical trial. Diabetes Care. 1989;12:384–8.
8. Cavanagh PR, Bus SA. Off-loading the diabetic foot for ulcer prevention and healing. J Vasc Surg. 2010;52:37S–43S.
9. Armstrong DG, Lavery LA. Evidence-based options for offloading diabetic wounds. Clin Podiatr Med Surg. 1998;15:95–104.
10. Shaw JE, Hsi WL, Ulbrecht JS, Norkitis A, Becker MB, Cavanagh PR. The mechanism of plantar unloading in total contact casts: implications for design and clinical use. Foot Ankle Int. 1997;18(12):809–17.
11. McGuire JB. Pressure redistribution strategies for the diabetic or at-risk foot: part I. Adv Skin Wound Care. 2006;19(4):213–21; quiz 222–3.
12. McGuire JB. Pressure redistribution strategies for the diabetic or at-risk foot: part II. Adv Skin Wound Care. 2006;19(5):270–7; quiz 277–9.
13. Bus SA, Valk GD, van Deursen RW, et al. The effectiveness of footwear and offloading interventions to prevent and heal foot ulcers and reduce plantar pressure in diabetes: a systematic review. Diabetes Metab Res Rev. 2008;24 Suppl 1:S162–80.
14. Mrdjenovich DE. Off-loading practices for the wounded foot: concepts and choices. J Am Col Certif Wound Spec. 2011;2(4):73–8.
15. Wu SC, Jensen JL, Weber AK, Robinson DE, Armstrong DG. Use of pressure offloading devices in diabetic foot ulcers: do we practice what we preach? Diabetes Care. 2008;31(11):2118–9.
16. Fife CE, Carter MJ, Walker D. Why is it so hard to do the right thing in wound care? Wound Repair Regen. 2010;18(2):154–8
17. Guyton GP. An analysis of iatrogenic complications from the total contact cast. Foot Ankle Int. 2005;26(11):903–7.
18. International Working Group on the Diabetic Foot. IWGDF Guidance on Footwear and Offloading Interventions to Prevent and Heal Foot Ulcers in Patients With Diabetes. http://www.iwgdf.org/files/2015/website_footwearoffloading.pdf. Accessed February 27, 2018.
19. Armstrong DG, Lavery LA, Kimbriel HR, Nixon BP, Boulton AJ. Activity patterns of patients with diabetic foot ulceration: patients with active ulceration may not adhere to a standard pressure off-loading regimen. Diabetes Care. 2003;26(9):2595–7.
20. McGuire J. Transitional off-loading: an evidence-based approach to pressure redistribution in the diabetic foot. Adv Skin Wound Care. 2010;23(4):175–88.
About the Author
Dr. James McGuire is the director of the Leonard S. Abrams Center for Advanced Wound Healing and an associate professor of the Department of Podiatric Medicine and Orthopedics at the Temple University School of Podiatric Medicine in Philadelphia. Dr. McGuire has over 30 years of experience in wound management and lectures both nationally and internationally in the areas of wound healing, diabetic foot management, off-loading, and biomechanics of the at-risk foot.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.








