Case Study: Total Knee Replacement Patient with Wound Dehiscence Due to Lymphedema
September 14, 2016
If you read my last blog on therapeutic interventions to stimulate wound healing, then you may recall the asset that a lymphedema trained therapist can be to your wound care department. A recent patient at the inpatient rehab facility where I am currently the Wound Care Coordinator illustrates this wonderfully.
Managing Wound Dehiscence with Chronic Lymphedema
Patient L entered our facility from an acute care hospital. She had already failed discharge home and arrived with a diagnosis of incision and drainage of her infected knee replacement with heavy wound drainage. She required more than one dressing change per day (even with wicking ultra-absorbent dressings). Her topical dressing was changed to a post-op negative pressure wound therapy (NPWT) dressing at 125mmHg continuous. The dressing was applied in a partially flexed position to allow range of motion (ROM) exercises. Output required changing the 300ml canister BID. Her comorbid diagnosis of chronic lymphedema was obviously slowing the healing of her surgical incision such that even the NPWT pump could not keep up with it. Her physicians cleared her for Manual Lymphatic Drainage (MLD) and multilayer compression bandaging when an ABI showed adequate arterial circulation.
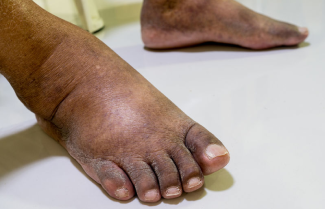
An assessment of her lymphedema revealed she was in the Chronic Stage (3) with positive Stemmer Sign (pinched skin above second toe is unable to be lifted from subcutaneous structures), fibrosis in the ankle area, scarring from previous wounds in lower leg as well as posterior thigh edema. In addition, she was morbidly obese and had osteoarthritis. She was further educated regarding lymphedema and the components of her Complex Lymphatic Therapy (CLT).
A Multifaceted Approach to Healing a Surgical Wound
The first step in the program was to apply multilayer compression bandaging to the knee. The NPWT tubing was padded to prevent pressure buildup of tubing on her skin. Because she needed to work on knee ROM and the multilayer bandages would have compromised her balance, her thigh/knee wraps were modified. An abdominal binder was applied around her thigh and knee. It could easily be removed for gait, mobility and therapeutic exercises and reapplied promptly by the patient or any staff member.
The second component was manual lymphatic drainage (MLD) combined with decongestive exercise. This entailed deep breathing, decongestion of the axillary and abdominal lymph nodes and venous angles as well as establishing an alternative drainage path for the lymph congested in her legs and abdominal panus. Modification of her post-op total knee replacement program with respect to her lymphedema was discussed with her rehab therapists. Ms. L was educated in self-MLD prior to her OT and PT therapeutic exercise and lower extremity elevation was incorporated into her rehab whenever possible.
The patient was educated in meticulous skin care: prevention of fungal infections and spreading of them during bathing, symptoms of infection, and selection of appropriate bathing and skin care products. The occupational therapist incorporated this into her adaptive activities of daily living (ADL) activities.
The above program resulted in reduction in limb girth as well as a gradual closing of her incision. By discharge date, the incision was minimally exuding. Due to hygienic issues at home, the NPWT was continued for a short period post discharge to completely close the wound. Home care staff would continue the compression bandaging and CLT program. Compression garment options and donning devices were discussed with the patient.
Payment for an expensive custom garment was a concern. So in addition, the Lymphedema Treatment Act (LTA) was discussed with the patient as the non-coverage for compression garments by Medicare and Insurance had affected her health and recovery from the total knee replacement. She indicated that she would support the passage of the LTA and do what she could to obtain a garment on her own. Had the patient been treated for her chronic lymphedema prior to joint replacement surgery and had she worn custom compression garments during her recovery period, the dehiscence and infection that complicated her post-op rehabilitation might have been avoided.
About the Author
Janet Wolfson is a wound care and lymphedema educator with ILWTI, and Lymphedema and Wound Care Coordinator at Health South of Ocala with over 30 years of field experience.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.