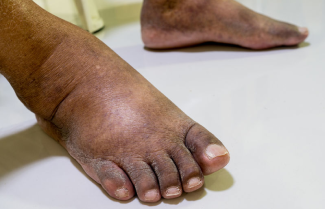
Compression Garment Selection for Kidney Failure-Related Edema
June 16, 2017
Acute care wound or edema professionals are bombarded with multiple kinds of edema that can be treated in many ways—and with many choices of compression garments. What to choose?
Edema Identification
The first issue to solve is: what kind of edema is swelling these legs? If kidneys are part of the issue, knowing the Glomerular Filtration Rate (GRF), which is a measure of kidney function to stage the degree of failure, can inform how tolerant the patient may be to compression (See Table 1).
Consulting the patient’s nephrologist (if available) is the best option. Patients in moderate to severe kidney failure may need modifications to not place undue burden on the kidneys. Staging the wraps one leg at a time, moving forward gradually, may be the only way to slowly and carefully decongest the legs.
Choosing the Right Compression Garment
Appropriate compression garments should then complete the decongestion program. Skin in “watery” edema, such as kidney or heart failure, can be very frail and easily torn. Struggling to put on traditional compression knee or thigh highs can result in skin tears. Using a donning aid or other assistive device can assist in gently applying the compression stocking, as it rolls the stocking up or off the leg.
Nontraditional compression garments, such as adjustable or other easy-to-don compression products, may offer gentle solutions as well – no pulling and tugging is necessary!
Working in conjunction with dialysis days is very effective. The patient is dialyzed, and then the wraps are reapplied. This should be done in consultation with the kidney specialist. A reduction garment can allow the garment to be easily adjusted (following the filtration) to maintain volume reduction. They would also allow for fluctuation in edema between dialysis treatments. The patient will need to be able to tolerate the accumulation of fluid above the level of the compression garment and/or eventually add a garment to include the thigh.
Kidney failure patients should absolutely be approached with compression cautiously - and in consultation with their physicians. Their compression garments need to be prescribed thoughtfully. When used appropriately, compression can improve quality of life through protection from skin tears and the reduction of water weight in the legs.
Table 1: Glomerular Filtration Rate and Kidney Failure Staging

About the Author
Janet Wolfson is a wound care and lymphedema educator with ILWTI, and Lymphedema and Wound Care Coordinator at Health South of Ocala with over 30 years of field experience.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.