Dressing Change Tips Every Clinician Should Know to Help Prevent MARSI
July 21, 2017
Wounds are dressed every day, and much goes into the choices that are made to properly apply wound dressings. The condition of the periwound skin should be a major factor in the decisions made, as injuring this area can extend the wound and cause considerable pain. Tape removal is one of the most painful areas of wound care.1
Dressing Down: Preventing MARSI is Every Clinician's Responsibility
Periwound skin is affected by the dressing choice in several ways. If the wound is wet or the dressing is unable to manage the exudate, then the periwound skin may macerate. Exudate lying on the skin may also cause irritation, itching, and inflammation. Thirdly, the dressing product used (or the adhesive incorporated into it) may cause a localized sensitivity reaction. Last but definitely not least there is iatrogenic damage caused by the dressing application or removal, also known as tape stripping and medical adhesive-related skin injury (MARSI). Not only are dressings responsible for MARSI, but also any adherent device—from catheter securement devices to electrodes. Different adhesives have different properties, and some are more likely than others to damage skin. A company merely stating that a border dressing is safer on the skin does not necessarily make it so. There has been much press given to safer adhesive technology, and a little less to other aspects of reducing the possibility of MARSI.
Tips for Preventing Medical Adhesive-Related Skin Injury During Dressing Changes
Earlier this year, Yates et al set the standard for MARSI interventions.2 Interestingly, the mechanics of proper adhesive removal were found very difficult to describe, though maybe this is understandable in the setting of a consensus approach. Common sense and pictures may better convey some dos and don'ts, at the risk of being less agreeable to some. You can decide how you learn best. The term tape is used below for border dressing, semi-permeable transparent films, and negative pressure wound drape.
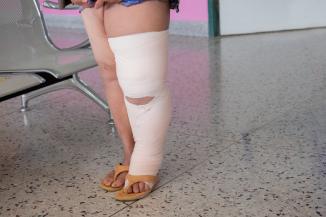
- If the periwound skin is not healthy, use a wrap net or support garment. If a wrap is used on the lower leg, it should generally go from the base of the toes to above the calf, at mild compression unless contraindicated (severe arterial disease).
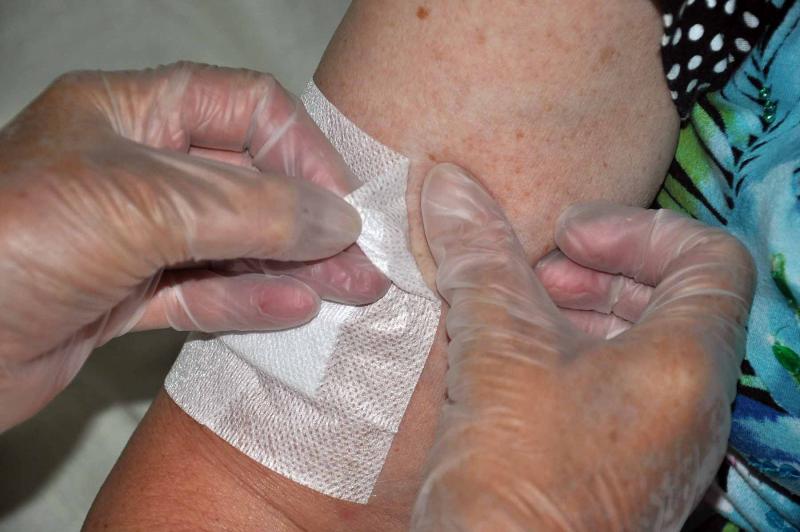
- Most dressings should be fully covered with tape, not picture framed, as this supports the dressing better. Fully taping lessens evaporative heat loss, encourages moist wound healing, and reduces contamination and cross infection risk.
- Only sufficient tape to secure the dressing should be on the skin, and should be placed considering the Langer lines to reduce tension and promote comfort. Some tapes have more "give" one way, and this too should be in the direction of the Langer lines.
- Removing backing paper as the tape is pulled can stretch the skin. Stretching the skin to apply tape delivers stress that not only can shear the skin layers, but can also cause significant skin pain. Skin pain can be a major reason for pain from negative pressure wound therapy.
- Post-operative blisters may be caused by edema or by stretched tape.
- Applying tape with no tension is very important. Turning back a tab makes removal easier.
- Skin prep, barrier wipes, and sprays are meant to form a layer over the skin that protects it. They should be allowed to dry fully to function optimally and protect the skin on removal of the tape. Not allowing skin prep to dry when applying a condom catheter should be a dismissible offense!
- To improve adhesion of devices, such as ostomy appliances, warmth and pressure work well. Rubbing shreds the adhesive and should be discouraged. Skin barrier wipes (skin prep) smooth out the natural, tiny skin contours that improve the qualities of the adhesive in the hydrocolloid barrier, and are generally not necessary.
- Peeling back a dressing to look at a wound (and replacing it) increases the possibility of dislodgement and risk of bacterial contamination, and should be avoided.

Finally, adhesive remover wipes are designed to remove adhesives. They work. Use them. Sadly, most are tiny pads - they need to come in a larger size! Tape removal is one of the most painful parts of a dressing change. The pain caused is held in memory, and increases pain and anxiety at subsequent procedures. Please use adhesive remover wipes and take time to remove tape. Your patients will thank you. Image Credit: Margaret Heale. Used with Permission
References
1. Denyer, J., Reducing pain during the removal of adhesive and adherent products., in British Journal of Nursing. 2011. p. S28-S35.
2. Yates, S.M., L; Heineche, SB; Gray, M., Embracing the Concept, Defining the Practice and Changing the Outcome. Journal of Wound, Ostomy and Continence Nursing, 2017. 44(1): p. 13-17.
About the Author
Margaret Heale has a clinical consulting service, Heale Wound Care in Southeastern Vermont and draws on her extensive experience as a wound, ostomy and continence nurse in acute and long-term care settings to provide education and holistic care in her practice.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.