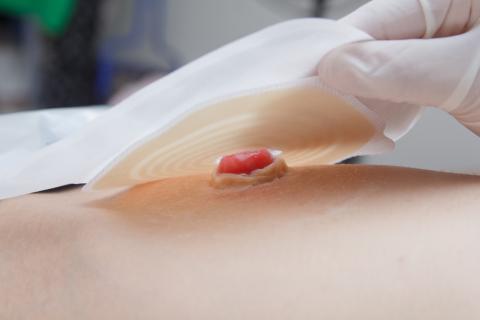
Examining Convexity in Ostomy Management
May 7, 2026
Understanding the role of convexity in pouching systems is critical for improving fit, reducing complications, and supporting better long-term outcomes.
Key Takeaways
-
Peristomal skin complications affect up to 73% of ostomy patients, driving increased healthcare utilization and costs, with leakage as a primary contributing factor.
-
Convexity plays a crucial role in improving pouch seal and reducing leakage, particularly in patients with challenging peristomal anatomy, yet remains inconsistently applied in practice.
-
Advancing clinician assessment skills in convexity selection is essential for improving patient outcomes, enhancing quality of life, and supporting value-based care initiatives.
Ostomy creation is a common surgical intervention, with an estimated 725,000 to 1 million people living with an ostomy in the United States alone, and approximately 100,000 new ostomy surgeries performed annually.1,2 As survival rates improve for colorectal cancer, inflammatory bowel disease (IBD), and other conditions requiring diversion, the population requiring long-term ostomy management continues to expand.3
Despite advances in surgical technique and ostomy products, complications remain highly prevalent. Peristomal skin complications (PSCs) are among the most common issues, affecting between 36% and 73% of ostomy patients.4-6 These complications include irritant dermatitis, moisture-associated skin damage (MASD), and mechanical injury—all of which are frequently linked to poor pouch seal and leakage.
From a health system perspective, PSCs are not benign. They are associated with increased healthcare utilization, including more frequent clinic visits, higher supply usage, and, in severe cases, hospital readmissions.5 One study estimated that patients with PSCs incur significantly higher ostomy-related healthcare costs compared to those without complications, driven largely by the need for additional interventions and product changes.7
For wound care professionals, these statistics underscore a critical need: improving ostomy management is not just about comfort—it is directly tied to patient safety, outcomes, and cost containment.
Leakage: A Persistent and Underrecognized Driver of Poor Outcomes
Leakage remains one of the most frequently reported and distressing complications among patients with an ostomy. Surveys indicate that up to 62% of individuals with an ostomy experience leakage at some point, with many reporting recurrent episodes.8
The clinical implications of leakage extend beyond inconvenience. Chronic exposure of peristomal skin to effluent can lead to rapid skin breakdown due to enzymatic and chemical irritation, particularly in ileostomy patients where output is more caustic.4 This creates a cyclical problem: compromised skin further impairs pouch adhesion, increasing the likelihood of additional leakage.
From a psychosocial standpoint, leakage is strongly associated with reduced quality of life. Patients frequently report anxiety, social withdrawal, and decreased confidence in daily activities due to fear of visible leaks or odor.9 These concerns can lead to decreased adherence to care routines and reluctance to engage in follow-up care, compounding clinical risks.
Given that leakage is often preventable with optimal pouch fit and seal, it represents a key modifiable factor in improving both clinical and patient-reported outcomes.
The Role of Convexity in Addressing Anatomical Challenges
Convexity—defined as the outward curvature of the skin barrier designed to improve stoma protrusion and seal—has emerged as a critical tool in ostomy management. Its primary function is to compensate for challenging peristomal topography, such as retracted stomas, skin folds, or uneven abdominal contours.
Anatomical variability is a major contributor to pouching difficulties. Studies suggest that a significant proportion of ostomy patients have non-ideal stoma characteristics, including flush or retracted stomas, which increase the risk of leakage.10 Additionally, factors such as obesity, postoperative edema, and scar tissue can further complicate pouch adherence.
Convex pouching systems are specifically designed to address these challenges by applying gentle pressure around the stoma, promoting protrusion and enhancing the seal. Clinical consensus statements emphasize that appropriate use of convexity can significantly reduce leakage and improve wear time.11
However, despite its recognized benefits, convexity remains underutilized or inconsistently applied in practice. Variability in clinician training, uncertainty in assessment, and lack of standardized guidelines contribute to gaps in optimal use.11,12
Variability in Clinical Assessment: A Key Gap in Practice
One of the most significant barriers to effective ostomy management is inconsistency in peristomal assessment. Unlike other areas of wound care where standardized assessment tools are widely adopted, ostomy care often relies on clinician judgment, which can vary based on experience and training.
Research indicates that improper product selection—including inappropriate use or underuse of convexity—is a leading contributor to leakage and PSCs.6 In many cases, clinicians may delay introducing convexity due to concerns about pressure injury or lack of confidence in identifying appropriate candidates.
At the same time, emerging evidence suggests that early and appropriate use of convexity does not increase complication rates and may, in fact, reduce the incidence of PSCs when used correctly.11 This highlights a critical need for education focused on assessment skills and decision-making frameworks.
For wound care professionals, strengthening these competencies is essential to delivering consistent, high-quality care across diverse patient populations.
Impact on Quality of Life and Patient Confidence
Beyond clinical outcomes, ostomy management has profound implications for patient quality of life. Studies consistently show that ostomy-related complications—particularly leakage and skin issues—are among the strongest predictors of reduced health-related quality of life.9
Patients with poorly managed ostomies often experience:
-
Decreased social participation
-
Increased anxiety and depression
-
Reduced physical activity
-
Challenges with employment and daily functioning
Conversely, effective pouching systems that minimize leakage and protect skin integrity are associated with improved confidence and independence.9
Convexity, when appropriately applied, plays a central role in achieving these outcomes by enhancing pouch reliability. For many patients, the difference between a well-fitting system and a poorly fitting one can determine their ability to engage fully in daily life.
The Economic Imperative for Optimized Ostomy Care
The financial implications of suboptimal ostomy management are substantial. In addition to direct medical costs, indirect costs such as lost productivity and caregiver burden contribute to the overall economic impact.
Studies have shown that PSCs alone can increase ostomy-related care costs by hundreds to thousands of dollars per patient annually.7 When scaled across the growing ostomy population, this represents a significant burden on healthcare systems.
Improving pouch fit and reducing complications through better assessment and product selection—including the appropriate use of convexity—offers a clear opportunity for cost savings. This aligns with broader healthcare priorities; value-based care and outcome optimization.
Elevating Practice Through Focused Education on Convexity
The importance of convexity in ostomy management lies not only in its clinical utility but in its role as a marker of advanced assessment and decision-making. Understanding when and how to use convexity requires a nuanced appreciation of anatomy, product design, and patient-specific factors.
In a field where small adjustments can have significant impacts, the ability to optimize pouch fit represents a critical competency.
References
- United Ostomy Associations of America. Ostomy statistics. Accessed May 6, 2026. https://www.ostomy.org/ostomy-statistics/
- Colwell JC, Pittman J, Raizman R, Salvadalena G. A randomized controlled trial determining variances in ostomy skin conditions and the economic impact (ADVOCATE trial). J Wound Ostomy Continence Nurs. 2021;48(1):50-57.
- Bray F, Laversanne M, Weiderpass E, Soerjomataram I. The global cancer burden 2020: GLOBOCAN estimates of incidence and mortality worldwide. CA Cancer J Clin. 2021;71(3):209-249.
- Salvadalena G. Incidence of complications of the stoma and peristomal skin among individuals with ostomies. J Wound Ostomy Continence Nurs. 2020;47(5):423-428.
- Nichols TR. Health utility, social functioning, and peristomal skin complications. J Wound Ostomy Continence Nurs. 2021;48(2):141-146.
- Pittman J, Colwell JC, Raizman R, et al. Characteristics of the patient with an ostomy associated with leakage. J Wound Ostomy Continence Nurs. 2021;48(1):43-49.
- Taneja C, Netsch D, Rolstad BS, Inglese G, Eaves D, Oster G. Clinical and economic burden of peristomal skin complications in patients with recent ostomies. J Wound Ostomy Continence Nurs. 2020;47(2):141-149.
- Claessens I, Probert R, Tielemans C, et al. The Ostomy Life Study: the everyday challenges faced by people living with a stoma. J Wound Ostomy Continence Nurs. 2021;48(2):163-170.
- Nichols TR, Inglese GW. The burden of peristomal skin complications on quality of life. J Wound Ostomy Continence Nurs. 2020;47(5):432-438.
- Colwell JC, Beitz J. Survey of WOC nurse clinicians on stoma and peristomal complications. J Wound Ostomy Continence Nurs. 2022;49(3):251-257.
- Wound, Ostomy and Continence Nurses Society Guideline Development Task Force. WOCN Society clinical guideline: management of the adult patient with a fecal or urinary ostomy—an executive summary. J Wound Ostomy Continence Nurs. 2018;45(1):50-58.
- Gray M, Colwell JC, Doughty D, et al. Peristomal moisture-associated skin damage in adults with fecal ostomies: a comprehensive review and consensus. J Wound Ostomy Continence Nurs. 2021;48(2):101-107.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.