How Do You Select a Wound Dressing?
March 11, 2021
Introduction
Let’s face it, dressing selection can be overwhelming for clinicians because of the plethora of products that are in the wound care market space. If only there were a multifunctional smart-dressing that could be used on every wound etiology. It would make managing wounds much easier. Practical knowledge of dressing categories, functionality, appropriateness, and reimbursement is key in dressing selection.
Considerations in Wound Dressing Selection
There are various dressing categories to choose from, and clinicians should remember that although dressings are categorized, specific product features, benefits, and dressing technology may vary. Clinicians should have practical knowledge of dressing categories, wound types, and indications when deciding on the most appropriate dressing for best healing outcomes. Clinicians tend to learn the dressing’s brand name in their facility’s formulary and not know what the dressing’s function is. Wound care dressing reimbursement is driven by the Medicare guidelines payment system.
Wound care documentation should support the medical necessity for advanced wound care dressings. Supporting documentation includes wound date of onset, wound etiology, wound status, wound size, wound depth, presence of bioburden, exudate type and amount, dressing frequency, and physician wound progress notes. Clinicians should be familiar with the payment systems, which may vary by health care setting, state, and region.1 When selecting a dressing, remember to consider wound size and depth, exudate amount, dressing frequency, and any patient-related factors such as payer source and who will be changing the dressing.2
Dressings should have conformability to keep direct contact with the wound bed. Wounds located on the heel are a good example; you may need to create a heel cup or use a heel-designed dressing to avoid bulkiness. Remember always to pack dead space in wounds, but loosely. Wound cleansing during each dressing change will help decontaminate the wound, eradicate biofilm, and promote healing.3
Cleansing the wound bed surface, periwound, and surrounding skin will support good wound hygiene practices. There are various wound cleansers and solutions, but become familiar with the ingredients in products. Cleanser and solution features may include bactericidal, bacteriostatic, fungicidal, various delivery methods (spray, non-aerosol, splash guard), and specific dosing (vials, units). Consider the cleanser or solution’s mode of action paired with the type of dressing and format to avoid deactivation of certain bioactive products. Using dressings that keep the wound warm and maintain an optimal moist wound environment will prevent moisture imbalance and promote healing.
Dressings that absorb, such as foams and super absorbents, provide these functions and allow longer wear times as indicated. Some dressings contain super absorbent polymers that have a moisture transfer and wicking property to ensure periwound protection from excess moisture. Selecting the appropriate dressing size will help prevent maceration and further skin impairments.
Remember the periwound is just as important as the wound. Use liquid skin protectants or sealants and barrier cream to protect surrounding skin from moisture-associated skin damage. In wounds that are draining only a scant amount of exudate, you can stretch the dressing wear time or may need to use a dressing to donate moisture. This will help optimize a moist healing wound environment, thereby moving the wound toward a healing trajectory. Remember to keep wounds covered because research shows that wounds heal at a faster rate when the wound is covered and maintain a steady temperature.
Dressing Categories and Indications for Use
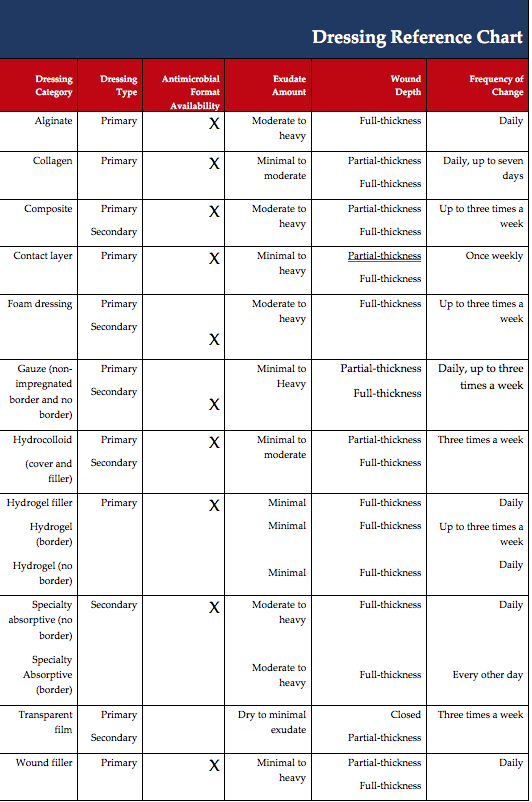
The following table is provided to help determine appropriate dressings by looking at wound depth, wound exudate, availability of an antimicrobial format, and frequency of dressing change.4
References
- Medicare & Medicaid Services. Surgical dressing services. 2020. https://www.medicare.gov/coverage/surgical-dressing-services. Accessed March 1, 2021.
- Dabiri G, Damstetter E, Phillips T. Choosing a wound dressing based on common wound characteristics. Adv Wound Care (New Rochelle). 2016;5(1):32-41. doi:10.1089/wound.2014.0586.
- Mannis D, Brandl A. Efficacy of common decontamination methods for cleaning contaminated wounds. Health Phys. 2015;108(1 Suppl 1):S5-S12. doi: 10.1097/HP.0000000000000190. PMID: 25551653.
- Noridian Healthcare Solutions. Surgical dressings. https://med.noridianmedicare.com/web/jddme/dmepos/surgical-dressings. Accessed March 1, 2021
About the Author
Cheryl Carver is an independent wound educator and consultant. Carver's experience includes over a decade of hospital wound care and hyperbaric medicine. Carver single-handedly developed a comprehensive educational training manual for onboarding physicians and is the star of disease-specific educational video sessions accessible to employee providers and colleagues. Carver educates onboarding providers, in addition to bedside nurses in the numerous nursing homes across the country. Carver serves as a wound care certification committee member for the National Alliance of Wound Care and Ostomy, and is a board member of the Undersea Hyperbaric Medical Society Mid-West Chapter.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.