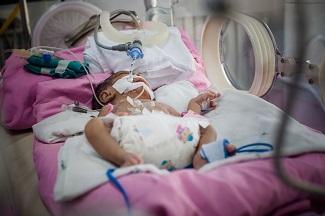
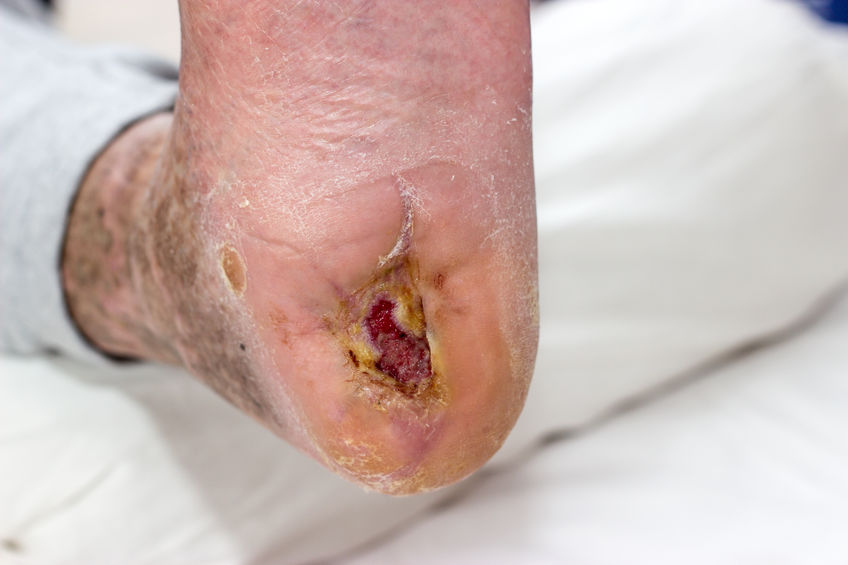
Neonatal Pressure Injury Prevention
January 16, 2020
By Ivy Razmus, RN, PhD, CWOCN
There remain many unanswered questions regarding pressure injury and prevention practices among neonatal patients. Guidelines for pressure injury prevention were initiated in 1992 by the U.S. Agency for Healthcare Research and Quality (AHRQ). Pressure injury prevention practices are based on these guidelines, which recently expanded to include pediatric patients.1-3
Neonatal Intensive Care Unit Studies
A study conducted by Fujii et al.4 included infants in incubators from seven neonatal units in Japanese hospitals. Of the 14 pressure ulcers that developed, almost half were located on the nose. A cumulative incidence of pressure injuries of 16% was described.4 The lack of research on infants and pressure injury practices restricts our application of pressure injury prevention in this patient group. Studies of neonatal intensive care unit (NICU) patients have provided data for a higher frequency of pressure injuries in neonates relative to patients in general pediatric units.5 In a multisite study of pressure injury occurrence in children from birth to 18 years of age, 24% of the pressure injuries occurred in premature infants from the NICUs in four hospitals in Germany and Switzerland, as reported by Schlüer et al.6 Level III NICUs had the lowest proportion of patients assessed for pressure ulcer risk on admission, but they had the highest proportion of patients determined to be at risk for pressure ulcers.6 Interestingly, the lowest proportion of patients determined to be at risk for pressure ulcers was in level IV NICUs.7 It is unclear what clinical factors were used in determining risk in these patients.
Recently, in a study of 11,203 at-risk pediatric patients, only 70.7% of the pediatric patients at risk for pressure ulcers received a pressure redistribution surface.7 European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel (NPIAP), and Pan Pacific Pressure Injury Alliance guidelines recommend use of a pressure redistribution surface compatible with the care setting and individual patient size and weight.3
It is not clear whether the pressure redistribution surfaces used in the NICUs were designed for pediatric or adult patients or whether pediatric redistribution surfaces were available. More information is needed to better understand the use of pressure redistribution surfaces in pediatric patients, including which type of pressure redistribution surface decreases hospital-acquired pressure injury. In the aforementioned study of pressure injury prevention in acutely ill pediatric patients, moisture was managed most often among patients in level III NICUs (88.8%), level IV NICUs (85.5%), and pediatric rehabilitation units (92.1%).7
Although the NPIAP guidelines recommend keeping the skin clean and dry while also protecting the skin from excessive moisture,8 no study has examined the use of moisture management as a pressure injury prevention intervention in unit types outside of pediatric critical care units or with a larger sample. For example, neonatal skin is still developing, and products may be absorbed through the skin; however, most products intended for moisture management have not been tested in this vulnerable population.9 More studies are needed to define the type of moisture management used to prevent pressure ulcers among neonatal at-risk patients.
Conclusion
For infants, evidence for pressure injury risk assessment, pressure redistribution surface use, and moisture management is unavailable. Based on the lack of current evidence on pressure injuries and prevention measures, there is a need for future research into pressure injury prevention practices among NICU care nurses in assessing risk, pressure redistribution surface use, and moisture management. If you would like to refer a survey to nurses involved in neonatal care, please ask them to contribute to our data by using this link: https://forms.office.com/Pages/ResponsePage.aspx?id=2MKkyGi9ukC4tnUivpp…
References
1. Agency for Healthcare Research and Quality (AHRQ). Pressure ulcer guidelines. Rockville, MD: AHRQ; 1992. https://www.ncbi.nlm.nih.gov/books/NBK63915/. Accessed December 16, 2019.
2. European Pressure Ulcer Advisory Panel (EPUAP). Pressure ulcer prevention: Quick reference guide. 2009. http://www.epuap.org/wp-content/uploads/2010/10/Quick-Reference-Guide-D… . Accessed December 16, 2019.
3. European Pressure Ulcer Advisory Panel (EPUAP). Pressure ulcers: Quick reference guide. 2014. http://www.epuap.org/wp-content/uploads/2010/10/NPUAP-EPUAP-PPPIA-Quick…. Accessed December 16, 2019.
4. Fujii K, Sugama J, Okuwa M, Sanada H, Mizokami Y. Incidence and risk factors of pressure ulcers in seven neonatal intensive care units in Japan: a multisite cohort 163 prospective study. Int Wound J. 2010;7(5):323-328. doi:10.1111/j.1742- 481X.2010.00688.xt
5. Razmus I, Berquist-Beringer S. Pressure injury prevalence and the rate of hospital-acquired pressure injury among pediatric patients in acute care. J Wound Ostomy Continence Nurs. 2017;44(2):110-117. doi: https://doi.org/10.1097/WON.0000000000000306
6. Schlüer AB, Cignacco E, Müller M, Halfens RJ. The prevalence of pressure ulcers in four paediatric institutions. J Clin Nurs. 2009;18(23):3244-3252. doi:10.1111/j.1365-2702.2009.02951.x
7. Razmus I, Berquist-Beringer S. Pressure ulcer risk and prevention practices in pediatric patients: a secondary analysis of data from the National Database of Nursing Quality Indicators®. Ostomy Wound Manage. 2017;63(2):28-32. PMID:28267681.ui
8. National Pressure Injury Advisory Panel (NPIAP). Mucosal pressure ulcers: a NPUAP position statement. 2009. https://cdn.ymaws.com/npuap.site-ym.com/resource/resmgr/position_statem…. Accessed January 16, 2020.
9. Razmus I. Pressure ulcers and prevention among pediatric patients and factors associated with their occurrence among acute care. 2015. https://kuscholarworks.ku.edu/handle/1808/23979. Accessed December 12, 2019.
About the Author
Ivy Razmus, RN, PhD, CWOCN is an Assistant Professor at the University of Detroit Mercy where she is currently teaching in the BSN Nursing program. Her research focus is on pressure injury prevention for pediatric patients including neonatal patients. She has experience as a Manager of Pediatric populations both neonatal and pediatric intensive care; as a quality analyst within a health system focusing on nursing sensitive quality indicators and root cause analysis; and as a CWOCN in the acute, critical and outpatient settings in the adult population.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.