Does Moisture-Associated Skin Damage Apply to Infants?
May 31, 2019
Moisture-associated dermatitis has been described as "inflammation and erosion of the skin due to prolonged exposure to moisture and its contents which include urine, stool, perspiration, wound exudate, mucus, or saliva."1 Incontinence dermatitis is caused by overhydration of the skin, maceration, prolonged contact with urine and feces, retained diaper soaps, and topical preparations. Indeed, diaper dermatitis has been used to describe an infant's skin breakdown related to moisture exposure.
Categories of Moisture-Associated Dermatitis in Adults
In adults, moisture-associated skin breakdown has been divided into four categories: incontinence-associated dermatitis (IAD); intertriginous dermatitis (ITD); peristomal moisture-associated dermatitis; and periwound moisture-associated dermatitis. Diaper dermatitis in infants has long been known in clinical practice. It results from long-term exposure of the skin to harmful moisture and can lead to extensive skin breakdown. The term moisture-associated skin damage, used to describe the variations of skin damage in older populations, can easily be applied to infants as well.
Application of Adult Categories to Infants
For example, ITD, also referred to as intertrigo, occurs when sweat is not able to evaporate in skin folds. This causes overhydration resulting in maceration. You may see this on infants in their neck folds where there is minimal air circulation or under their arms. Friction may also occur on both sides of the skin folds. Infants are more at risk because of sweat trapped in skin folds with minimal air circulation. When the sweat is not able to evaporate, the stratum corneum becomes overly hydrated and macerated. It is not known whether these data are collected or used for comparison in infants. In other cases, infants may also have an ostomy or opening into their skin that could result in peristomal moisture-associated dermatitis. These openings could also include a gastrostomy tube or a tracheostomy.
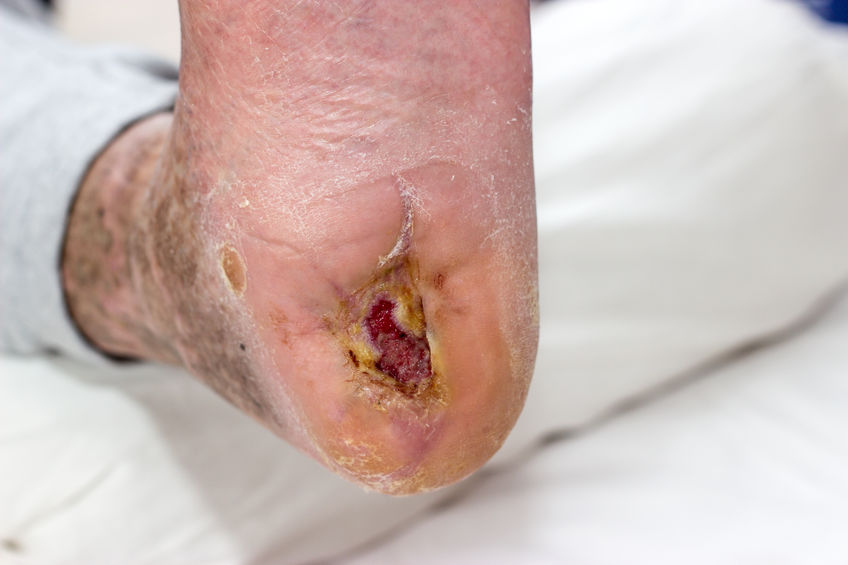
These areas could be exposed to moisture such as saliva or drainage leaking from the stoma site of urine, stool or sweat. It is important to have skin barriers appropriate for infants in use and size to protect these areas from the effluent and moisture that can lead to breakdown of the surrounding skin. There are also situations in which infants have a wound resulting from surgery or from birth. Those wounds may produce exudate, which can cause skin to become macerated and lose its integrity. This type of skin damage is called periwound moisture-associated dermatitis. Infants with abdominal wall defects or surgery for myelomeningocele are examples of situations in which wounds could produce moisture during the inflammatory stage of healing and thereafter. This could result in an inability for the wound to close in a timely way. Similarly, IAD in infants could be caused by the same organisms and conditions that are found in adults, such as Candida, seborrhea, bacteria or allergies.
Conclusion
As we develop our evidence for best practices in older populations, we should keep in mind that there is a need for evidence on effective products for moisture-associated skin breakdown in infants as well as adults, and the methods used to describe these conditions would be useful in younger populations.
References
1. Baharestani M, Black, J, Bliss D, Colwell J, Goldberg M, et al. Moisture-associated skin damage: overview and pathophysiology. J Wound Ostomy Continence Nurs. 2011 May-Jun;38(3):233-41. Accessed at https://www.ncbi.nlm.nih.gov/pubmed/21490547.
Esser M. Diaper dermatitis: what do we do next? Adv Neonatal Care. 2016;16 Suppl 5S:S21-S25. John Hopkins Medicine. Diaper dermatitis. https://www.hopkinsmedicine.org/health/conditions-and-diseases/diaper-d…. Accessed May 6, 2019.
About the Author
Ivy Razmus, RN, PhD, CWOCN is an Assistant Professor at the University of Detroit Mercy where she is currently teaching in the BSN Nursing program. Her research focus is on pressure injury prevention for pediatric patients including neonatal patients. She has experience as a Manager of Pediatric populations both neonatal and pediatric intensive care; as a quality analyst within a health system focusing on nursing sensitive quality indicators and root cause analysis; and as a CWOCN in the acute, critical and outpatient settings in the adult population.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.