Nutritional Deficiencies in a Safety Net Hospital: The Socioeconomics of Healing
January 10, 2022
Introduction
The human body possesses an amazing ability to heal itself, if given the right nutrients to carry out the necessary biologic processes involved. The need for nutritional assessment and support is critical for both acute and chronic wound healing and prevents an impaired immune defense that results in infection. Dietary intake must meet the increased demands of the body for recovery from the break in skin integrity. Nutrition in general is often overlooked when assessing healing potential in a patient's plan of care.
Safety Net Hospitals and the Socioeconomics of Wound Healing
The World Health Organization (WHO) defines malnutrition as any form of deficiency, excess, or imbalance in the intake of nutrients by an individual.1 The presence of nutrient deficiency despite normal caloric intake is quite common, specifically in low-income areas that lack access to grocery stores. These areas are defined as food deserts by the US Department of Agriculture (USDA).2
The city of Jacksonville, Florida has several neighborhoods that are designated as food deserts because they lack public transportation and grocery stores that offer fresh food.3 This nutritional compromise is associated with chronic health conditions, including hypertension, diabetes, cardiovascular disease, and delayed wound healing. The full impact of nutritional deficits on wound healing is probably still a bit of a surprise, even to seasoned wound care clinicians. In fact, I would dare to say it is eye opening and has certainly caused our multidisciplinary team to take notice! Indeed, the food desert designation was a call to action to address a serious socioeconomic disparity. The University of Florida (UF) Health System in the city of Jacksonville is a safety net hospital, meaning we serve the uninsured, underinsured, psychiatric, and forensic patient population. Our Wound Healing Clinic provides care across the continuum to help heal wounds and save limbs, or at least we thought it was a comprehensive program. It turns out we were not fully as inclusive as we thought.
A company representative contacted me about a nutritional supplement that is available in the hospital. The only drawback was that it is accessible only if the patient has insurance. I spoke with this representative and told her very candidly that I run an underserved clinic and my patients cannot obtain the supplement (although it sounds amazing). She then gave me a few samples. I knew the perfect patient who would benefit from this supplement because nothing else was helping her to heal. The following is a brief clinical vignette of her struggle with a chronic venous leg ulceration.
Case Study
Our patient is a 51-year-old woman who presented with a chronic venous leg ulceration for a 2-year period to the Wound Healing Clinic. She is unfunded and in the city contract program. During her course of treatment, she underwent the standard of care, including an antimicrobial foam dressing with consistent compression therapy. Evaluation of her venous system through ultrasound showed no evidence of deep vein thrombosis or venous reflux by vein mapping. The wound biopsy performed showed only the presence of inflammatory cells, with no malignancy noted. Serial synthetic skin grafting was attempted, with failure at each application. Laboratory evaluation of her albumin and prealbumin values showed that they were within normal limits. Her past medical history was positive for hypertension and morbid obesity, with a body mass index of 49.2. Clinical photograph from May 2021 of right leg venous ulceration (consent obtained).

Wound measurement (8.2cm x 2.0cm x 0.2cm). The patient was started on nutritional supplementation in May 2021 (additional samples were provided by the wound specialist physician, who covered the cost personally because of the unfunded status of the patient). After a 2-month period of two packets per day consumed in 8 ounces of water, wound closure was observed on July 21, 2021. Clinical photograph of healed wound (consent obtained). 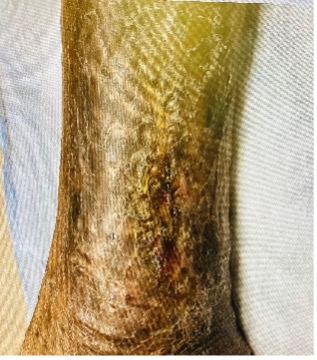
What This Patient Taught Us
This case study demonstrates that despite having enough or even excessive caloric intake, there are still major deficiencies at the micronutrient level that impede wound healing. By addressing these deficiencies with supplementation (especially zinc and vitamins C, E, and B12) and patient education, clinicians find the missing component to healing success. This patient had struggled for a while, even though her initial assessment blood work did not show any abnormal ranges. This patient’s case made us realize that we had been missing the larger picture when nutritionally assessing our wound healing patients. This patient inspired us to engage and utilize our clinical nutrition team more. Our team achieves these goals through the implementation of diverse screening tools while expanding our nutrition-focused patient education programs.
Going Forward
In an effort to make the foregoing nutritional supplement available to the unfunded patient population at UF Health, a grant application has been submitted in the hopes of covering the cost of the supplement with increased education initiatives in conjunction with community advocacy groups to better serve our patients. The opportunity to heal fully should not be dictated by the socioeconomics of your Zip Code.
References
- Barchitta M, Maugeri A, Favara G, et al. Nutrition and wound healing: an overview focusing on the beneficial effects of curcumin. Int J Mol Sci. 2019;20(5):1-14. doi:10.3390/ijms20051119
- Pike SN, Tapl ES Clark JK, et al. Examining the food retail choice context in urban food deserts, Ohio, 2015. Prev Chronic Dis. 2017;14:E90. doi:10.5888/pcd14.160408
- Phillips J. “You have to think about struggling people” food desert program to begin in NW Jacksonville.” Action News Jax, January 27, 2020. Accessed January 9, 2022. www.actionnewsjax.com/news/local/duval-county/you-have-think-about-stru…
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










