Understanding Infection: An Overview of the Mechanisms of Viral, Fungal and Parasitic Infections
February 11, 2014
By Bruce E. Ruben MD
Part 1 in a series on infection management
What is an Infection?
The world of bacteria, viruses, fungi and parasites has a long and storied place in the human condition. Way more often than not, bacteria live normally on our skin and line our entire gastrointestinal tract from mouth to anus.
Throughout our lives, viruses and parasites find homes in our nerves, brains, lungs and lymph nodes – living happily and symbiotically off of our bodies without noticeable "infection" or "disease." I like to think of our immune system as the armed forces with a separate army, navy, marines and central intelligence on call defending our health against invasion 24/7.
By way of example, one trillion fresh white blood cells or leukocytes are made daily, circulating and penetrating every tissue in our body from the far reaches of our skin to the marrow of our bones. These leukocytes are the army, our first line of defense, if one should sustain a trauma to the skin and loads of bacteria move beyond the skin's surface to below. They act like piranhas, slurping up every last germ until sterility is achieved and healing takes place. Rarely does a cut lead to aggressive fast moving infection of the skin and the soft tissues below.
However, life is not perfect and at times there are lapses in the body's immune response or delays in recognition and response to the invading microorganism. Infection or disease then becomes clinically evident to us all depending on what organ system is affected. The following two images illustrate various diseases (bacterial and viral) and the targeted organ systems affected by each type of infection:
Image 1: Bacterial Infections
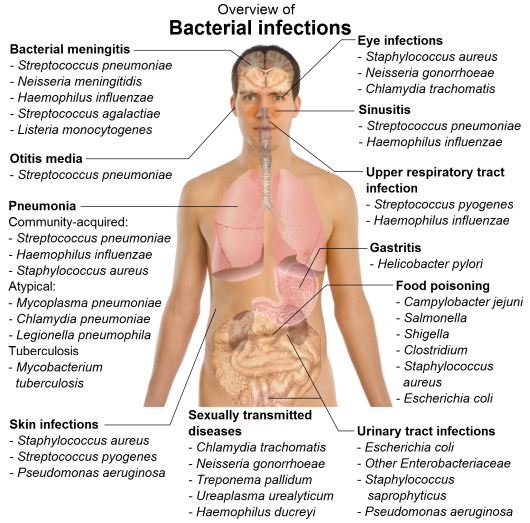
Image 2: Viral Infections
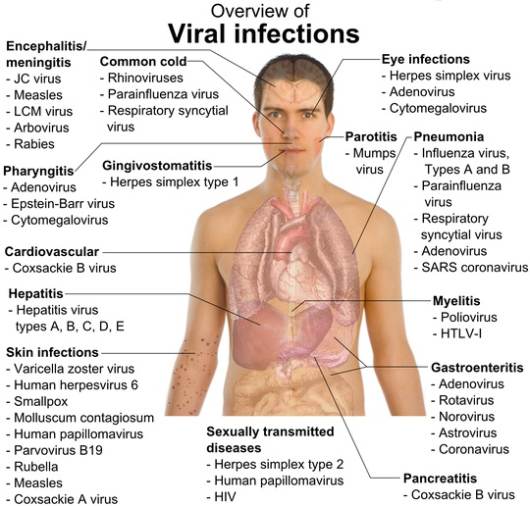 (Source: www.wikimedia.org)
(Source: www.wikimedia.org)
In all cases, the body will mount an inflammatory response and this is telling by the universal symptoms of fever, chills, fatigue and loss of appetite with specific signs based on the organ affected. For example, if it's infection in the lung, a cough will accompany these symptoms.
Lack of immune recognition of a new germ is an increasingly common cause of infection or disease, as exemplified by the constantly changing influenza virus. Still, most of us have the recognition and response capabilities to make specific proteins and toxins to vanquish a virus and return to good health.
Despite the wonderment of our divine immune system, the advent of the germ theory of disease, antimicrobial agents and vaccine prevention have had no equal in advancing mankind's longevity. Just consider that back in 1900, before penicillin, people rarely lived to have pneumonia twice.
Treatments for Infections
Today, antibiotic, antiviral, antifungal, and anti-parasitic agents are available to aid our body's response to these organisms when they are causing disease and they can often tip the scales in our health's favor. Most if not all of these agents are well tolerated. The route of antibiotic administration, oral or intravenous, is based on the drug levels needed to achieve bacterial death and does not change the frequency of adverse complications such as an allergic reaction.
It's important to remember is that these antimicrobial medicines interfere only with microbial life and don't affect human tissue, which distinguish them from cancer chemotherapy. Antibiotic resistance is attributed to microbial mutation and selection just as cancer resistance is due to human cancer cell mutation and selection. Thus, people don't become immune to antibiotics, bacteria do.
In short, infections cause disease when the body's remarkable immune system falls short. Universal symptoms include fever, chills, fatigue, and loss of appetite. Additional symptoms attributed to the organ system involved, such as diarrhea in the gastrointestinal tract, help the skilled physician locate and properly manage the disease.
About the Author
Dr. Bruce Ruben is the Founder and Medical Director of Encompass HealthCare, located in West Bloomfield, Michigan. Encompass Healthcare is an outpatient facility featuring advanced wound care, IV antibiotic therapies, hyperbaric oxygen treatment, nutritional assessment, and other treatment modalities. Dr. Ruben is board certified in Internal Medicine, Infectious Disease, and in Undersea and Hyperbaric Medicine. He is a member of the Medical and Scientific Advisory Committee and National Spinal Cord Injury Association (NSCIA) board.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of WoundSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.






