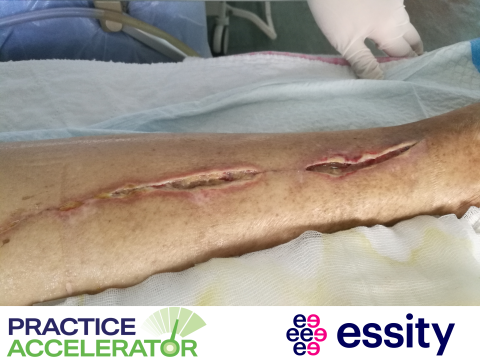
Bioburden Reduction in Surgical Wounds
September 22, 2023
In the United States alone, there are between 160,000 and 300,000 surgical site infections (SSIs) each year, representing $3.5 to $10 billion in annual health care costs.1 Reducing bioburden in surgical wounds is a critical component of preventing such infections and promoting healing. There are multiple strategies that that health care teams can employ to achieve this goal, usually aimed at reducing the levels of bacteria found in the wound and/or optimizing the host immune responses to infection.2 Surgical wounds are susceptible to bacterial contamination, which can lead to postoperative wound complications, including SSI.
Why is it Important to Reduce Bioburden in Surgical Wounds?
Bioburden refers to the number of bacteria present in a wound that can lead to infection if not managed properly.3 Proactively managing bioburden prior to the onset of infection can decrease the risk of postoperative complications, as high bacterial loads in surgical sites significantly correlate with a greater risk of postoperative complications and delayed healing.3 High bacterial loads (>105 CFU/swab) on postoperative day 2 independently increased the risk of a surgical site infection (SSI). A post hoc analysis of 58 surgical wounds found that early detection of high bacterial burden is crucial in preventing surgical site infections (SSIs).3
Does Bioburden Reduction Impact Health Care Costs?
SSIs represent $3.3 billion yearly in health care spending and contribute to more than $20,000 in costs.4 By preventing SSI and reducing risk, there is the potential to significantly reduce potential health care expenditure, and any subsequent financial burden. Additionally, avoiding unnecessary antibiotic administration has the potential to save pharmaceutical costs and prevent antimicrobial resistance. Overall, proactive management of bioburden has logical and important potential benefits not only clinically, but economically.
What Can Help Reduce Bioburden in Surgical Wounds?
Overall, early intervention before clinical infection develops and before oral or intravenous antibiotics become necessary is preferrable to manage bioburden in surgical wounds. One strategy may include wound cleansing and debridement. Techniques and agents may vary, but guidance exists that assigns different levels of cleansing intensity to the various tissue types noted upon examination of the surgical wound.5 For instance, necrotic or sloughy tissue may warrant more aggressive cleansing than healthy granulating or epithelializing tissue.5
Some approaches may even take place before the surgical incision is ever made. Recommendations ask patients to shower or bathe with soap or an antiseptic one night prior to surgery.6 Additionally, skin preparation per facility-established protocols prior to draping and beginning the procedure may aid in this effort.
Advanced therapies may also aid in prevention. Negative pressure wound therapy (NPWT) can remove excess exudate, maintain moisture balance, increase blood flow into the wound, control infection, and modulate immune responses.2 Advanced diagnostic imaging technology, such as fluorescence imaging, may also help clinicians detect and manage high bacterial loads prior to infection.3 Clinicians who are highly familiar with image interpretation have demonstrated the technology’s ability to detect elevated bacterial burden, but there is a learning curve associated with interpreting color-based images.3 However, when a positive signal appears on fluorescence images, studies note that vigorous scrubbing can often remove the signal.3 It is important for professionals to acknowledge that not all technologies will directly address surgical wound bioburden, but instead may provide benefit in early identification and monitoring.
How Much Do You Know About Surgical Wound Care? Take our quiz to find out! Click here.
Antiseptic agents like octenidine dihydrochloride (OCT), polyhexamethylene biguanide (PHMB), povidone-iodine, super-oxidized hypochlorous acid (HOCl), and sodium hypochlorite (NaOCl) are available in solution form or as functionalized dressings with microbicidal and anti-biofilm properties.2 These features may be helpful in reducing surgical wound bioburden when used in the appropriate scenarios. For instance, using stable hypochlorous acid-preserved wound cleanser as an irrigant in NPWT instead of 0.9% saline resulted in a trend towards fewer operating room visits and shorter length of hospital stay.4
In general, postoperative dressings should be kept clean and dry to avoid creating a hospitable environment for infection to develop in surgical wounds. Dressing materials should, when possible, support skin health and avoid medical adhesive-related skin injury (MARSI) that could contribute to SSI. This may include choosing skin-friendly adhesives, non-adherent materials, and using atraumatic dressing change techniques. For surgical wounds where drainage is expected, use of an appropriate drain system and/or absorbent dressing may be helpful. Specialized antimicrobial dressings are another choice clinicians may employ to reduce bioburden in surgical wounds. Specifically, these antimicrobial dressings may reduce bioburden via agents such as povidone-iodine, medical-grade honey, silver, polyhexamethylene biguanide, chlorhexidine gluconate, or dialkylcarbomoyl chloridedialkylcarbomoyl chloride.7,8
Other strategies for reducing bioburden in surgical wounds may include the use of antibiotic-coated sutures, intraoperative irrigation with or without antimicrobial solutions, and adhering to sterile surgical techniques.
Conclusion
A proactive approach to managing bacterial burden in surgical wounds may decrease the need for antibiotic usage and reduce the risk of postoperative complications. Technology may aid in early detection of high bacterial burden and allow for prompt intervention. Other peri- and postoperative strategies can also address the risk that bioburden poses, hopefully resulting in better healing outcomes and reduced health care expenditure.
Overall, reducing bioburden in surgical wounds requires a comprehensive approach that incorporates both proactive treatment strategies and advanced technologies. By reducing bacterial levels and optimizing healing processes, health care professionals can promote successful outcomes for patients undergoing surgical procedures
References
- Ban KA, Minei JP, Laronga C, et al. American College of Surgeons and Surgical Infection Society: Surgical Site Infection Guidelines, 2016 Update. J Am Coll Surg. 2017; 224(1): 59-74
- Versey Z, da Cruz Nizer WS, Russell E, et al. Biofilm-innate immune interface: contribution to chronic wound formation. Front Immunol. 2021;12:648554. doi: 10.3389/fimmu.2021.648554.
- Sandy-Hodgetts K, Andersen CA, Al-Jalodi O, et al. Uncovering the high prevalence of bacterial burden in surgical site wounds with point-of-care fluorescence imaging. Int Wound J. 2022;19(6):1438-1448. doi: 10.1111/iwj.13737. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9493216
- Gallagher KE, Alberto EC, Mallow PJ, Hermans MH, Cardenas L. A retrospective health economic analysis of a stable hypochlorous acid preserved wound cleanser versus 0.9% saline solution as instillation for negative-pressure wound therapy in severe and infected wounds. Cureus. 2022;14(4):e24321. doi: 10.7759/cureus.24321. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9123387
- National Healthcare Safety Network. Surgical site infection events module. Centers for Disease Control and Prevention; 2023. https://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf.
- Berríos-Torres SI, Umscheid CA, Bratzler DW, et al. Centers for Disease Control and Prevention Guideline for the Prevention of Surgical Site Infection, 2017. JAMA Surg. 2017;152(8):784–791. doi:10.1001/jamasurg.2017.0904
- Mana TSC, Donskey C, Carty N, et al. Preliminary analysis of the antimicrobial activity of a postoperative wound dressing containing chlorhexidine gluconate against methicillin-resistant Staphylococcus aureus in an in vivo porcine incision wound model. Am J Infect Control. 2019;47:1048-1052
- Totty JP, Bua N, Smith GE, Harwood AE, Carradice D, Wallace T, Chetter IC. Dialkylcarbamoyl chloride (DACC)-coated dressings in the management and prevention of wound infection: a systematic review. J Wound Care. 2017;26(3):107-114. doi: 10.12968/jowc.2017.26.3.107. PMID: 28277989.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.