Common Peristomal Skin Complications: How to Prevent and Manage
July 14, 2023
Introduction
Peristomal skin complications (PSCs) include inflammation, injury, or damage to the skin surrounding an abdominal stoma. PSCs are among the most common challenges faced by people living with an ostomy, with as high as 80% reported incidence.1 Complications are highest in individuals with an ileostomy.2 Some of the most common PSCs in individuals with stomas for fecal diversion include the following:
- Irritant Contact Dermatitis (PICD)
- Fungal Dermatitis
- Allergic Contact Dermatitis
- Folliculitis
- MARSI
Prevention and treatment of the above conditions are paramount for best outcomes. Knowledge and resources to prevent and manage these complications are essential for ostomates and their caregivers.
Unfortunately, many ostomates accept peristomal skin problems as a part of life with an ostomy, but this should not be the case! Healthy peristomal skin should appear like the adjacent or contralateral skin on the abdomen. Peristomal skin should be intact and free from inflammation or sensations such as pain, burning, or itching.2
How to Manage Pouching Systems
A well-fitting ostomy pouch with adequate peristomal support is the foundation for maintaining healthy peristomal skin integrity. Many peristomal complications are the result of an ill-fitting pouch, which leads to the following:
- Leakage
- Increased frequency of pouch changes
- Subsequent skin breakdown
Pouching systems should be cut to fit closely around the stoma to minimize effluent contact with peristomal skin. Convex pouching systems and ostomy belts should be considered early as valuable tools to enhance pouch security.2 Convexity is essential in providing peristomal support to individuals with flat (ie, skin-level) or recessed stomas.
How to Manage Peristomal Skin Folds
Individuals with peristomal skin folds or creases experience a higher rate of PSCs. Elevated BMI also increases PSC risk.2 Creating a flat peristomal surface on the abdomen is essential to successful pouching. This topography can be achieved with accessory products like stoma paste and barrier rings or strips to fill in skin defects or scars, in combination with an appropriate pouching system. The expected frequency of pouch changes vary widely based on the following:
- The type of ostomy
- The topography of the abdomen
- Age and activity level of the individual
- Available resources
Patients and caregivers should be taught to recognize pouch erosion (ie, visual changes in the wafer that occur when it becomes saturated). Pouch changes should occur before the wafer is compromised to maintain healthy peristomal skin.
Cleansing Peristomal Skin
Peristomal skin should be cleaned with a soft material and plain water. Use of alkaline soaps on the peristomal skin should be avoided to maintain the skin’s acidic pH and natural protective barrier.
Access to an experienced ostomy care provider and appropriate supplies can help ostomates and their caregivers arm themselves with tools to prevent and manage most PSCs.
How to Assess Peristomal Skin Complications
Many peristomal skin complications present as a reported “rash” or “skin irritation,” which can be confusing and challenging to treat without further investigation. In lighter skin tones, dermatitises often appear pink or red, while there may be varying shades of brown, pink, purple, or gray in medium to dark skin tones.
A combination of macules, papules, or pustules may be present. These visual findings may be caused by numerous factors and should be evaluated carefully to determine their cause so that appropriate treatment is initiated. Since the appearance of inflammation may vary among patients with different skin tones, other factors should be considered equally important when determining etiology of PSCs – these factors include:
- Patient history
- Pain
- Burning
- Itching
The above also includes the patient’s report of their previous experiences with skin complications and treatments.
What is Peristomal Irritant Contact Dermatitis (PICD)?
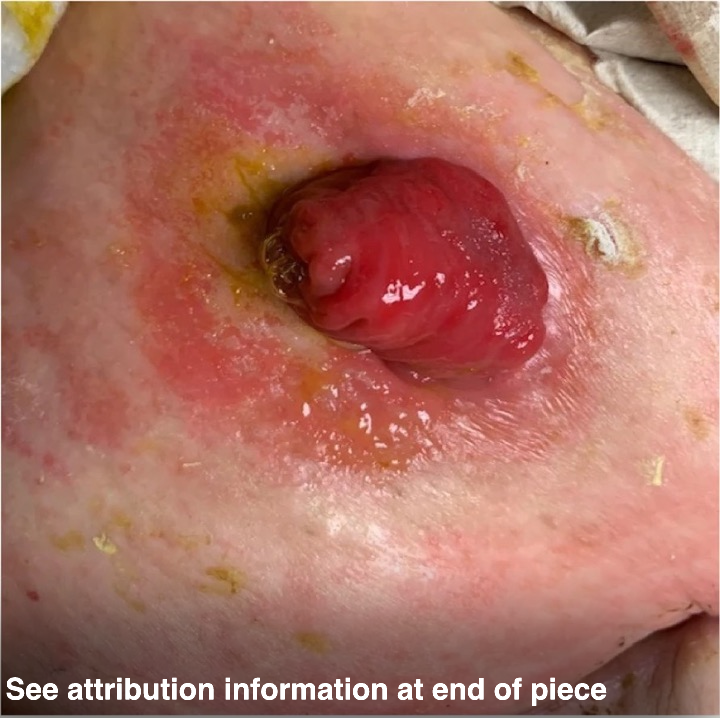 Peristomal irritant contact dermatitis (PICD), also known as peristomal moisture-associated skin damage (PMASD), is the most common PSC.2 A leaking ostomy pouch, particularly in ileostomy patients with liquid output, can rapidly lead to PICD. Leaking pouches should never be reinforced along the edges to quell leaks and delay pouch changes, as the enzymatic effluent is quite literally “digesting” the skin under the pouch. This condition often appears as skin inflammation and rash and may also show areas of skin loss. The color of PICD varies by skin tone but ranges from pink, red, and purplish to gray and dark brown. There may be scattered open wounds or bleeding. PICD is often described as painful or burning.
Peristomal irritant contact dermatitis (PICD), also known as peristomal moisture-associated skin damage (PMASD), is the most common PSC.2 A leaking ostomy pouch, particularly in ileostomy patients with liquid output, can rapidly lead to PICD. Leaking pouches should never be reinforced along the edges to quell leaks and delay pouch changes, as the enzymatic effluent is quite literally “digesting” the skin under the pouch. This condition often appears as skin inflammation and rash and may also show areas of skin loss. The color of PICD varies by skin tone but ranges from pink, red, and purplish to gray and dark brown. There may be scattered open wounds or bleeding. PICD is often described as painful or burning.
A secure pouching system is the best prevention for leakage and resultant PICD. Ensure the aperture is cut to fit closely around the stoma, and consider using stoma paste or barrier rings to seal this junction. If PICD occurs, areas of denudation may be effectively treated by "crusting" with stoma powder and a skin barrier film. Stoma powder is dusted on raw areas and then sealed with a no-sting skin barrier film. For severe or extensively denuded PICD, cyanoacrylate skin barrier film can provide a very effective treatment under a pouch.
What is Peristomal Fungal Dermatitis?
Fungal dermatitis, known as candidiasis or yeast rash, may develop on the peristomal skin due to increased skin moisture. Antibiotic therapy increases the risk of fungal dermatitis. Other areas of the body (axillae, inguinal creases) should also be assessed for fungal dermatitis. A fungal rash typically presents with individual "satellite lesions" along the edges of a more dense patch of macules, papules, and pustules. Itching and burning are commonly reported, and the skin may have weeping or exudate present. The color of fungal dermatitis may vary by skin tone, appearing pink or red in lighter skin tones and either lighter or darker than surrounding skin in dark and medium skin tones. Dark and medium skin tones may appear ashy, gray, or peeling as fungal dermatitis resolves.
The most effective treatment and prevention of peristomal fungal dermatitis is a secure pouching system that controls excess moisture on the skin. To topically treat peristomal fungal dermatitis, providers can apply antifungal powders (-azole agents) to the peristomal skin before pouching. Powder may be sealed in place with a no-sting barrier film. Systemic antifungal treatment may be necessary if fungal dermatitis is present in other body areas.
What is Peristomal Allergic Contact Dermatitis?
Peristomal allergic contact dermatitis (PACD) is a rarer skin complication and describes an inflammatory reaction to chemicals in or under the pouch wafer. PACD presents as skin inflammation, which mirrors the shape and location of the pouch wafer.
Treatment should focus on simplifying and reducing products used in pouching. Topical products used under the pouch (soaps, lotions, accessory products, etc) should be eliminated when possible. Patch testing may be necessary to determine the offending product.3
What is Peristomal Folliculitis?
Peristomal folliculitis may occur due to adhesive trauma or inflammation of hair follicles on the peristomal area. Skin bacteria may also play a role. Folliculitis is identified by the presence of pustules at the hair follicles. Peristomal hair should be shaved gently with a single-use disposable razor or clippers in the direction of hair growth. Pouches should be removed carefully, using adhesive removal agents to reduce trauma to hair follicles. Antibacterial washes have also shown to be beneficial for the prevention of peristomal folliculitis.2,3
What is Peristomal MARSI?
Repeated pouch removal, particularly in the case of frequent pouch changes, leads to the stripping of the skin layers and can result in mechanical skin damage or medical adhesive-related skin injury (MARSI). Injudicious pouch removal may cause immediate peristomal MARSI. This condition often presents as patches of skin loss, appearing moist and pink or red, which mirror the edge or shape of the pouch. These areas may be weeping or bleeding.
Prevention of peristomal MARSI is best achieved using no-sting skin barrier films applied under the pouch wafer to reduce adhesive trauma on pouch removal. Adhesive removal agents may also aid pouch removal. Pouches should be removed from the skin gently, working from the top edge downward and applying counter pressure on the peristomal skin. Treatment of peristomal MARSI is best achieved by "crusting" denuded skin with stoma powder and no-sting barrier film, as described above, or using a cyanoacrylate film to promote healing under the pouching system.
Conclusion
Individuals with ostomies are more likely to have improved recovery and enhanced quality of life when they have access to ostomy specialists and resources that can provide education and ongoing support. Online resources like psag.wocn.org provide valuable information to clinicians and consumers to help them troubleshoot issues and connect them to an ostomy specialist in their area.4
References
- LeBlanc K, Whiteley I, McNichol L, Salvadalena G, Gray M. Peristomal Medical Adhesive-Related Skin Injury: Results of an International Consensus Meeting. J Wound Ostomy Continence Nurs. 2019;46(2):125-136. doi:10.1097/WON.0000000000000513
- Ratliff CR, Goldberg M, Jaszarowski K, McNichol L, Pittman J, Gray M. Peristomal Skin Health: A WOCN Society Consensus Conference. J Wound Ostomy Continence Nurs. 48(3):p 219-231, May/June 2021. | DOI: 10.1097/WON.0000000000000758
- Colwell J, Goldberg MT, Carmel J. Fecal & Urinary Diversions: Management Principles. Place of publication: Mosby; 2004. https://shop.elsevier.com/books/fecal-and-urinary-diversions/colwell/97…
- Gray M, Colwell JC, Doughty D, et al. Peristomal Skin Assessment Guide for Clinicians. WOCN. http://psag.wocn.org/
About the Author
Elizabeth Day Dechant, BSN, RN, CWOCN, CFCN is a Certified Wound Ostomy Continence Nurse at Children’s of Alabama, where she provides wound treatment recommendations and wound management for both inpatients and outpatients with acute and chronic wounds. She provides staff education on skin and wound care, ostomy care, and pressure injury prevention. Elizabeth works diligently with the hospital’s Pressure Injury Prevention Team to track and reduce hospital-acquired pressure injuries.
Image disclosures: This image is from Stoma-related complications and emergencies and is used under Creative Commons Attribution 4.0 International License.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










