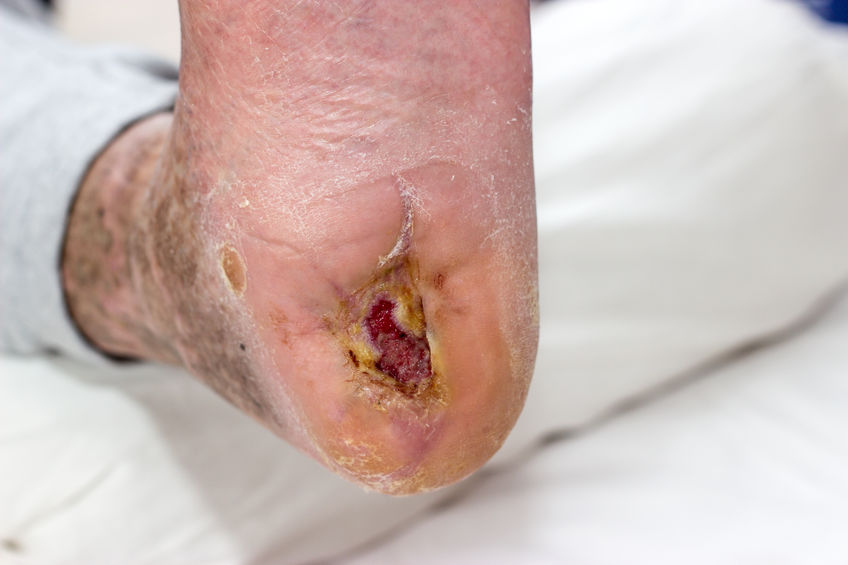
Extremes of Age and Skin Injuries
March 19, 2019
The very old and the very young are more alike than you might think when you consider risk for skin injuries. They are alike regarding their limited sensory perception, mobility, and activity. They are also alike in their potential for inadequate nutrition and their skin's supporting structures (muscle, collagen and elastin). These similarities place them at greater risk for pressure injuries.
Factors Contributing to Pressure Injury Risk
Sensory Issues
Premature infants and older adults may not be able to sense discomfort, and therefore they cannot ask for help or change their position themselves. This increases their exposure to pressure that is high or occurs over a longer period. Their limited mobility, combined with decreased activity and sensory perception, creates a risky situation without interventions to prevent prolonged pressure. The very young and the very old also may be limited in their activity levels, which decreases their ability to change their position without help or assistance.
Nutrition
The nutritional status of the very young and the very old may not be adequate because of their inability to eat, their immature or aging nutritional systems, and their dependence on others for nourishment. They may be more vulnerable to fluid and electrolyte imbalances. Premature infants may need careful management of fluids and calories and gradual introduction of oral feedings, whereas older adults may have decreased appetite for food, and if they experience alterations in activity and mobility, they may also be functionally limited in their access to food.
Properties of the Skin
In the very young and very old, the diminished amount of tissue between the skin and bone may also make the skin more at risk for decreased tolerance of pressure and shearing injury. In preterm infants, the skin is transparent, reddish, and gelatinous in appearance. The horny layer of the skin has insufficient cell layers, with two to three layers of stratum corneum at 30 weeks' gestation and virtually no stratum corneum at 23 to 24 weeks' gestation. The junction between the dermis and the epidermal basal layer is immature, with very few fibrils in the epidermal basal layer. Similarly, in very old adults, age-related skin changes induce flattening of the layers at the dermoepidermal junction, loss of tissue elasticity, and thinning of subcutaneous tissue. These issues in older adults are especially relevant given the aging of the population and the increasing numbers of persons who are more than 80 years old.
Evidence-Based Practice: Recommendations and Challenges
Evidence to support best practices in prevention and treatment of pressure injuries are emerging, and this development is encouraging. We are fortunate to have numerous professional organizations globally that are establishing guidelines and recommendations for care, but the level of evidence in premature and sick infants differs from that in the very old. It may be challenging to obtain more evidence in premature and sick infants because these patients are a vulnerable population that cannot sign a consent form, and a randomized control study may be difficult and possibly unethical to implement in one setting, thus reducing the potential for a multisite study and stronger evidence.
Conclusion
Both the very young and the very old are predisposed to skin injury because of age-related sensory perception, nutritional challenges, and characteristics of the skin at the extremes of age. Although general guidelines are available, a need exists for a stronger evidence base for prevention and treatment of age-related skin injuries, especially in premature and sick infants.
Suggested Reading
Farage MA, Miller KW, Elsner P, Maibach HI. Characteristics of aging skin. Adv Wound Care. 2013;2(1):5–10.
Roggero P, Gianni ML, Amato O, et al. Is term newborn body composition being achieved postnatally in preterm infants? Early Hum Dev. 2009;85(6):349–52.
Rutter N. The immature skin. Eur J Pediatr. 1996;155(Suppl 2):518–20.
About the Author
Ivy Razmus, RN, PhD, CWOCN is an Assistant Professor at the University of Detroit Mercy where she is currently teaching in the BSN Nursing program. Her research focus is on pressure injury prevention for pediatric patients including neonatal patients. She has experience as a Manager of Pediatric populations both neonatal and pediatric intensive care; as a quality analyst within a health system focusing on nursing sensitive quality indicators and root cause analysis; and as a CWOCN in the acute, critical and outpatient settings in the adult population.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.