Skin Conditions Frequently Found in Obese Patient Populations
August 10, 2018
By Sharon Baranoski, MSN, RN, CWCN, APN-CCNS, FAAN and Kimberly LeBlanc, PhD, RN, WOCC©, IIWCC
Overview
The Centers for Disease Control and Prevention state that in the United States, "...thirty eight percent of adults, and that seventeen percent of children and teens are obese." It is imperative that the term obesity be differentiated from overweight. Obesity refers to higher than normal body fat, whereas overweight is in reference to an individual weighing more than the standard for height and weight. Although both terms mean that a person's weight is greater than what is considered healthy for his or her height, obesity has higher negative health-related consequences.1 Health care professionals are challenged to manage increasingly complex health issues related to obesity, including complex skin conditions. The increase in stored fat associated with obesity can contribute to a variety of changes in skin physiology and is implicated in a range of dermatologic conditions.2
The skin's ability to manage transepidermal water loss is altered in the obese population. With increased fat stores the transepidermal water loss is increased, resulting in dryness and delayed skin repair. Additionally, sebaceous channels are blocked, leading to an increase in oils and resulting in acne.2 The thick layers of subcutaneous fat in obese individuals may contribute to profuse sweating (hyperhidrosis) when overheated or with activities. Hyperhidrosis can set the stage for profuse skin damage. Moisture trapped in skin folds coupled with friction as body folds rub together in combination with poorly perfused adipose tissue, insufficient oxygenation, and a compromised circulation can contribute to disruption in skin integrity and delayed healing.2
The complex skin issues and the potentially devastating consequences if an individual with obesity develops skin breakdown make it imperative that all obese individuals receive a complete and thorough skin assessment on admission to any health service. This is the first step in recognizing unusual or questionable skin conditions. A cursory assessment is not sufficient. Two or more persons may be needed to complete a good examination of all areas on the body. All skin folds and panniculus should be gently lifted and examined for erythematous, fungal, or moist denuded areas or pressure injuries. This blog addresses several of the most common types of skin injury or conditions seen in the obese population with hope of preparing clinicians to identify and prevent these skin conditions before they become complex issues.
Intertriginous Dermatitis
The most common skin condition seen is intertriginous dermatitis (ITD). It is defined as an inflammatory dermatosis of apposing skin surfaces, caused by moisture. An overly hydrated stratum corneum can result in friction damage. The moisture source is often perspiration, but it can also be urine or stool. Macerated skin can become inflamed and denuded, producing a breeding ground for microorganisms and an infection. ITD is commonly found in inframammary, axillary and inguinal skin folds and in other skin folds.3 Who is at risk for ITD? Any patient with a skin fold, hyperhidrosis, diabetes, steroid use, broad-spectrum antibiotic use, or urinary and fecal incontinence.3
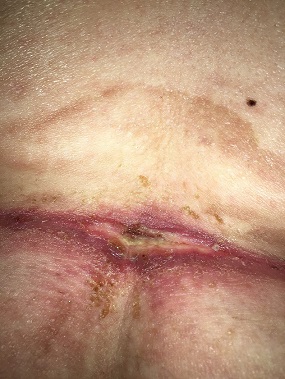
Intertriginous Dermatitis
© Kimberly LeBlanc. Used with permission.
Management Strategies: Wick moisture away from affected and at-risk skin; use soft, absorbent pads, soft linen, or high-air flow incontinence pads between skin folds to decrease moisture and friction; reduce heat and moisture in the folds; and avoid products containing chlorhexidine gluconate, alcohol, or perfume. The use of measures to ensure continued drying of the skin fold is a primary treatment strategy. Treat secondary infection with appropriate systemic and topical agents. Individuals with ITD should seek assistance from their health care professionals.
Acanthosis Nigricans
Acanthosis nigricans is one of the most common skin conditions of obesity. Acanthosis nigricans is not a disease. It is a symptom of another condition that may require medical attention. Skin patches (brown) occur when epidermal skin cells begin to reproduce rapidly. This abnormal skin cell growth is most commonly triggered by high levels of insulin in the blood.4 When you eat, your body converts carbohydrates into sugar molecules such as glucose. Some of this glucose is used for energy in your cells, and the rest is stored. The hormone insulin must allow glucose to enter cells so that the cells can use glucose for energy.4 Obese people tend to develop resistance to insulin over time. Although the pancreas is making insulin, the body cannot use it properly. This creates a buildup of glucose in the bloodstream that can result in high levels of both blood glucose and insulin in your bloodstream.4
Excess insulin causes normal skin cells to reproduce at a rapid rate. These new cells possess increased levels of melanin. This increase in melanin produces a patch of skin that is darker than the skin surrounding it. Thus, the presence of acanthosis nigricans is a strong predictor of future diabetes.4
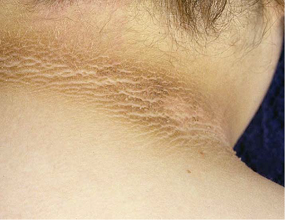
Acanthosis Nigricans
Management Strategies: If the cause of the changes in skin pigmentation is related to high blood glucose and insulin, then the issue can be controlled with proper diet, exercise, and blood glucose control. If the patient is concerned with the appearance of the affected skin, there are cosmetic treatments available. Antibacterial soaps, oral acne medications, and laser therapy are also options to lighten the skin.4
Hyperkeratosis
Hyperkeratosis results from chronic excessive pressure on or friction to the epidermis, particularly on the feet. Excessive weight on the feet leads to plantar hyperkeratosis, a thickening of the weight-bearing surfaces on the soles. It manifests with itchy, scaly patches that are bluish-purple (lichen planus); red, flat coarse skin patches (actinic keratosis); and small, harmless brown or black skin growths of unknown cause.5
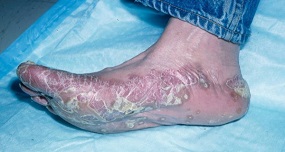
Hyperkeratosis
Photo credit: Diseasespictures.com
Management Strategies: Any treatment of hyperkeratosis normally depends on the cause, location, type, and severity. Treatment includes weight loss and orthotic shoe inserts to protect bony prominences from breakdown. Additionally, skin softening agents may help. Individuals with hyperkeratosis should seek assistance from their health care professionals for foot and nail care.
Pressure Injuries
Pressure injuries that develop in the obese population have slightly different characteristics because pressure is distributed somewhat differently. In patients of normal weight, high pressure points are seen over bony prominences. With the obese patient, a large amount of weight-induced force is distributed over the entire supine surface, as well as the bony prominence. Atypical pressure injuries may develop over the buttocks, buttock cleft, or other areas of maldistribution of weight. Bilateral hip injuries are commonly seen in patients placed in chairs that are too narrow for their size. Large, heavy calves need to be suspended off the bed, elevated on a properly sized wedge for the patient. These patients seem to be at higher risk for pressure damage related to medical devices (e.g., tubes, probes) because the devices become lodged within skin folds or under the abdominal pannus.6

Pressure Injuries
Management Strategies: The best management of pressure injuries is prevention. Many of these pressure injuries can be prevented with proper bariatric equipment or devices and frequent inspection of the skin for tissue damage. If pressure injuries do occur, it is imperative that individuals seek the assistance of a health care professional.
Erythrasma
Erythrasma is a superficial skin infection that causes brown, scaly skin patches. It is caused by Corynebacterium minutissimum, a normal part of skin flora. Not only is this an aesthetically unappealing condition, but also there is evidence to support that erythrasma can be an early sign of type 2 diabetes mellitus. Generalized erythrasma is most commonly seen in diabetes mellitus type 2, in which the lesions go beyond the areas of the body where skin is rubbing together. Erythrasma is prevalent in obese persons, in warm climates, and in people with diabetes.
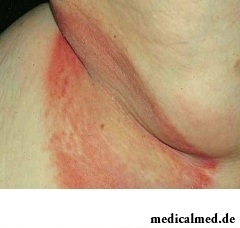
Erythrasma
Management Strategies: Treatment focuses on keeping the area clean and dry and using appropriate antibiotics. The condition is worsened by wearing occlusive clothing.4
The Need for Skin Inspection
Regardless of the skin condition, it is important that individuals with obesity perform skin self-inspection when possible and that any alterations in skin integrity are reported and discussed with their health care practitioners. Individuals need to collaborate with health care professionals to ensure that regular skin inspections are completed by their health care practitioners.
References
1. U.S. National Library of Medicine. Medline Plus. June 2017.
2. Muir M, Archer-Heese G, et al. Essentials of a bariatric patient handling program. OJIN. 2009;14(1).
3. Black J, Gray M, Bliss D, et al. J Wound Ostomy Continence Nurs. 2011;38(4):359-70.
4. Ng HY. Acanthosis nigricans in obese adolescents: prevalence, impact, and management challenges. Adolesc Health Med Ther. 2016;8:1-10.
5. Hahler B. An overview of dermatological conditions commonly associated with the patient with obesity. Ostomy Wound Manage. 2006;52(6):34-47.
6. Cai S, Rahman M, Intrator O. Obesity and pressure ulcers among nursing home residents. Med Care. 2013;51(6):478-86.
About the Authors
Sharon Baranoski, MSN, RN, CWCN, APN-CCNS, FAAN is a master's-prepared advanced practice nurse with 35 plus years of experience in skin and wound care, and nursing management. She is a certified wound care nurse, and has experience in acute care, home care, acute rehab and nursing home consultation. Ms. Baranoski, a well-known lecturer, consultant, author and educator on various nursing and wound care issues, is co-editor of the textbook Wound Care Essentials: Practice Principles. She has authored numerous book chapters and published more than 100 nursing articles.
Kimberly LeBlanc, PhD, RN, WOCC©, IIWCC is the Academic Chair of the Canadian Wound Ostomy Continence Institute and a certified Wound Ostomy and Continence (WOCC (C)) Nurse working with KDS Professional Consulting. Kimberly is an Adjunct Professor with the University of Western Ontario Masters in Wound Care Program and a visiting lecturer at the McGill University School of Nursing and University of Ottawa Faculty of Medicine. Kimberly has lectured nationally and internationally on wound and ostomy care and is considered an expert on wounds in the aging population. She has published numerous peer-reviewed articles and three book chapters. Kimberly's current area of research interest is skin health in the frail elderly.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.







