The Skinny on Cellulitis: Causes, Symptoms and Treatment of Cellulitis
February 25, 2014
Part 2 in a series on infection management
For Part 1, click here
Our skin is our largest organ and performs a myriad of functions, including pain sensation, pressure sensitivity, temperature regulation and water conservation.
The skin is also our first line of defense against our physical and microbial environment. And although sheets and sheets of bacteria live harmoniously on the skin, it is still impenetrable to even the smallest protein molecules. Note: that's great information for the next time you purchase anti-wrinkle products that claim to get below the skin.
Causes and Symptoms of Cellulitis
The most common organisms, Staphylococcus aureus and Groups A-F Streptococcus, encamp in droves on our skin. But for invasive disease such as cellulitis to occur in the skin, there must first be a breach in the skin's integrity. That's when the Staphs and Streps advance below and cellulitis develops. This knowledge makes antibiotic selection easy and responses to the antibiotics predictably good when patients seek attention early on in cases of cellulitis.
Other less common causes of penetrating events such as animal and human bite wounds, needle injections, nail punctures and blunt trauma also have well known microbiology and effective antibiotic treatment is readily available when this history is known.
The cardinal signs of inflammation, redness, heat, swelling and pain, with accompanying symptoms of fever and chills, are obvious to both patient and practitioner. Cultures are generally unnecessary since Staph and Strep are the known intruders. Nearly all cases of cellulitis can be successfully managed outside a hospital today since effective oral and intravenous antibiotics are readily available in an outpatient setting.
Still, cellulitis is exceedingly rare considering the amount of skin damaging events that occur to our skin over our lifetimes. The legs and feet are the most common areas where cellulitis occurs. When cellulitis recurs, practitioners know to look in the webs between the toes where athlete's feet (tinea pedis) creates the microscopic cuts that serve as a portal of entry for skin Staph and Strep. Simple antifungal creams break the cycle of re-infection by treating the cause of the skin disruption and healing the skin.
Cellulitis or advancing skin infections rarely occur even in open, chronic, non-healing wounds because our next line of defense, 11 trillion white blood cells made fresh daily, contain and localize microbiology to the wound's surface, thereby protecting the rest of our surrounding skin and the organs below. This level of protection is comprehensive and efficient.
Advanced Complications of Cellulitis
In the rarest of events, cellulitis may advance due to either an extraordinarily virulent organism or poor host conditions. It can destroy skin and the structures below, spilling into our blood stream (bacteremia), and threatening our lives (sepsis). In only these circumstances will hospitalization be required for intensive fluid and respiratory support, and the possible surgical excision of rapidly advancing gangrene (skin death).
Summary
In short, cellulitis is a relatively rare infectious disease caused by Staph or Strep bacteria that enter the body through a breach in the skin. Once an attack of cellulitis has been diagnosed, doctors prescribe antibiotics that target and destroy the invading bacteria. Oral antibiotics are effective in resolving the majority of cellulitis cases and when they're not, higher concentrations can be administered intravenously. Combined with excellent wound care to restore skin integrity and proper nutrition, cellulitis can resolve quickly.
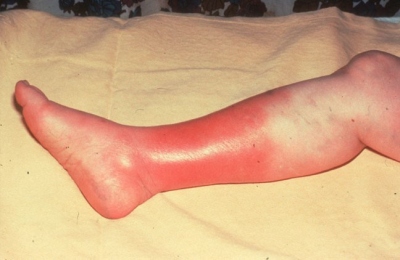
Figure 1: Cellulitis is a skin infection caused by bacteria.
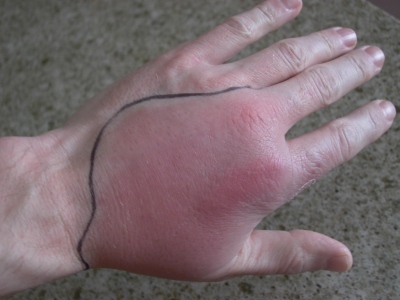
Figure 2: Doctors draw a border around the infected area to gauge whether the cellulitis is advancing or declining.
About the Author
Dr. Bruce Ruben is the Founder and Medical Director of Encompass HealthCare, located in West Bloomfield, Michigan. Encompass Healthcare is an outpatient facility featuring advanced wound care, IV antibiotic therapies, hyperbaric oxygen treatment, nutritional assessment, and other treatment modalities. Dr. Ruben is board certified in Internal Medicine, Infectious Disease, and in Undersea and Hyperbaric Medicine. He is a member of the Medical and Scientific Advisory Committee and National Spinal Cord Injury Association (NSCIA) board.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.