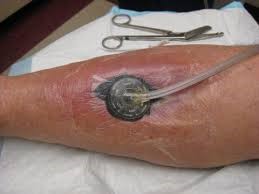
Why Protein is Important for Healing Wounds
December 2, 2015
A day doesn't go by that I'm not bombarded with information on the newest diet, the latest exercise trend or the fastest way to get in shape. My email inbox opens with message subjects like "click here to drop 10 pounds fast" or "how to get a Kardashian body without surgery." I overhear women at a local breakfast haunt order egg whites instead of whole eggs, because they contain less fat and they are worried about gaining weight. How about the latest craze of ordering sandwiches wrapped in lettuce because everyone is afraid of the dreaded carbohydrates? Our culture is so focused on losing weight, getting in shape, and looking like the latest model on the cover of Vogue or GQ that we have lost sight of what is healthy.
Yet on the other extreme, I see adults and children who are so overweight that the word "obesity" now applies to children at an alarming rate. In fact, the percentage of children aged 6-11 years in the United States who were obese increased from 7% in 1980 to nearly 18% in 2012. Similarly, the percentage of adolescents aged 12-19 years who were obese increased from 5% to nearly 21% over the same period.1 Children's clothing stores have adopted the newer label "plus sizes," replacing its predecessor "husky." Sadly, these plus sizes currently comprise 50% of store inventory.2 Medically speaking, it is a well-known fact that childhood obesity is causing type 2 diabetes.3
So we have the two extremes: the population that strives to be thin and buff and the population that overeats and overindulges. But what if I told you that many of the patients that I see in my office each day have non-healing wounds because they don't eat enough? And what if I told you that these patients don't know that they aren't eating enough to heal their wounds? (And neither do their primary care doctors!) And to complicate matters further, what if you knew that the breakdown of protein, carbohydrates and fat must be in certain proportions in order to get their non-healing wound to heal, despite other medical treatments that they may need…even if they are consuming upwards of 4,000 calories per day from foods like donuts, cookies, and cake?
Supporting Wound Healing Through Nutrition
It is important to understand that proteins are the building blocks for your body while carbohydrates and fats are primarily used for energy. Think of it like this: the protein is the framing structure, just like wood is the framing structure for a house. Your body is supported by the underlying wood framing, (i.e. the protein.) A diet with too many carbs and fats and not enough protein is like a house with really fancy bricks overlaying a straw foundation. (Think about "The Three Little Pigs.")

Carbohydrates and fats, however, are very important because they are used for energy. They support the energy requirement for protein to do its job in total, the work of living. In fact all three make up the nutritional profile needed for healthy living. The recommended diet ratio for an otherwise healthy person is 20% protein, 55% carbohydrates, and 25% fat. The general rule of thumb here is to consume approximately .5 grams of protein per 1 kg of weight. So someone who weighs 45 kg (or 99 pounds) needs about 23 grams of protein per day which equates to roughly 3-4 ounces, the size of a small chicken breast. However, when someone has a non-healing wound like a pressure ulcer, that person needs to eat three times the amount of protein in order to keep up with the body's demands.
In this example, the body is in a constant state of effort in trying to heal the wound, even though it's not visible from the outside. It's as if your body is running a race, all day long, trying so hard to recruit all of the necessary biochemical protein-based processes such as collagen formation, oxygen delivery, etc., that are needed in order to heal the wound. Without enough protein, the body gets "confused" and chooses, instead, to break down nutritional protein first, and then the body's structural protein (i.e. muscle) to meet the energy demands to preserve the most vital organs for life which are the heart and the brain. Patients in these states are considered "protein energy malnourished" and are in a catabolic state: their protein is used for energy vs. the normal anabolic state where protein is used for structure and function.
Protein Intake and the Nutritional Status of Patients with Wounds
Without this knowledge, patients with serious wounds continue their ordinary, every day eating habits, never stopping to think about their diet because this critical information may be widely ignored by medical doctors at large. In fact, most people who start down the wound healing path first see their primary physician. Often, they are not assessed properly for their nutritional status because, for example, they may look overweight. Unless they are nutritionally assessed with either an indirect calorimeter or through a carefully calculated process, there is really no way of knowing if their nutrition is supporting the wound healing process. So an obese patient with a non-healing wound who isn't eating enough protein unknowingly starts using protein for energy instead of carbs and fat. He might look well-nourished from the outside, but that person's wound will never heal due to his ongoing catabolic state.
Furthermore, additional nutrition is needed in patients with other comorbidities such as bone infections, and/or increased activity level, sometimes exceeding what most people can eat. In these instances, a feeding tube might be necessary for nutritional support, usually administered at bedtime. One thing is clear: nutrition is an often-missed piece of the wound-healing puzzle and no number of wound healing techniques such as hyperbaric oxygen therapy, IV antibiotics, vascular corrections for venous insufficiency, or even offloading will help that patient heal his wound until his body is working and functioning correctly. To go back to the house metaphor, adequate wood has to be readily available to frame a strongly grounded house. So, it's important to know the role that protein plays in wound healing for populations of patients who suffer from pressure ulcers and other non-healing wounds and it's equally important to seek out a professional wound medicine physician if all other efforts are failing.
Last, adequate hydration is as critical to life itself as it is to wound healing. Your body contains 60-70% water by weight, more water than any other component. Regulating body temperature, transporting nutrients, and waste removal are just a few of water's critical functions. The work of healing also consumes additional water beyond water loss in breath, sweat, urination and defecation. No less than 2.5-3.5 liters per day are recommended in healthy circumstances but that may need to be doubled in a serious wound healing situation. The lesson here is clear: once we all challenge the social pressure of looking like Twiggy or bravely delve into our probable, underlying, psychological reasons for overeating, what's left is basic nutrition: nutrition that applies to healthy individuals and nutrition that is specialized for patients with non-healing wounds.
References
1. http://www.cdc.gov/healthyschools/obesity/facts.htm
2. http://www.babble.com/mom/plus-sized-clothing-for-toddlers/
3. http://www.nytimes.com/2012/04/30/health/research/obesity-and-type-2-di…
About the Author
Dr. Bruce Ruben is the Founder and Medical Director of Encompass HealthCare and Wound Medicine, located in West Bloomfield, Michigan. Encompass Healthcare is an outpatient facility featuring advanced wound care, IV antibiotic therapies, hyperbaric oxygen treatment, nutritional assessment, and other treatment modalities. Dr. Ruben is board certified in Internal Medicine, Infectious Disease, and in Undersea and Hyperbaric Medicine. He is a member of the Medical and Scientific Advisory Committee and National Spinal Cord Injury Association (NSCIA) board, an advisory board member of WoundSource, and serves on the board of The Emily Stillman Foundation.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.