Wound Healing in Immunocompromised Patients
February 28, 2022
Introduction
Patients who are immunocompromised present a unique and difficult challenge when considering wound care and healing. These patients may include children, older adults, organ transplant recipients, patients with cancer,1 those with diabetes mellitus, or those with HIV/AIDS.2 Immunocompromised patients are at increased risk of hypothermia,1 infection,3 and otherwise poorly healing or recurrent wounds.4 Many treatments for infection and interventions to promote wound healing rely on a properly functioning immune system.2 In immunocompromised patients, alternate treatment methods are needed to compensate for the impairments in their natural immune response.
Challenges of Wound Healing in Immunocompromised Patients
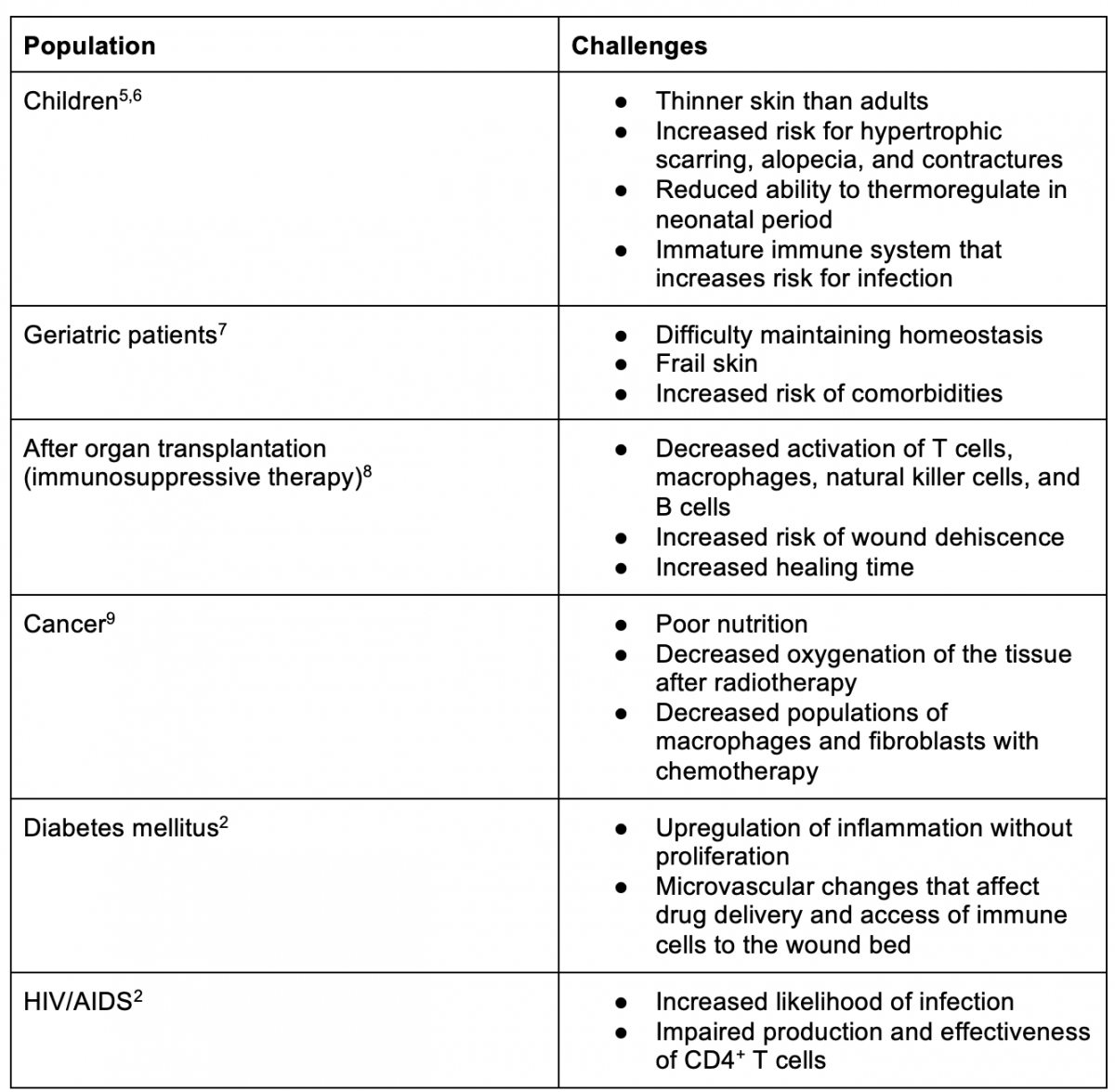
A healthy immune system consists of the innate and adaptive immune systems, each employing different cell types. The innate immune system includes neutrophils, macrophages, dendritic cells, complement proteins, and natural killer cells. The adaptive immune system includes B and T cells.2 Typical immune responses activate complex systems that can be compromised at various levels. Depending on the reason a patient is considered immunocompromised, the treatment intervention may need to be adjusted. Table 1 reviews the considerations that need to be made for wound care in various immunocompromised patient populations. However, the challenge is the same: typical wound care strategies are not necessarily effective in immunocompromised patients.
Table 1. Challenges Presented by Specific Immunocompromised Patient Populations
Specifically during the COVID-19 pandemic, immunocompromised patients have had increasingly poor wound healing outcomes. The pandemic has led to decreased access to primary and preventative care services. This change, in turn, has led to more severe infections, more hospitalizations, and more amputations, especially among diabetic patients.10 Therefore, novel approaches are needed for addressing wound care in immunocompromised patients.
Use of Advanced Technologies to Overcome Healing Obstacles
There is a growing base of novel approaches to and technologies for wound care. Choosing the right combination can help overcome the barriers to wound healing in immunocompromised patients. The following subsections describe some examples of advances in technique and technology that may positively impact wound healing in these patients.
Advanced Dressings
Advanced dressings contain a combination of materials that can target all phases of the healing process.11 In immunosuppressed patients, the wound bed may be at different phases of wound healing simultaneously as a result of microvascular issues, and the skin may be fragile. Advanced dressings can address both of these issues by impacting the wound at all levels of the healing process while also reducing the need for frequent dressing changes.
Allografts
Immunosuppressants are often used with patients after skin grafting for large or deep wounds with poor closure. The literature indicates that this approach may also be used with immunosuppressed patients who have severe wounds. The immunosuppression increases the likelihood of tissue acceptance, and the skin graft can help in wound closure, reduce the risk of infection, and decrease healing time.12
Scaffolds
Scaffolds are three-dimensional structures designed to be placed over or into a wound for support and structure. Scaffolds provide the following benefits:
- They retain and attract cells or biomaterials needed for wound healing.
- They facilitate cell interaction and migration.
- They stimulate cells to elicit improved immune and wound healing response.
- They mimic the extracellular matrix environment.
In immunocompromised patients, scaffolds can provide nutrients, cellular stimulation, and cellular migration, actions that are lacking when the immune response is suppressed or impaired.13
Stem Cell Therapy
Stem cell therapy is an emerging technology within wound care practices. It has been shown to improve both the quality and the rate of wound healing.14 However, more research is needed before stem cell therapy can be a viable option in clinical wound care patients. This therapy is currently limited to clinical trials.
Conclusions
Immunocompromised patients have unique wound care needs that cannot always be addressed with standard practices. These patients are at higher risk of complications and poor wound healing. Therefore, clinicians must take each patient’s particular situation into consideration and determine which advanced technologies would best overcome these obstacles. Especially during the current pandemic, patients who are immunocompromised need increased attention to prevent hospitalization, amputation, or severe infection.
References
- Neil JA. Perioperative care of the immunocompromised patient. AORN J. 2007;85(3):544-564. doi:10.1016/S0001-2092(07)60126-4
- Tatara AM, Kontoyiannis DP, Mikos AG. Drug delivery and tissue engineering to promote wound healing in the immunocompromised host: current challenges and future directions. Adv Drug Deliv Rev. 2018;129:319-329. doi:http://dx.doi.org/10.1016/j.addr.2017.12.001
- Schmidt G, Piponov H, Chuang D, Gonzalez M. Hand infections in the immunocompromised patient: an update. J Hand Surg. 2019;44(2):144-149.
- Lee LD, Stroux A, Nickisch D, Wröbel L, et al. Operative outcome of hernia repair with synthetic mesh in immunocompromised patients. ANZ J Surg. 2020;90(11):2248-2253.
- Sanchez J, Antonicelli F, Tuton D, Mazouz Dorval S, François C. Particularités de la cicatrisation de l’enfant [Specificities in children wound healing]. Ann Chir Plast Esthet. 2016;61(5):341-347. doi:10.1016/j.anplas.2016.05.001
- Patel S, Tomic-Canic M. Neonatal debridement: tricks or treats. J Wound Technol. 2014;1(23):12-13.
- Upton L. What is the effect of age on wound healing in the acute trauma setting?: A scoping review. Wound Pract Res. 2020;28(3):115-126. Accessed January 31, 2022. https://search.informit.org/doi/10.3316/informit.401335586556822
- Bootun R. Effects of immunosuppressive therapy on wound healing. Int Wound J. 2013;10 98-104. doi:10.1111/j.1742-481X.2012.00950.x
- Payne WG, Naidu DK, Wheeler CK, et al. Wound healing in patients with cancer. Eplasty. 2008;8:e9.
- Casciato DJ, Yancovitz S, Thompson J, et al. Diabetes-related major and minor amputation risk increased during the COVID-19 pandemic. J Am Podiatr Med Assoc. 2020;3:20-224. doi:10.7547/20-224
- Tottoli EM, Dorati R, Genta I, Chiesa E, Pisani S, Conti B. Skin wound healing process and new emerging technologies for skin wound care and regeneration. Pharmaceutics. 2020;12(8):735.doi:10.3390/pharmaceutics12080735
- Chang CK, Bartkova J, Liao YS, Tzeng YS. Successful treatment of lower limb burn wounds with long-term survived human skin allograft in an immunosuppressed patient: a case report. Int J Low Extrem Wounds. 2021;20(2):167-171. doi:10.1177/1534734620904566
- Negut I, Dorcioman G, Grumezescu V. Scaffolds for wound healing applications. Polymers (Basel). 2020;12(9):2010. doi:10.3390/polym12092010
- Nourian Dehkordi A, Mirahmadi Babaheydari F, Chehelgerdi M, et al. Skin tissue engineering: wound healing based on stem-cell-based therapeutic strategies. Stem Cell Res Ther. 2019;10(1):111. doi:10.1186/s13287-019-1212-2
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










