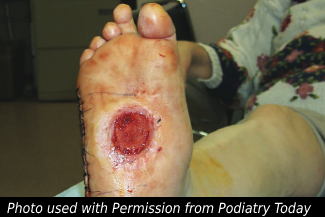
Wounds Secondary to Sleeping Position Part 1: Recognizing Pressure Injuries Secondary to Sleeping Position
June 13, 2022
Introduction: Do You Know Whether Sleeping Position Is Affecting Your Patient’s Ability to Heal?
Heel pressure injuries and various forms of ulcers are easy to identify, but are you overlooking sleeping position as a cause for wounds in other locations? Do you have a wound you are sure is venous but has normal venous insufficiency testing results and fails to respond to compression? Can pressure while sleeping slow or stop healing in your patients with venous and arterial wounds? Do you ask patients about their sleeping position in your history taking and physical examination? After reading this article, you will be able to ask patients about their sleeping habits and heal more wounds with that knowledge.
The Burden of Pressure Injuries on Patients and Health Care Professionals
Older adult patients who are confined to their bed may develop complications such as pressure injuries (previously referred to as pressure sores or decubitus ulcers) as a result of decreased mobility and increased pressure of the lower limbs. These pressure injuries may be present most often at the site of bony structures of the lower extremity, including but not confined to the heel, lateral malleolus, and medial malleolus. These ulcerations are a burden not only to the patient, but to our hospital system as well. Previous studies have noted mortality rates as high as 60% for older adults with pressure injuries within 1 year of hospital discharge.1 A retrospective chart analysis of stage 4 pressure injuries showed that the overall hospital treatment cost for hospital-acquired pressure injuries during a single admission was $129,248, and it was $124,327 for community-acquired pressure injuries over an average of 4 admissions.2 Another study showed that 83% of patients in the hospital setting with pressure injuries developed these lesions within 5 days of hospitalization.3 Pressure injuries are related to increased pressure over time. With continued education and a holistic team approach, the risk of developing these complications can be minimized.
Etiology: Why Pressure Injuries (Previously Known as Bed Sores, Pressure Sores, Decubitus Ulcers, etc) Develop
Factors contributing to pressure injuries may be classified as direct and indirect causes. Direct causes include pressure, shear, friction, immobility, loss of sensation, and combined disease.4 Indirect causes include mobility problems, poor nutrition, health conditions, aging skin, incontinence, and mental health conditions.4 The common pathway to the development of pressure injuries is tissue ischemia. Tissues are able to sustain a pressure of 30 to 32 mm Hg for only a short time. When pressure increases above this capillary fill time, it causes microcirculatory occlusion.4 This then initiates ischemia, tissue death, and ulceration.4 Lymphatic flow is also obstructed, causing metabolic waste products, proteins, and enzymes in the tissue and leading to further tissue damage from the compounding products.4
Differentiating Ulcers
Do You Know the Differences Among Venous, Arterial, and Neuropathic Ulcers?
There are 4 main types of ulcerations: venous, arterial, neuropathic, and pressure ulceration. It is important to identify the underlying etiology because each type of ulceration requires a different management approach. The key to effective management is a thorough assessment of the patient and the wound. In our experience, recognizing patterns plays a key role but usually comes only with experience.
How to Identify Venous Ulcers
Venous ulcerations are typically found at the “gaiter” region, which is located from the midcalf to the ankle. Patients with venous ulcerations typically report aching and pain at the end of the day. The pain may be alleviated with elevation. Venous leg ulcers typically have an irregular shape and well-defined borders.5 In addition, venous disease such as varicose veins, edema, and venous dermatitis may be present.5 Other signs of venous disease include telangiectasias, corona phlebectatica, atrophie blanche, lipodermatosclerosis, and inverted champagne-bottle deformity.5
How to Identify Arterial Ulcers
Often arterial ulcers as associated with pain with exercise, at night, or at rest. 6 Arterial ulcers can occur almost anywhere in the leg but typically distally on the toes and on pressure injuries such as the heels, malleolus, and shins. Arterial ulcers are usually painful; the pain is often relieved by placing the leg in a dependent position and is aggravated with elevation.6 The wounds margins are even, sharply demarcated, and punched out.6 The wound beds are commonly accompanied by necrosis and exposed tendons.6
How to Identify Neuropathic Ulcers
Unlike other ulcerations, neuropathic ulcerations are painless. They vary in size and location. They can occur over pressure points of the foot and heel. Neuropathic ulcers have a punched-out appearance and an overlying callus typically. Claw toes, Charcot neuroarthropathy, and dry and scaly feet may be associated with these ulcers.
Wounds Secondary to Sleep Position
Working through the differential diagnosis of an ulcer can be a swift process or may take weeks to months. A typical medial ankle wound may undergo venous and arterial insufficiency testing. When results are abnormal, we can easily classify the wound as venous, arterial, or of mixed etiology. When results of these studies are normal, we often blame the ultrasound technician for missing the disease or refer to ankle-brachial index scores as a screening tool and order more invasive magnetic resonance angiography or computed tomography angiography. In some cases, however, these patients may have no treatable venous or arterial disease. Instead, they may have skin cancer or excess pressure to the area leading to the wound.
Why Clinicians Should Ask About Patients’ Sleeping Habits
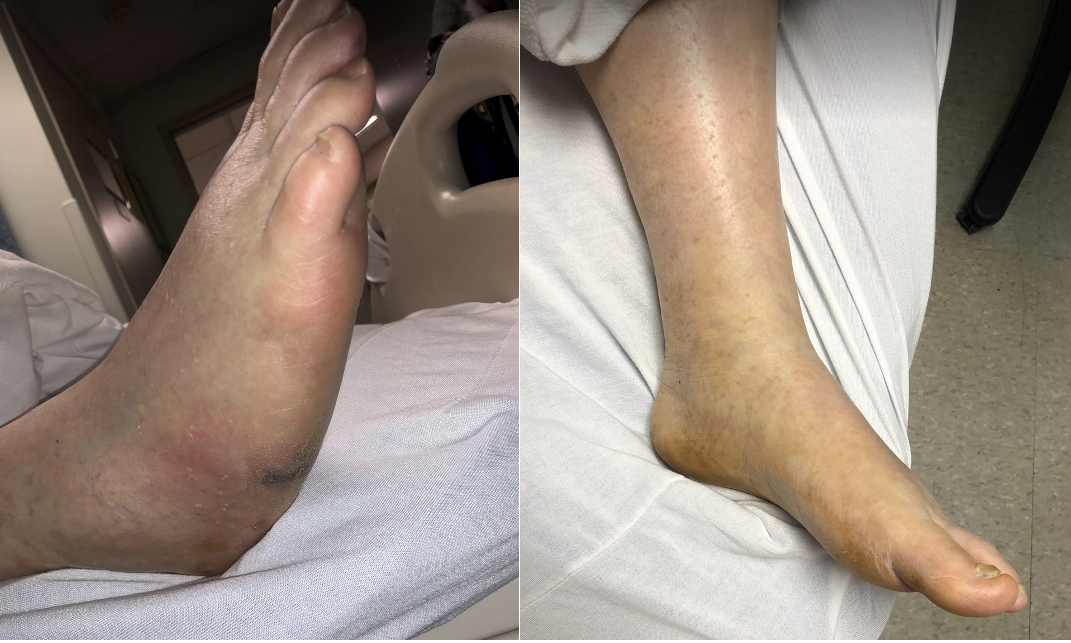
We ask every patient about their sleeping habits. We often ask, “Do you sleep in a bed or a chair?” Sleeping in a chair leads to more leg edema, even when patients are adamant that their chair elevates their legs. Chairs will impose abnormal pressure on certain regions of the lower extremity such as the posterior calf as the leg rests against the footrest. Sleeping on your left side may overload the left lateral fibula, left fifth metatarsal base (Figure 1), right medial malleolus, and right first metatarsal head. A bed that elevates the legs may lead to increased pressure at the posterior Achilles and posterior calf. Amputations alter this pattern further. One recent patient had a left above-knee amputation, slept on his left side, and developed a wound over his right medial tibial shaft. These puzzles must be decoded by identifying the wound location and the patient’s specific sleeping habits.
Connecting Pressure Injury Development to Mattress Quality
To our knowledge, no studies have evaluated pressure injuries developed in the home and have related these injuries to mattress age or type. Does a 15-year-old stiff mattress cause more pressure injuries over the lateral fibula than a newer, softer mattress? Should patients with lower extremity ulcers buy softer mattresses or pressure-reducing mattresses? Should insurance cover alternating-air mattresses, which inflate and deflate regularly to redistribute pressure, for patients at home with lower extremity pressure injuries?
How to Evaluate a Medical Mattress’ Lifespan
Most hospital mattresses are expected to last between 7 and 10 years. However, many factors may influence the mattress lifespan. Factors may include the material used in the construction of the mattress, the mattress’s original quality, the mattress type, the sleep position and body weight of the individual, and the care routine. There should be a system in place for inspecting and replacing support surfaces to assess the functional lifespan of hospital mattresses. Indicators of an expired mattress lifespan include the following: reduced height or thickness; discoloration; altered integrity of cover seams, zippers, or backing; degradation of internal components; or the presence of odor.7
In addition, following the manufacturer’s instructions should be considered. In our practice, specifically when treating patients in the hospital setting, we have noticed the lack of recognition of pressure wounds secondary to sleep position. We believe that a key to identifying these pressure wounds is through detailed assessment of the patient and the wound. Venous, arterial, and neuropathic wounds can be first ruled out through a detailed history, examination, and advanced testing. Pattern identification is another key in recognizing wounds secondary to sleep position.
Often patients with these types of pressure wounds have opposing malleoli wounds. For example, the patient may have a lateral malleolus wound on one leg and a medial malleolus wound on the opposing leg. This could simply reflect the way the patient’s leg is positioned during sleep. In addition, in our practice we have also seen lateral malleoli wounds coupled with fifth metatarsal head wounds and medial malleoli wounds coupled with metatarsal head wounds in these pressure wounds. Posterior calf wounds may also result from sleep position.
Conclusion
Pressure injuries pose a large burden on the health care community, a burden compounded by identification complications. Determining whether an ulcer is venous, arterial, neuropathic, or pressure related can impact a wound’s trajectory on the healing cascade if the lesion is identified incorrectly because each type of ulcer requires different treatment methods. Asking about a patient’s sleeping habits can help properly identify whether a wound is caused by pressure. Sleeping position and the quality and nature of sleeping surfaces can illuminate the cause of injury. In Part 2 of this blog, discover in depth how mattresses and other offloading surfaces aid in pressure injury prevention.
References
- Hughes RG, ed. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Agency for Healthcare Research and Quality; 2008.
- Brem H, Maggi J, Nierman D, et al. High cost of stage IV pressure ulcers. Am J Surg. 2010;200(4):473-477.
- Bansal C, Scott R, Stewart D, Cockerell CJ. Decubitus ulcers: a review of the literature. Int J Dermatol. 2005;44(10):805-810.
- Bhattacharya S, Mishra RK. Pressure ulcers: current understanding and newer modalities of treatment. Indian J Plast Surg. 2015;48(1):4-16.
- Bonkemeyer Millan S, Gan R, Townsend PE. Venous ulcers: diagnosis and treatment. Am Fam Physician. 2019;100(5):298-305.
- Arterial vs venous ulcers: diagnosis and treatment. Adv Skin Wound Care. 2001;14(3):146-147.
- Mata L, Dissanaike S. Acute and Chronic Wounds: Current Management Concepts. 5th ed. Mosby; 2015:15.
About the Authors
Dr. Lenz is a Certified Wound Specialist Physician. He has a special interest in limb salvage and wound care including surgery to correct deformities causing lower extremity ulcerations. He uses the most technologically advanced wound healing treatments available. He has presented multiple research projects related to advanced wound care at national surgical conferences. He is a graduate of the New York College of Podiatric Medicine and completed a comprehensive medical and surgical residency at the Jesse Brown Veterans Affairs Medical Center in Chicago, Illinois, where he served as Chief Resident. Dr. Lenz completed advanced surgical training in Germany and England, where he worked with international experts in diabetic foot surgery. He is dual board certified by the American Board of Wound Management and the American Board of Podiatric Medicine. He is a member of the American Podiatric Medical Association (APMA). Dr. Lenz is certified in hyperbaric medicine by the Undersea and Hyperbaric Medical Society. Dr. Lenz is certified in foot surgery by the American Board of Foot and Ankle Surgery.
Dr. Hussain is a foot and ankle surgery resident at RWJBH-Community Medical Center in Toms River, New Jersey. Fahad received his bachelor’s degree in biology from The University of Houston, and his medical degree from Temple University School of Podiatric Medicine. Dr. Hussain is surgically inclined and has a devoted interest in reconstructive surgery, limb salvage, cosmetic surgery, trauma, and minimally invasive surgery.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.