Acute Surgical Wounds Part I: Who's Managing the Wound?
December 13, 2018
Welcome to the first in a series of blogs focusing on acute surgical wound management. Future segments will discuss steps toward developing an acute surgical wound service (ASWS) and tips reflective of successful healing strategies. Acute wounds, the majority of wounds, are often consequences of trauma or surgery that, if not meticulously managed, can profoundly affect the patients' morbidity. Health care providers extend ample effort toward optimizing concomitant outcomes and preventing deleterious evolution that could involve loss of limbs, sepsis, and chronic wounds. However, the magnitude of wound care significantly affects every health care facility in the world. Operationally, it can be challenging to engage a consistent, coordinated care team that is proficient in advanced wound care, has familiarity with the affected patients and families, and has availability to participate in their longitudinal care throughout the healing continuum: inpatient → intraoperative → outpatient → healed.
Acute Surgical Wound Service
To provide a patient-centric comprehensive approach to care coordination, Christiana Care Health System, a 1,000-bed Level I Trauma Center in Wilmington, Delaware, developed an ASWS in 2010. This is not the first service of its kind, but its success is worthy of sharing. A specialized team consists of Board of Surgery–certified acute care/trauma surgeons and a wound care–certified nurse practitioner who are committed to management of wounds meeting any of the following criteria: result of a traumatic injury; infection; complex open surgical site; requiring multiple surgical interventions; potential for loss of limb(s); high resource case. Priorities to encourage wound healing include: most effective therapies; communication among all service providers, patients, and families; coordination of safe discharge; and close follow-up.
A recent international evidence-based prevention and treatment guideline identified multidisciplinary wound care teams of clinicians who provide consistent management as being instrumental in improving the level of quality of care and outcomes.1 Additionally, current internal and external forces in conjunction with incentives to reduce lengths of stay and readmissions align with objectives of providing an advanced wound care–focused multidisciplinary team for these complex patients.
Such a dedicated team can further alleviate the worries of patients and their families over path forward ideas, exorbitant hospitalization costs, and thoughts of potential deficits that can be overwhelming. The wound care providers' close observation can afford more opportunities for early detection of factors that often impede wound healing (i.e., infection, necrosis, malnutrition, medications, tobacco use, comorbidities, and loss of moist wound environment), thereby subsequently avoiding deterioration.
The patient-provider relationship that develops can significantly reduce anxiety in all aspects of the necessary care. Ultimately, successful outcomes are gratifying to all those involved, and feedback to team members promotes enthusiasm and further engagement in innovative wound care. Without this service, trauma patients have reported having as many as 17 different business cards of various providers attempting to manage their complex care. These providers have rotating schedules, so patients and their families are unlikely to have consistency from week to week, sometimes day to day, during their hospital stay. Their health care professionals are also not necessarily proficient in advanced wound care, and this issue contributes to variability of assessments and treatments. These patients may also have other critical diagnoses that necessitate prioritization (i.e., heart, brain, lung functionality). Days, possibly weeks, pass, and the question must be posed, "Who's managing the wound?"
Optimizing Wound Healing
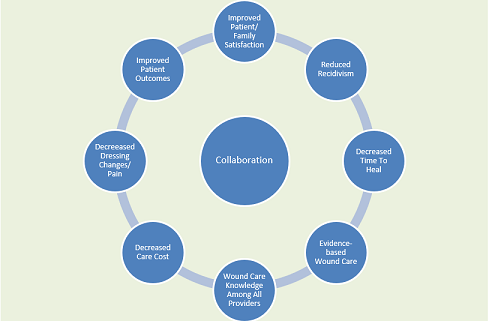
This dedicated management, like our ASWS, commences with the admission of the patient, assists in the operating room, follows during the inpatient stay, and continues in post-discharge settings until the wound is healed. This service leads the development of a patient-centric cohesive plan involving coordination of care among all the adjunct health care team members to optimize wound healing potential by utilizing evidence-based standards in a collaborative effort that ultimately reduces health care costs, alleviates lengthy hospital stays, reduces trips to the operating room, and avoids readmissions. Communication, adherence to evidence-based standards, and consistency are integral to the overall success. From our experience, the establishment of such a team has prompted:
- Collaboration of all health care providers and family
- Innovative, evidence-based wound care
- Improved wound documentation
- Decreased pain associated with dressing changes
- Increased participation in research toward improved wound care
- Post-discharge home monitoring via computerized software
- Facility-wide education encouraging vested interest in surgical outcomes and value
- Frequent post-discharge office visits ensuring durability of care
- Establishment of relationships with home health care/extended care facilities to reduce variability and keep abreast of new developments
- Decreased readmissions/length of stay/operating room trips, thereby decreasing care costs
- Hospital-specific wound care resource website
- Finally, the commitment of a comprehensive wound management team combined with efforts of ancillary health care providers and diligence of patients and families leading to successful accelerated wound healing
Wound care challenges are compounded by emphasis on outcome measures such as decreased lengths of stay and avoidance of readmissions. Meanwhile, patients are overwhelmed by the sometimes confusing plans of care, hospitalization costs, and potential residual deficits. This paradigm warrants creative, bold efforts to maximize best practice health care. Next steps for ASWS:
- More wound-certified practitioners to complement the specialized service
- Earlier notification of acute wounds, on arrival to emergency department
Next blog topic: Steps toward creating an ASWS
Reference
1. Zakhary SA, Davey C, Bari R, et al. The development and content validation of a multidisciplinary, evidence-based wound infection prevention and treatment guideline. Ostomy Wound Manage. 2017;63(11):18–29.
About the Author
Kathy is the co-developer and coordinator of the Acute Surgical Wound Service at Christiana Care Health Services. She advocates a team approach along a continuum of care from inpatient to surgery to outpatient. Her concentration has been traumatic wounds and addressing the individualized needs of those affected. She continues to harmonize patient care after discharge to skilled nursing/rehabilitation facilities and home care.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.