Necrotizing Fasciitis: When A Harmless Bug Turns Deadly
April 8, 2014
Part 4 in a series on infection management Part 1 | Part 2 | Part 3
Before you can delve into the vicious and deadly world of necrotizing fasciitis, the ghastly "flesh-eating disease" that's been widely reported by the media, you have to understand something about the bacteria that causes it and who is most susceptible to this rare condition.
Causes of Necrotizing Fasciitis
Here, the main culprit is a very common bacterium that may be harmlessly colonizing on your skin right now called Group A streptococcus (GAS). Often, though, necrotizing fasciitis is a combination of bacteria including klebsiella, clostridium, E. coli, staphylococcus aureus, and aeromonas hydrophila. On first reading that GAS is colonizing on your skin, one might wonder why necrotizing fasciitis is so rare a condition. The answer is that your body has been manufacturing antibodies since day one to protect you from any problem Group A Streptococcus can cause.
 Normal Skin
Normal Skin
Essentially, GAS is a benign colonizer that can occasionally cause mild skin infections such as impetigo or throat infections such as strep and pharyngitis. The bacteria spread and multiply quickly, but with conservative antibiotic therapy, the infection is resolved quickly. However, when the host's immune system is compromised and/or the strain of GAS (plus any of the other bacteria mentioned above) is particularly virulent, more intensive medical intervention is required.
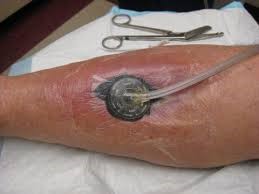
In these rare cases, the GAS bacteria can travel to the deeper layers of skin and subcutaneous tissues where it spreads quickly along the fascia, which are the connective tissues that cover muscles. There, they release toxins that speed up the rate of infection dramatically, leaving dead, necrotic tissue in their wake. That’s necrotizing fasciitis, aka, the "flesh-eating disease."
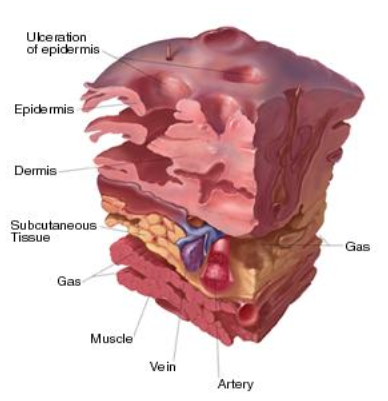 Necrotizing Fasciitis
Necrotizing Fasciitis
The "Flesh-Eating" Fallacy
But "flesh-eating" is a misnomer, as the bacteria do not actually "eat" the tissue, but release toxins including streptococcal pyogenic exotoxins that hyper-accelerate the spread of the infection. Until recently, scientists had no idea what turned the harmless bug, GAS, into deadly necrotizing fasciitis. But in recently published research (January 2014) conducted jointly by the Hebrew University of Jerusalem and the National University of Singapore, a new mechanism has been discovered that reveals how necrotizing fasciitis operates in early stages of the infection. Researchers found that when GAS sticks to and infects the host's cells, it delivers into these cells two streptolysin toxins. These poisons impair the body's mechanism for quality control of protein synthesis, allowing the invasive GAS to proliferate dramatically, much faster than the host can manufacture antibodies to fight them.
Treatments for Necrotizing Fasciitis
At that point, the main treatments include intensive intravenous antibiotics and surgical removal of infected tissues. Still, even after those modalities are promptly implemented, bacteria can still succeed in proliferating and cause death in approximately 25-30 percent of patients. That's why necrotizing fasciitis is one of the more vicious and deadly diseases. And, what makes it so ghastly are the disfiguring surgical excisions, amputations and scarring patients are left with if they survive.
There is optimism, though, in the recently published research. The team that did the studies discovered that asparaginase, a popular chemotherapeutic agent FDA-approved for lymphoblastic leukemia, stops GAS growth in human blood and in an animal model of human bacteremia. That may mean that it’s possible that asparaginase may also be applied to treat GAS infections resulting in necrotizing fasciitis. Hyperbaric oxygen therapy is also an FDA- and Medicare-approved modality to combat the disease. In addition, a product called NeutroPhase, a 0.01% pure hypochlorous acid saline solution with no bleach impurities, has been shown in extensive in vitro testing to kill bacteria in seconds and has the ability to neutralize toxins generated by GAS. The key to all the possibilities in treating necrotizing fasciitis is early detection because patients diagnosed with the condition have an ongoing emergency that doesn’t end until all the toxins released by the bacteria are gone.
About the Author
Dr. Bruce Ruben is the Founder and Medical Director of Encompass HealthCare, located in West Bloomfield, Michigan. Encompass Healthcare is an outpatient facility featuring advanced wound care, IV antibiotic therapies, hyperbaric oxygen treatment, nutritional assessment, and other treatment modalities. Dr. Ruben is board certified in Internal Medicine, Infectious Disease, and in Undersea and Hyperbaric Medicine. He is a member of the Medical and Scientific Advisory Committee and National Spinal Cord Injury Association (NSCIA) board.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.