Pressure Injury/Ulcer Risk Assessment: A Patient-Centered Approach
October 31, 2018
The goal of pressure injury/ulcer prevention is not only to maintain skin integrity but also to provide a patient-centered plan of care geared toward positive outcomes. This includes seeing your patient as a person, as well as identifying the patient’s pressure injury risks. Caregivers of any kind should learn to take steps in the prevention of pressure injuries/ulcers. We can utilize every risk assessment and tool known, but without educating our patients, health care professionals, and caregivers, a prevention program will not be successful. And let’s not forget that pressure injuries/ulcers can occur in patients of any age, at any weight, and in any type of setting. Most people think nursing homes are to blame when they hear the terms pressure ulcer, pressure injury, sore, decubitus, and bedsore. As clinicians, we tend to focus on the patient groups we take care of. Pressure injuries/ulcers are, most of the time, preventable.
Develop a Comprehensive Pressure Injury Risk Management Program
Developing specific policies and procedures related to pressure injury prevention and treatment will provide a strong, structured prevention program. Using a validated risk assessment tool such as the Braden Scale for Predicting Pressure Sore Risk® or Pressure Ulcer Scale for Healing (PUSH) tool is imperative for predicting pressure injury/ulcer risk. Risk assessment tools and frequency used vary by health care setting. For example, long-term care facilities may screen for pressure injury/ulcer on admission, readmission, change in condition, and with each minimum data set (MDS) 3.0 assessment.1 Your facility should have an algorithm in place for prevention and treatment of pressure injuries/ulcers. Here are a few questions to ask yourself when evaluating your risk assessment process.2
- Do you have interventions in place that can be immediately implemented for patients with low, moderate, and/or high risk of pressure injury/ulcer development?
- Do you have the necessary equipment to implement these interventions, such as redistribution mattresses, offloading heel devices, seat cushions, positioning devices, turning pads/slings for bariatric patients, etc.?
- Do you have a protocol for patients with medical devices? These patients should be considered high risk.
- Do you have daily, weekly, or monthly skin checks at your facility?
The Pressure Injury Risk Assessment Tool Focus
The following items detail common risk factors for developing pressure injuries/ulcers and contain interventions to help prevent the injury/ulcer from developing.1
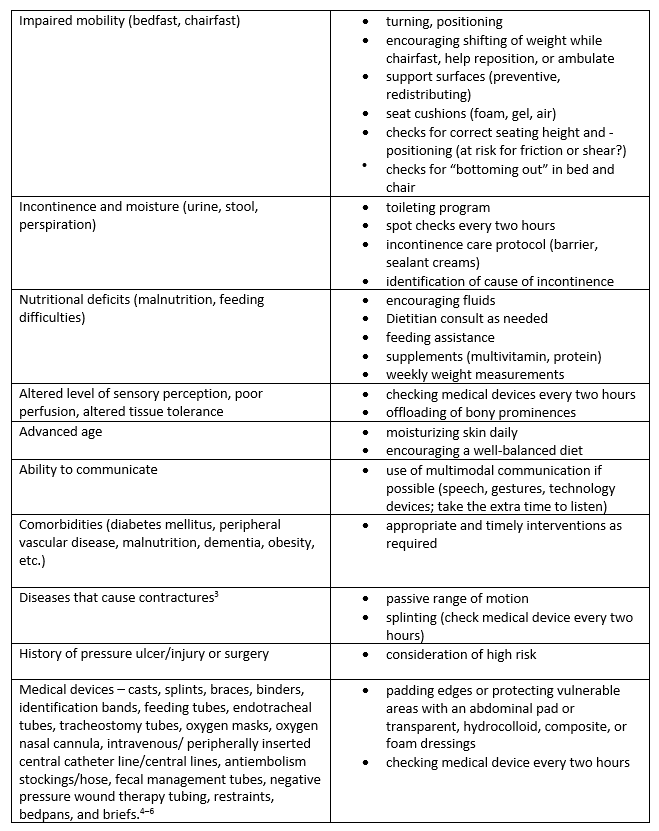
Conclusion If we are proactive with our assessments, we can help prevent the development of pressure injuries/ulcers. Health care providers can help improve patients’ outcomes, reduce complications, and control costs. Listen to your patients, and work together to plan their care. The goal is to reduce pressure injury/ulcer incidence entirely.
References
1. CMS MDS 3.0 RAI Manual. Centers for Medicare & Medicaid Services. https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Ins…. Accessed October 24, 2018.
2. Agency for Healthcare Research and Quality. Preventing pressure ulcers in hospitals. A toolkit for improving quality of care. https://www.ahrq.gov/sites/default/files/publications/files/putoolkit.p…. Accessed on October 7, 2018.
3. Skalsky AJ, McDonald CM. Prevention and management of limb contractures in neuromuscular diseases. Phys Med Rehabil Clin N Am. 2012;23(2):675–87.
4. National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel, Pan Pacific Pressure Injury Alliance. Prevention and treatment of pressure ulcers: clinical practice guideline. 2014. http://www.npuap.org/resources/educational-and-clinical-resources/preve…. Accessed on October 7, 2018.
5. National Pressure Ulcer Advisory Panel. The unavoidable outcome: a pressure injury consensus conference. J Wound Ostomy Continence Nurs. 2014;41(4):1–22.
6. Cock K. Anti-embolism stockings: are they used effectively and correctly? Br J Nurs. 2006;15(6):S4–12.
Suggested Reading
Centers for Medicare & Medicaid Services. CMS MDS 3.0 RAI manual. https://cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instrum…. Accessed September 21, 2018.
National Pressure Ulcer Advisory Panel. Pressure injury prevention points. http://www.npuap.org/wp-content/uploads/2016/04/Pressure-Injury-Prevent…. 2016. Accessed September 21, 2018.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










