Weird Wounds Part 1: Pyoderma Gangrenosum
March 2, 2020
"The world of the weird... wounds that are zebras rather than horses."
When I was in my APRN program, a phrase that I heard from an instructor has stuck with me throughout my practice: "When it comes to diagnosing, if you hear hooves, think horses, not zebras." Essentially, think of the obvious or likely reason first before jumping to a more obscure diagnosis. In the large majority of cases, the more common ailment is likely the cause. But what happens if the symptoms just don't quite add up? Or the treatment you prescribe, which should show some improvement, just doesn't? There are a lot of reasons people develop chronic wounds, which may be difficult to heal, but if you end up seeing a patient whose wound simply doesn't respond to conventional treatment, it may be time to think zebras. In this six-part series, we will discuss some of the more unusual wounds that you may periodically encounter. This will include a discussion on pyoderma gangrenosum, calciphylaxis, necrobiosis lipoidica, Marjolin ulcers, pemphigus, and sickle cell ulcers.
Part 1: Pyoderma Gangrenosum: The Painful Ulcer
Hypothetical Case Imagine this: It's a Wednesday morning at 8:30; you have seen two pretty routine follow-ups, and you look at your schedule to see that your next patient is new. While you sip your coffee (still warm, so it's a good day!), you give her chart a quick review before going into the room, and her history seems fairly benign.
"Patty" is a 46-year-old woman whose medical history is significant only for rheumatoid arthritis, for which she takes over-the-counter non-steroidal anti-inflammatory drugs as needed. She presented to her primary care physician (PCP) two weeks ago with a concern about two small, painful, pink bumps that had formed on her leg. She stated that she bumped her leg on a table at this site, but otherwise denied recent trauma or illness. She was started on an oral antibiotic, but the bumps grew and opened, and the pain increased.
With this in mind, you knock on the door of the exam room and enter. You notice right away that the Patty appears to be uncomfortable and is protective of her right leg by holding it close to her body. You introduce yourself to her and review her history, which is consistent with the documentation you had reviewed.
She mentions that she doesn't smoke, drinks only on rare social occasions, and hasn't traveled anywhere recently. It is currently winter, and you live in a northern climate, and she denies recent insect bites. She tells you that her arthritis has been stable, and she needs to take ibuprofen only periodically. She is active, works full time, and lives at home with her husband and two grade-school aged children. Her vital signs are normal, but she rates the wound pain as a six out of 10, "and I usually have a pretty high pain tolerance." She has been managing the wounds with gauze dressings and an over-the-counter antibacterial ointment, and she has been elevating her legs when she can. During the exam, you note that her legs are normal flesh-toned, have normal hair distribution, and have no significant edema. Her feet are warm, with good pedal pulses and capillary refill.
She has two irregularly shaped ulcers on the lateral surface of her right lower leg. The wound margins are slightly raised and jagged in appearance and have a purplish border. The wound bed is moist and dark red with 10% to 20% thin, yellow slough scattered at the base. There is a circumferential erythemic halo at the periwound. Gentle palpation of the skin near the wound elicits a dramatic painful response, as the patient yelps and draws her leg away from you. She tells you that it is so tender that she can hardly bear wearing socks or pants as this irritates the wounds and is very painful.
She mentioned that her PCP had initially suggested trying compression socks, but they were too painful to wear. These wounds are odd; they don't strike you as being vascular. They could be infectious, but she showed no response to the antibiotic. You take a culture to rule out infection. There is slough present, which you would normally try to debride; however, the pain of the wound is so significant that she doesn't let you touch it.
You order ankle-brachial index (ABI) tests to ensure it isn't arterial and recommend treatment with calcium alginate with gauze daily and ask her to follow up with you in a week. When she returns to you, the culture showed normal skin flora, and the ABI was normal. Despite the daily application of the alginate dressing, the wounds have grown, have developed more slough, and have become even more painful. This is the kind of wound that makes you step back for a few minutes and think about what might have caused the wound to form. Patty's history is significant only for an autoimmune condition.
She is an otherwise healthy woman without underlying vascular disease or infection. The one thing you keep going back to is the biopsy. Was it possible that she had an underlying cancerous growth that was missed? You review the pathology report; it reports normal epithelial cells. This is a stumper of a diagnosis. This is a case of exclusion; a wound of the weird: pyoderma gangrenosum (PG).
Overview of Pyoderma Gangrenosum
Pyoderma gangrenosum is a rare wound that you may encounter a few times in your career. PG is diagnosed once all other possibilities have been eliminated or dismissed; it's a diagnosis of exclusion. It was first described in 1916, and at that time, the etiology was unknown,1 although it was thought to be infectious, hence the name "pyoderma" or "purulent skin disease." The exact cause is still unknown; however, it is thought to be a disease of autoimmunity and not infection.
It does not respond to antibiotics and is considered a rare inflammatory skin condition that is diagnosed in approximately three out of 1 million people.2 There are no specific lab tests, but other conditions such as skin lymphoma or tumors, vascular disease, and infection should be ruled out. Because it is so rare, it may be easily overlooked, and without appropriate treatment, the results can have terrible effects on the patient. It most commonly occurs in people ages 40–60 and is more common in women, and about 50% of these patients have another underlying autoimmune disorder, such as arthritis, inflammatory bowel disease, ulcerative colitis, or Crohn's disease.2
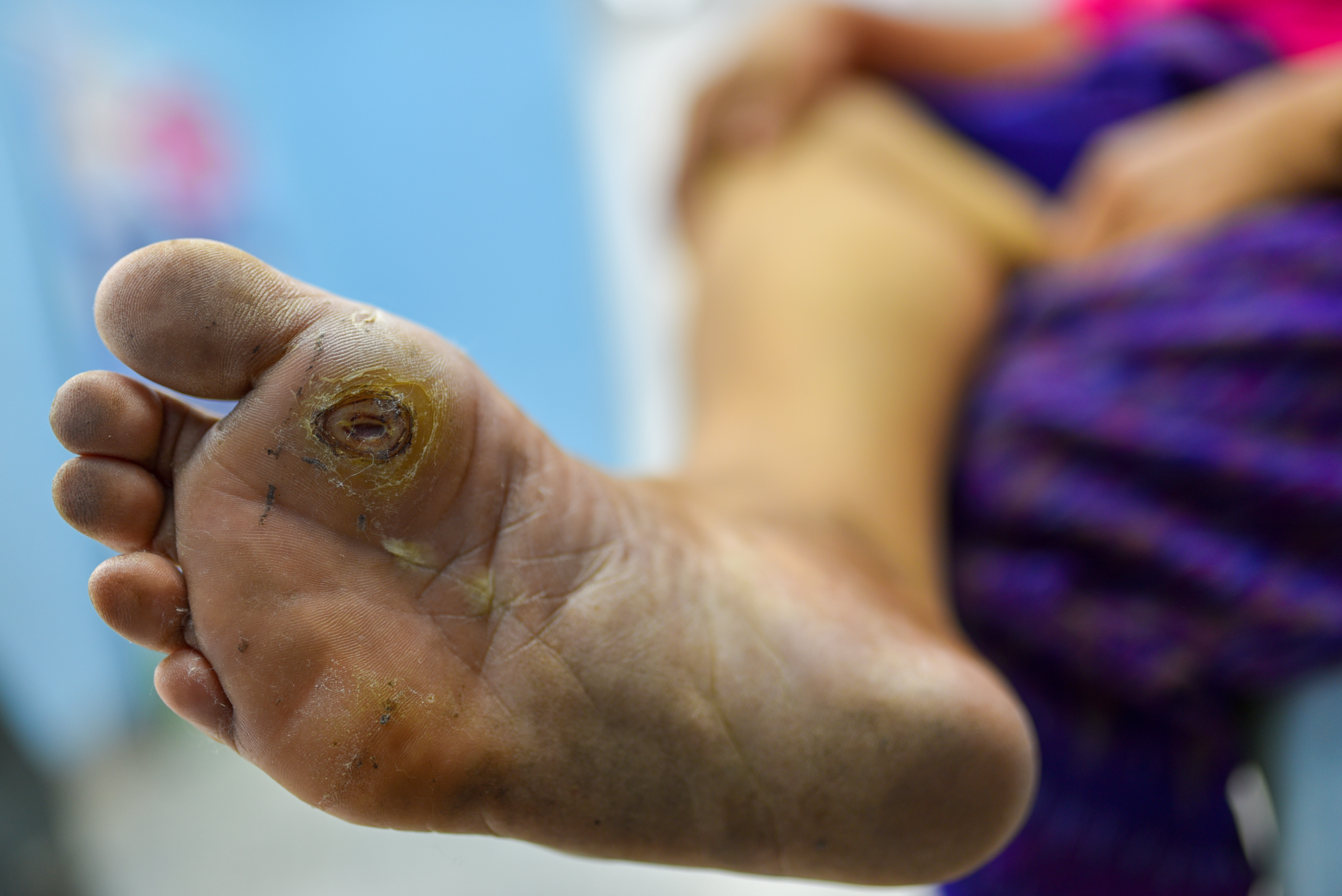
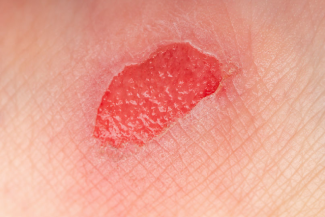
Onset is variable, but some cases of PG have been known to occur following minor skin trauma or surgery (which may be as minor as a skin biopsy). The wounds typically start as small, painful bumps that can quickly progress to large, painful ulcerations in the matter of a few days. The ulcers most commonly develop on the lower legs, but they may also form around stomas, on the dorsal surface of the hands, the extensor surface of the forearms, or the face. The wounds are extremely painful and have an irregular shape with purplish or bluish color at the margins.
There is often a halo of erythema surrounding the wound. When the wound starts to heal, you may see string-like projections of new skin starting to grow along the border of the ulcer bed and the skin.2 Once healed, the site may have a cribriform scar.
Hypothetical Case, Continued
In our case, Patty is a middle-aged woman with an autoimmune disease, which puts her at greater risk for developing PG. Her biopsy likely exacerbated this and caused the wounds to develop. She didn't respond to the antibiotics, as PG doesn't represent an infectious process. She had no signs of vascular disease and mentioned that attempting to put on compression socks was too painful to tolerate. Once you diagnose Patty with PG, what should you do? If you suspect PG, don't attempt sharp debridement of the wound. Not only is this very painful, but it can actually aggravate the wounds, causing them to degenerate further.
Systemic corticosteroids are recommended; however, patients with severe cases may need to be hospitalized for several days to receive intravenous methylprednisolone. Moderate cases could be treated on an outpatient basis with 40–60mg/day of oral prednisone with appropriate wound dressings, such as an alginate, foam, hydrocolloid, or silver sulfadiazine. Dressings that contain methylene blue and crystalline violet have been shown to be particularly helpful in patients with PG wounds.1
Wounds that are covered in slough should be managed with an enzymatic debrider. Smaller PG wounds may respond to topical steroids. Pain can be significant, so a good pain management plan is an important step. If you start to see a decrease in pain and an improvement in erythema at the wound edge and overall improved dimensions, you know that you're on the right track. At this point, you could slowly start to taper the steroids as tolerated. Once healed, there can be scarring at the site of the wound. This can be minimized by prompt recognition and treatment of PG. Unfortunately, patients may have recurrent episodes of PD, so follow-ups with rheumatology consultation should be incorporated into their care plan to ensure good management of their underlying autoimmune condition.
Conclusion
Pyoderma gangrenosum is an unusual type of wound that may surprise you, but with a bit of testing and sleuthing, you may just find it to be quite manageable.
References
1. Pompeo MQ. Pyoderma gangrenosum: recognition and management. Wounds. 2016;28(1):7-13. https://www.woundsresearch.com/article/pyoderma-gangrenosum-recognition…. Accessed March 1, 2020.
2. Gameiro A, Pereira N, Cardoso JC, Gonçalo M. Pyoderma gangrenosum: challenges and solutions. Clin Cosmet Investig Dermatol. 2015;8:285-293. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4454198/. Accessed March 1, 2020.
About the Author
Becky received her BSN from the University of Vermont where, along with a love of nursing, she picked up a love of hiking and cross-country skiing. She moved to Massachusetts and started to work as a med-surg nurse at a busy Boston hospital. There, she found that she loved mentoring new nurses and returned to school to earn her MSN as an acute care clinical nurse specialist from the University of Massachusetts, Boston. She followed her love of teaching into the acute, sub-acute and university settings, but she found that she missed working directly with patients. She returned to school and earned her Post-Master's Family Nurse Practitioner Certification from Rivier University. It was shortly after this that Becky discovered her love for wound care. She worked part time in wound care and part time in family care while she earned her WCC certification. After several years, Becky decided to take her practice to the next level by opening her own LLC and is currently seeing patients for wound care and regenerative medicine. Becky's philosophy of “Never stop learning” has guided her in her practice and life. Her very supportive husband and daughter are her key inspirations to keep growing and trying new things. In her spare time, Becky loves traveling with her family, going on long walks with her dog, Echo, and reading historical and science fiction.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.