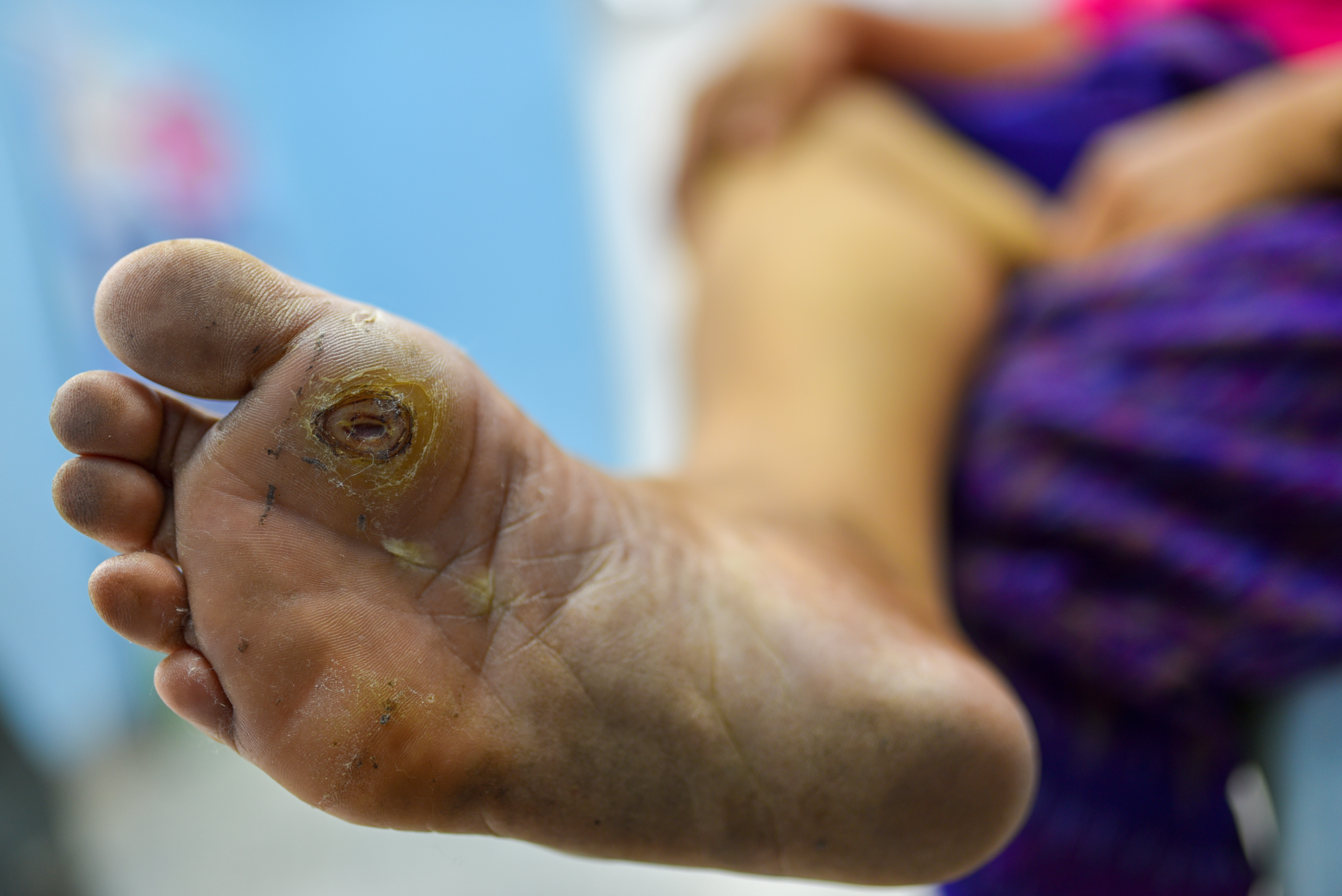
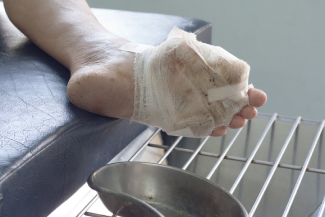
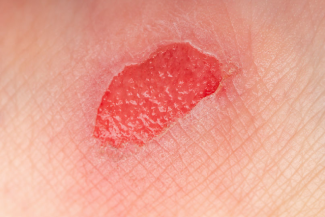
Weird Wounds Part 3: Hidradenitis Suppurativa – "Boils Gone Wild"
May 28, 2020
If you've ever had a painful red bump after shaving, you've probably chalked this up to razor burn or an ingrown hair. After an irritating day or so, the bumps will likely fade and disappear on their own, and you don't give it any more thought. But what if these bumps just kept growing and became more and more painful? And even worse, what if they developed in sensitive areas such as the axilla or the groin?
What if these bumps got so bad, they eventually opened, started to drain, and even formed tracts under the skin? Not only are these bumps painful, but they are also embarrassing. Forget about wearing a sleeveless shirt or bathing suit in the summer. Would people think you had a horrific contagious disease? You go to doctor after doctor, but no one has been able to treat this successfully. The bumps may disappear for some time but then suddenly reappear. They may leave scars that seem to open and close persistently, and at times they may become infected, requiring antibiotic therapy. Finally, you get the diagnosis for this awful condition: hidradenitis suppurativa (HS).
What Is Hidradenitis Suppurativa?
Also known as acne inversa, HS is a skin condition that occurs in roughly 4% of people.1 It is characterized by painful breakouts that most commonly occur in areas of the body where the skin may rub against itself and have more sweat or oil glands, such as the axilla, groin, anus, inner thighs, buttocks, and under the breasts. It typically may manifest in teens and last throughout the life span, and it may initially look like a black-head pimple or a small, pea-shaped, painful lump under the skin. Over time, multiple bumps may cause tracts under the skin.
Weird Wounds Part 2: Calciphylaxis – "The Heart Attack of the Skin"
The cause is not generally understood; however, some investigators speculate that the bumps may appear when a hair follicle becomes blocked, causing increased swelling and pain. HS is thought to be a genetic disease because roughly one third of those affected also have a first-degree relative who is also affected.1 HS was originally thought to be a disorder of the sweat glands, but more recent research has implicated a defect in the basement membrane of the apocrine glands of the skin that causes hyperkeratinization and chronic biofilm colonization.1 HS can be exacerbated by hormonal fluctuations and increased periods of stress. Metabolic diseases, such as diabetes, have been linked to an increased likelihood of occurrence, particularly if blood glucose concentrations are poorly controlled.
Obesity may increase outbreaks because of increased skin rubbing at predisposed sites, and smoking has also been linked to increased outbreaks in patients diagnosed with HS. Exposure to excessive heat may trigger outbreaks. Other risk factors can include concurrent diagnosis with acne, arthritis, Crohn's disease, or inflammatory bowel disease.2 Common complications of HS can include infection of the lesions, fistulas that track under the skin and may require surgery, and scarring that can lead to tough, pitted skin that may restrict movement (particularly when the sites are at the axilla and upper thighs).
Although rare, some patients with advanced HS may develop squamous cell carcinoma at sites of breakouts or scarring. Scarring may cause impaired lymph drainage if scar tissue impedes the lymph nodes at the axilla or groin. One of the most difficult to treat complications of HS is the very real sense of isolation that can develop. This can become a serious problem as a result of the chronic open, draining sores and scars, which can lead to embarrassment, depression, and reluctance to participate in social engagements.
Treatment of Hidradenitis Suppurativa
Treatment for HS is generally preventive and supportive during outbreaks. Patients with HS may be able to prevent outbreaks by managing biofilm, preventing follicular occlusion, and improving overall hormonal function and balance. Management of underlying metabolic and autoimmune disease, smoking cessation, and maintenance of a healthy weight can go a long way to help reduce recurrent episodes.
Some traditional therapies have included antibacterial washes (such as with benzoyl peroxide), topical clindamycin 1%, and systemic retinoids for active lesions. Intralesional steroid injections with triamcinolone acetonide can help reduce inflammation. Topical application of ketoprofen can be helpful in managing the pain that is associated with these lesions.3 Systemic antiandrogen therapy with spironolactone has been shown to be more effective than antibiotics in treating outbreaks. Newer research with laser treatment has shown promising results in decreasing inflammation, fibrosis, and scarring.4 Surgery may be performed to de-roof lesions, although this does not prevent recurrence.
Healing of Hidradenitis Suppurativa
Healing of HS ulcers requires returning to the ABCs of wound care: managing bioburden, maintaining a moist wound healing environment, and ensuring that any comorbidities are managed. Wounds should be treated on the basis of moist healing principles; dressings such as hydrofiber, alginate, foam, and honey can all help create a favorable healing environment. Platelet-rich plasma has been shown to be very beneficial in triggering a healing response. If appropriate, using a wound vacuum with negative pressure may be used to stimulate angiogenesis and increase tissue perfusion.3
Conclusion
HS is a challenging health condition that can have significant physical and psychological impacts on affected patients. It is important to reassure the patient that the ulcers have nothing to do with the person being "dirty" and that they are not contagious. It is not their fault, and the disease can be managed. There are many support groups online for HS, and they may provide psychological reassurance that these patients are not alone:
- Hidradenitis Suppurativa Foundation, Inc: https://www.hs-foundation.org/support/
- No BS about HS: https://www.nobsabouths.com/
- Multiple Facebook support groups: https://www.facebook.com/HidradenitisSuppurativaSupportGroups/
- Hope for HS: https://hopeforhs.org/
References
1. Gill L, Williams M, Hamzavi I. Update on hidradenitis suppurative: connecting the tracts. F1000 Prime Rep. 2014;6:112. https://f1000.com/prime/reports/m/6/112. Accessed April 21, 2020.
2. Hidradenitis Suppurativa Foundation. What is hidradenitis suppurative? https://www.hs-foundation.org/what-is-hs/. Accessed April 21, 2020.
3. Dini V, Oranges T, Rotella L, Romanelli M. Hidradenitis suppurativa and wound management. Int J Low Extrem Wounds. 2015;14(3):236-244. https://www.researchgate.net/publication/280869471_Hidradenitis_Suppura…. Accessed April 21, 2020.
4. Tierney E, Mahmoud BH, Hexsel C, Ozog D, Hamzavi I. Randomized control trial for the treatment of hidradenitis suppurativa with a neodymium-doped yttrium aluminium garnet laser. Dermatol Surg. 2009,35:1188-1198. https://f1000.com/prime/reports/m/6/112/#bib-036. Accessed April 21, 2020.
About the Author
Becky received her BSN from the University of Vermont where, along with a love of nursing, she picked up a love of hiking and cross-country skiing. She moved to Massachusetts and started to work as a med-surg nurse at a busy Boston hospital. There, she found that she loved mentoring new nurses and returned to school to earn her MSN as an acute care clinical nurse specialist from the University of Massachusetts, Boston. She followed her love of teaching into the acute, sub-acute and university settings, but she found that she missed working directly with patients. She returned to school and earned her Post-Master's Family Nurse Practitioner Certification from Rivier University. It was shortly after this that Becky discovered her love for wound care. She worked part time in wound care and part time in family care while she earned her WCC certification. After several years, Becky decided to take her practice to the next level by opening her own LLC and is currently seeing patients for wound care and regenerative medicine. Becky's philosophy of “Never stop learning” has guided her in her practice and life. Her very supportive husband and daughter are her key inspirations to keep growing and trying new things. In her spare time, Becky loves traveling with her family, going on long walks with her dog, Echo, and reading historical and science fiction.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.