Choosing Antimicrobial Wound Dressings
December 31, 2020
Prevention and management of biofilm and infection in wounds can be supported by using antimicrobial and antibiofilm dressings. Internationally, there has been a rising prevalence of antibiotic-resistant organisms; this has resulted in increased incorporation of antimicrobial dressings in wound management.
These dressings offer many advantages because they are easy to use, are readily available, have a decreased risk of resistance, and deliver sustained release of antimicrobial agents to the wound bed. This mode of action allows for a lower concentration of the agent and thereby lowers the possibility of toxicity to host cells. Clinicians should have practical knowledge of the various dressing technologies and formulations of antimicrobial and antibiofilm advanced wound care dressings. It is also imperative during dressing selection to know the different dressing properties, costs, and effectiveness. Clinicians should be confident in identifying hard-to-heal wounds, as well as knowing when to start and stop antimicrobial or antibiofilm treatments.1 Sequential debridement by itself is unlikely to prevent regrowth of biofilm because of rapid biofilm re-formation; therefore, antimicrobial dressings can help address residual biofilm and its re-formation after biofilm disruption.2
Antimicrobial Dressings
The term “antimicrobial” is used as an umbrella term that encompasses disinfectants, antiseptics, and antibiotics. Antimicrobial activity occurs in disinfectants and antiseptics but varies. Recent antimicrobial technologies have developed non-cytotoxic formulations to be less harmful to healthy wound tissue while remaining effective in dismantling pathogens. Many dressing technologies and formulations are available, including dressings that utilize substances with antimicrobial or antibiofilm capabilities such as silver, cadexomer iodine, polyhexamethylene biguanide, medical-grade honey, and others.
How much do you know about infection management? Take our 10-question quiz to find out! Click here.
Clinicians who are selecting dressings may come across the terms “antimicrobial,” “antiseptic,” and “disinfectant.” These terms describe what the dressing is used for, and it is important to know the differences among these types.
- Antimicrobial agents kill microorganisms.
- Antiseptics are broad-spectrum biocides used to inhibit or kill microorganisms present on skin or within a wound; resistance to antiseptics is uncommon.
- Disinfectants are broad-spectrum chemical agents or biocides that inhibit or kill microbes on objects; microbial resistance is uncommon.
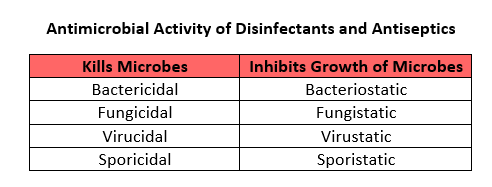
Additionally, clinicians should be familiar with the suffixes “-icidal” and “-static.” These prefixes describe goal of the substance, with “-icidal” being to kill microbes and “-static” to prevent the growth of microbes.
There continues to be controversy regarding topical antimicrobial agents because of reports of cytotoxicity. Providers should make evidence-based decisions.3 Highly cytotoxic agents include povidone-iodine and hydrogen peroxide.2 However, comparison studies have shown that cytotoxic agents diluted with saline solution are effective in killing gram-positive and gram-negative bacteria but are not harmful to normal fibroblast cells. This method continues to be used in practice, thus providing a balance between bactericidal and cytotoxic effects while being a lower-cost measure.4 When performing wound hygiene on hard-to-heal wounds, use surfactant-containing antiseptics or pH-balanced solutions in the wound and on the skin. Antiseptic cleansers used in wound healing include polyhexamethylene biguanide, hypochlorous acid, and chlorhexidine gluconate.2 Cleansing the wound bed and periwound will help promote a balanced wound bed environment for healing. Biofilm may be harbored in both the wound and the wound edges.2
Factors to Consider in Wound Dressing Selection
There is a multitude of antimicrobial dressings on the wound care market. How do you know which dressing to choose? Consider dressing selection to be as vital as the wound assessment. Dressing selection goals should be to address any residual biofilm and to prevent and manage biofilm regrowth. Antimicrobial dressings have different antimicrobial activity, delivery systems, absorbency capabilities, wear time, shapes, and sizes. Dressings may also offer sustained release of antimicrobial agents, with time frames generally ranging from two to seven days. Clinicians should also remember to select dressings that manage exudate and maintain an optimal moist wound environment.
Antimicrobial Dressing Categories
Antimicrobial dressings come in a variety of dressing formats, including alginate, collagen, foam, gauze, gelling fiber, hydrogel, and transparent dressings, as well as wound contact layers. Clinicians should assess or evaluate the wound during each dressing change to ensure that the wound is making healing progress. Assess the wound and the effectiveness of the current dressing every two to four weeks to evaluate whether the dressing should be stopped or continued. In wounds that are showing healing progress, continue to cleanse, debride, and refashion the wound edges, and consider whether to switch to a non-antimicrobial dressing.
Conclusion
Dressing selection should be part of an overreaching plan of care that includes wound hygiene. The wound and periwound should be cleansed at every dressing change, followed by debridement, refashioning of wound edges, and selection of an appropriate antimicrobial dressing to prevent and manage residual biofilm. Although many advanced wound dressings are available, understanding what the wound you are treating needs to progress toward healing will simplify dressing selection.

References
1. Antimicrobials made easy. Wounds Int. 2011;2(1). https://www.woundsinternational.com/download/resource/6086.
2. Murphy C, Atkin L, Swanson T, et al. International consensus document. Defying hard-to-heal wounds with an early antibioflm intervention strategy: wound hygiene. J Wound Care. 2020;29(Suppl 3b):S1-28.
3. Cooper R. A review of the evidence for the use of topical antimicrobial agents in wound care. World Wide Wounds. 2004. http://www.worldwidewounds.com/2004/february/Cooper/Topical-Antimicrobi…. Accessed December 13, 2020.
4. Rabenberg VS, Ingersoll CD, Sandrey MA, Johnson MT. The bactericidal and cytotoxic effects of antimicrobial wound cleansers. J Athl Train. 2002;37(1):51-54.
The views and opinions expressed in this content are solely those of the contributor, and do not represent the views of WoundSource, HMP Global, its affiliates, or subsidiary companies.










